Wednesday's health stories

Humana's profit engine: Medicare
Humana's stock jumped 4.5% Wednesday after the health insurance company more than doubled its second-quarter earnings to $650 million. Profit in the first half of the year was almost $1.8 billion, thanks in part to the termination fee Humana received from Aetna following their failed merger. Humana's market cap is now around $35 billion, which would make it harder for a competing insurer to buy it.
The bottom line: Humana's profit is growing like gangbusters because its primary health plan business, Medicare Advantage, coincides with the rapid aging of the country's baby boomers. Humana has almost 3.3 million people in one of its Medicare Advantage plans and another 5.2 million in its Medicare prescription drug plans.
Worth noting: Humana is ditching the Affordable Care Act's individual exchanges, but the company collected a $118 million profit from ACA plans in the second quarter.

Molina posts huge loss, will exit two states' ACA markets
Molina Healthcare lost $230 million in the second quarter this year — catching investors, who expected a slim profit, off guard. The Affordable Care Act exchanges wreaked havoc on the health insurer, which is pulling out of Utah and Wisconsin, pruning its participation in other states and laying off 7% of its workforce. Most of Molina's business is in Medicaid contracts with states.
The numbers: $230 million net loss, compared with a $33 million profit in the same period a year ago. Revenue increased 15% to $5 billion. Molina will cut expenses by up to $400 million by the end of next year — $55 million has already come from layoffs and restructuring.

Centene hires former HealthCare.gov chief
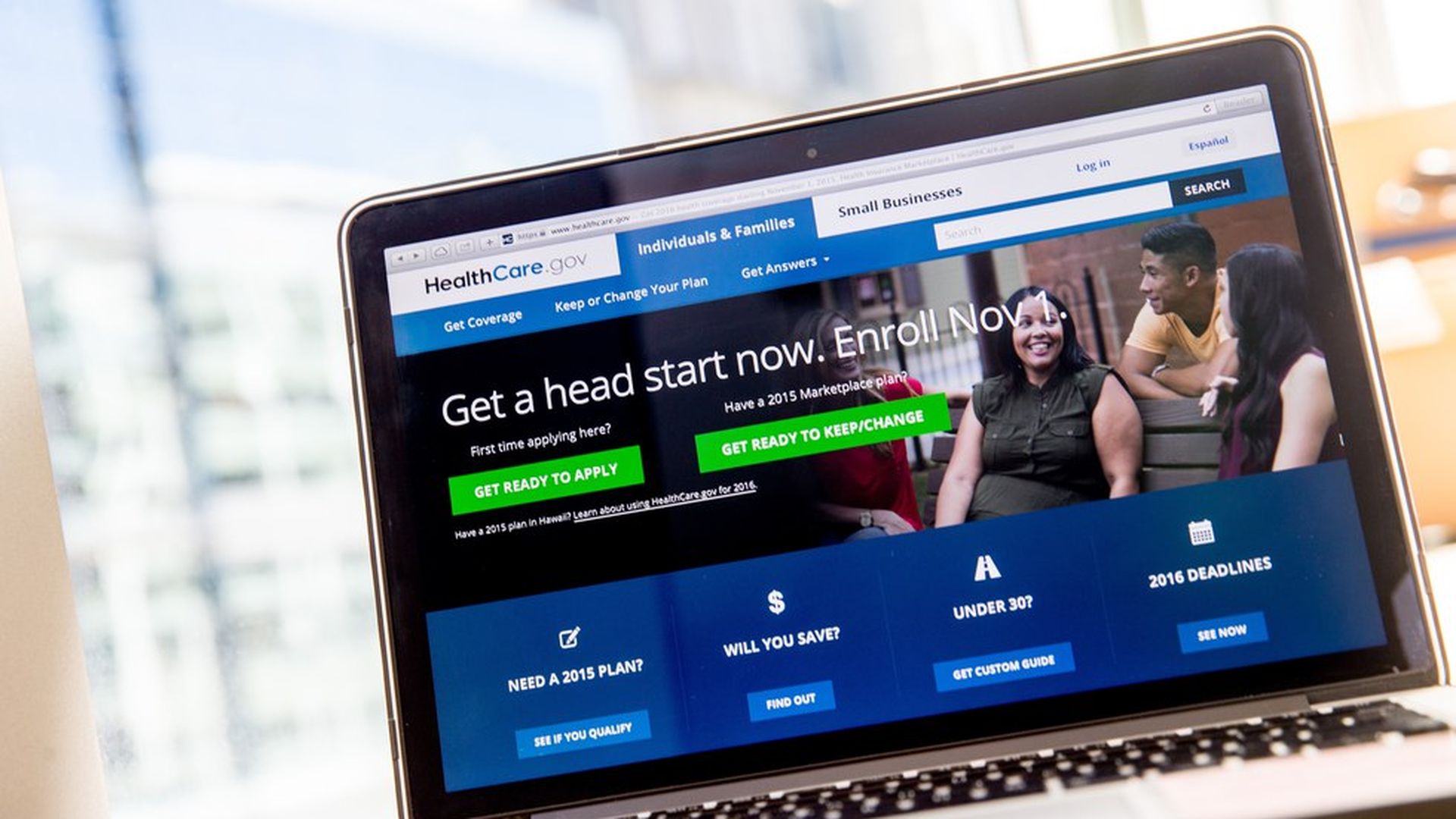
Kevin Counihan, the former head of the federal HealthCare.gov insurance exchange, has joined Centene, Vox reports. He will oversee Centene's health plans in the Midwest.
Why it matters: Counihan was an important Obama administration official — HealthCare.gov serves as the individual health insurance hub for 39 states that did not set up their own exchange. And now he's moving to Centene, which is mostly known for its Medicaid plans but has also embraced the ACA markets and is making a profit on those plans.

BCBS of North Carolina lowers ACA rate increases
Blue Cross Blue Shield of North Carolina will lower its average proposed rate hike on individual Affordable Care Act plans from 23% to 14%, the insurer said Wednesday. The medical costs of people in the ACA market are not expected to be as high, although uncertainty still remains around the law's cost-sharing reduction subsidies.
Key quote: "The individual market in North Carolina has become less volatile."
Go deeper: Many Blue Cross Blue Shield plans have started making money on ACA plans this year, as health insurance companies have finally gotten a grip on how to predict costs for this market. However, middle-income people who don't qualify for subsidies and buy outside the exchange are struggling with higher premiums.

Anthem prunes ACA plans in California
Anthem is leaving 16 of the 19 regions in California's Affordable Care Act insurance exchange for 2018, per Covered California. The for-profit Blue Cross Blue Shield giant also eliminated all of its HMO and PPO plans and will only sell "exclusive provider organization" plans, which are narrow networks of doctors and hospitals.
Yes, but: All 11 health insurers still plan on operating in California next year, and 82% of ACA shoppers will have at least three insurance options. Anthem's exit will affect about 150,000 people, but California's exchange has been robust enough to offer alternatives.
The headline numbers: Average ACA rates are expected to rise 12.5% in 2018. People with premium subsidies won't feel that rate bump much, but it's a large increase for middle-class people who don't get subsidies. Health plans also would add surcharges averaging 12.4% if cost-sharing reduction subsidies are nixed.

Map: Who loses if Trump cuts off health insurer payments
We could get a decision from Trump today on whether the administration will keep paying insurers for their cost-sharing reduction subsidies to low-income people. A few things to keep in mind if he stops the payments:
Data: Centers for Medicare & Medicaid Services; Map: Lazaro Gamio / Axios