New infertility definition could be "game-changer" for Oregonians
Add Axios as your preferred source to
see more of our stories on Google.

Illustration: Lindsey Bailey/Axios
A new, more expansive definition of infertility could lead to more resources for hopeful LGBTQ+ or single parents in Oregon.
Why it matters: While Oregon has one of the lowest fertility and birth rates in the country, the state does not require insurers to cover fertility treatment, despite multiple attempts by advocates and legislators.
Driving the news: A decision this month by an influential organization of reproductive health providers to redefine infertility could lead to broader insurance coverage of services nationwide — potentially pushing the needle in states like Oregon where attempts have stalled.
What's happening: The American Society for Reproductive Medicine (ASRM) previously defined infertility as the inability of a man and woman to get pregnant after a year of unprotected intercourse or intrauterine insemination. For women 35 and older, the time period is six months.
The group expanded its definition to now include:
- The inability to get pregnant because of the patient's medical, sexual and reproductive history, age, physical findings and diagnostic testing.
- The need for medical intervention such as using donor eggs or sperm to achieve pregnancy.
Between the lines: The updated language applies to anyone who needs help having children, regardless of relationship status, gender identity or sexual orientation.
What they're saying: A more inclusive definition of infertility — which ASRM considers a disease, condition or status — "could be a game-changer," Tracy Palmer, a Portland-based queer fertility advocate tells Axios.
- "Oftentimes as queer folks, we are not technically infertile, but we use all of the same methods to grow our family as those with a formal diagnosis," she said. "Without being included in the definition, we are often left out of the conversation."
Zoom in: A number of insurance plans rely on the ASRM definition of what's a disease to determine coverage. Some local advocates also hope the expanded definition will spur lawmakers to act.
- Paula Amato, a professor of obstetrics and gynecology at Oregon Health & Science University, told Axios she hopes Oregon lawmakers will now recognize that mandating fertility coverage is the "right thing to do."
- "Infertility is a disease and as such should be treated like any other," she said in an email.
Flashback: A bill that would mandate insurers within Oregon's health care marketplace cover fertility treatments has failed to move from committee hearings to a floor vote in the last three legislative sessions — even with bipartisan support.
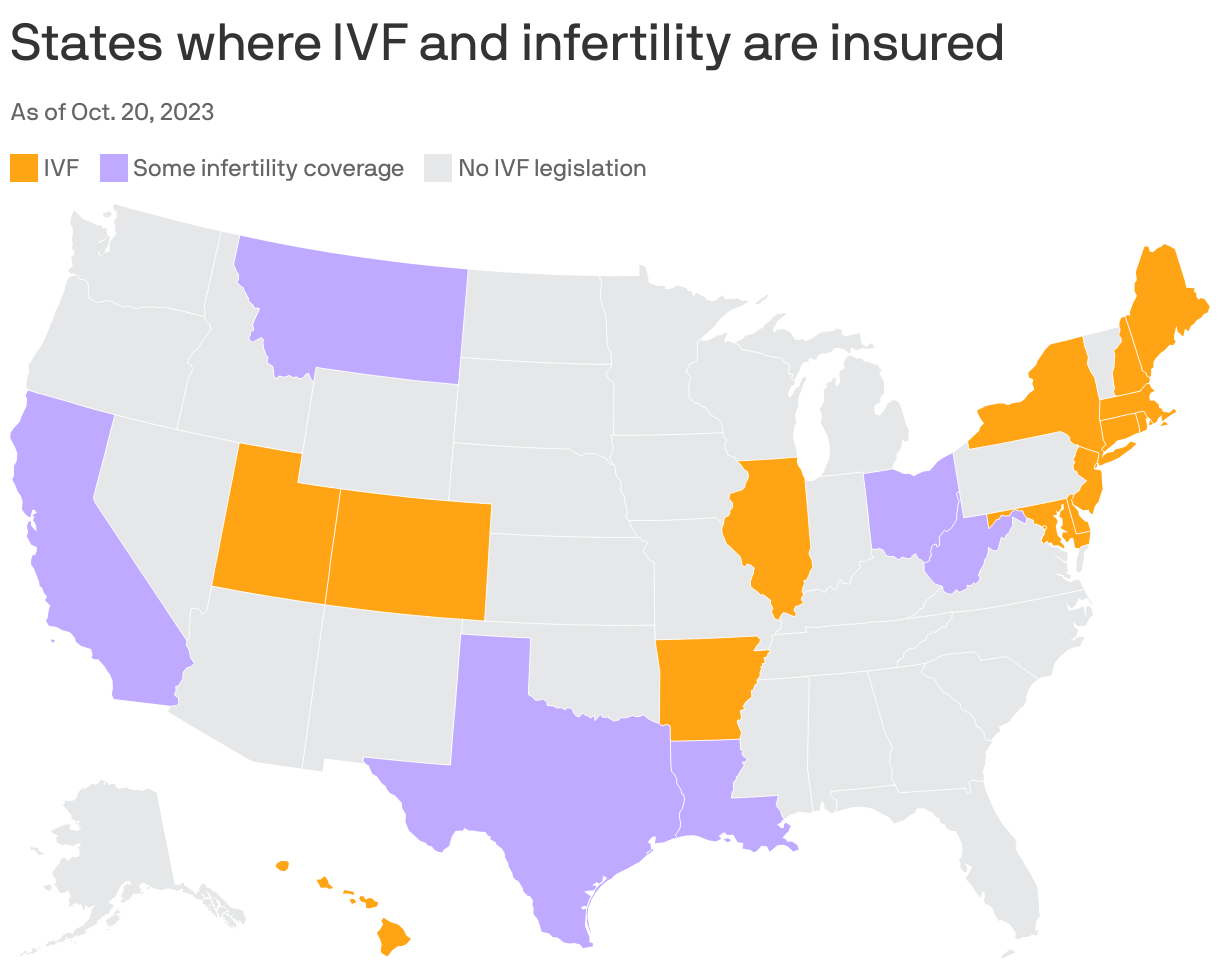
- Of note: As of now, 21 states plus D.C. require some workplace health plans to cover at least some form of fertility coverage, and of those, only eight states have policies that are inclusive of LGBTQ+ communities and single parents, according to Betsy Campbell, chief engagement officer at infertility advocacy group Resolve.
State of play: Despite the growing interest in fertility care — and more employers offering fertility benefits to stay competitive in the labor market — insurance coverage of the often-pricey services remains limited.
- Still, several studies suggest fertility insurance coverage does not significantly increase the cost of medical plans.
What's next: In an email, Oregon Fertility Advocates, a grassroots group pushing for pro-family legislation, said they plan to use the new definition as fuel to lobby lawmakers ahead of the next legislative session.

