Friday's health stories
ACA architect Max Baucus backs single-payer
Former Montana Sen. Max Baucus — a central architect of the Affordable Care Act who steered that bill toward the center and rejected multiple proposals for government-run insurance plans — now supports single-payer.
"My personal view is we've got to start looking at single-payer," Baucus, the Senate Finance chair during the ACA debate, said last night, according to the Bozeman Daily Chronicle. ""I think we should have hearings ... We're getting there. It's going to happen."
Why it matters: Baucus isn't in a position to make policy anymore, but he can still take the temperature of his party. Just eight years ago, he refused to even hold a hearing on single-payer. To say now that he not only supports it, but that he thinks it's inevitable, is a sign of just how dramatically Democrats are pulling to the left on health care.

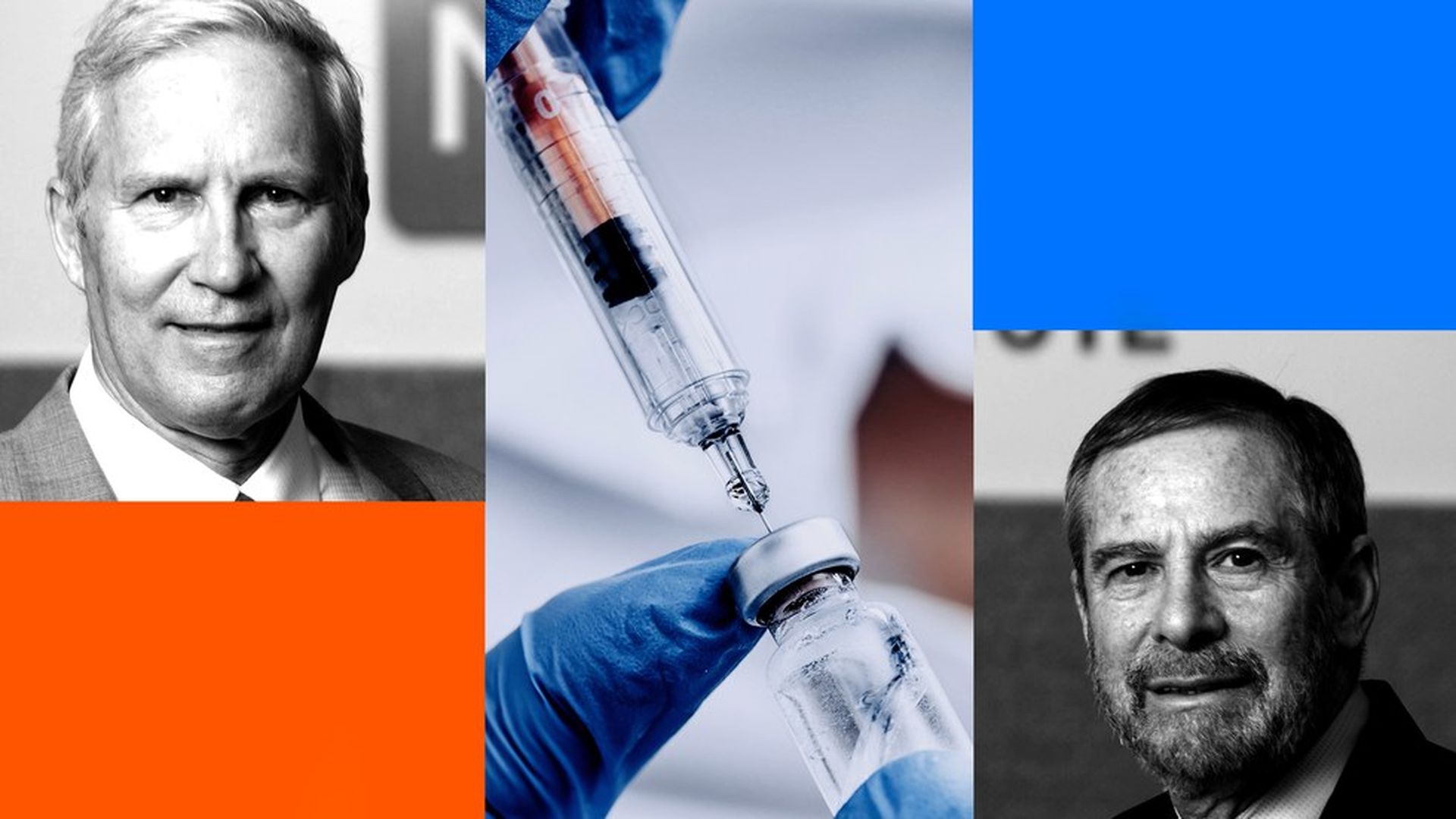
The cancer scientists behind the HPV vaccine win top medical prize
Douglas Lowy and John Schiller, scientists from the National Cancer Institute, will be presented the prestigious Lasker Award on Sept. 15 for their research that led to the development of human papillomavirus (HPV) vaccines. They're hopeful their approach could be used to produce more vaccines against other viral infections that cause cancers.
Why it's important: HPV vaccines are given to teens in an effort to thwart infections of the virus that can cause cervical and other cancers. While HPV is linked to cancers in both men and women, cervical cancer is one of its biggest possible consequences. More than 250,000 women die each year from cervical cancer worldwide, with the majority of cases happening in developing countries.
Schiller and Lowy, who is the acting NCI director, talked to Axios about the vaccine's use in the U.S. and cancer prevention efforts.

To get prime-age men back to work, get them off opioids
Opioid use may be responsible for a fifth of the record number of prime working-age American men who have chosen to fully drop out of the work force and no longer seek a job. In a new paper delivered at the Brookings Institution today, Alan Krueger, a professor at Princeton, described a strong correlation between high opioid use and low labor force participation among men 25 to 54 years old.
Where the correlation is highest: Here is a chart of Krueger's county-by-county study, showing the strongest impact in Mississippi, which has 10 of the top 25 counties on the list. Six are in Arkansas; and four each are in Alabama and North Carolina.

Putting a price on new cancer treatments
Last week, the FDA approved a new immunotherapy for treating a type of leukemia that affects children and young adults. The manufacturer, Novartis, expects it will cost about $475,000 for the one-time personalized treatment in which a patient's immune cells are removed, modified so they attack cancer cells and then infused back into the body. Other companies are working on similar therapies for other cancers —with tentative success and serious setbacks.
As these new drugs begin to enter the market, we asked researchers, economists and policy experts: how should their value be determined? Their answers:

The public should have a say in what a drug is worth
From our Expert Voices conversation on drug pricing.
Setting a "fair price" for a new drug is challenging but not impossible. Because we confer to manufacturers of new drugs a time-limited monopoly, the public has a legitimate claim to participating in the price-setting process. However, today, some aspects of it — like the rebates private insurers receive from manufacturers — are hidden from view.
Another approach: The Institute for Clinical and Economic Review (ICER) recommends prices based on drugs' clinical effectiveness relative to alternative treatments (and the strength of evidence for it), cost-effectiveness, and the extent to which prices are sustainable with health care program budgets. The process is far from formulaic; importantly, it takes account of additional factors like whether treatment outcomes reduce disparities across patient groups or facilitates greater productivity.
ICER's approach isn't perfect, but it is at least is open and includes public input, which is more than can be said for the rebates manufacturers offer insurers and pharmacy benefits managers.
The bottom line: If nothing else, a price for a monopoly drug will not widely be accepted as "fair" if it is arrived at in secret.
Other voices in the conversation:
- Greg Aune, pediatric oncologist, Greehey Children's Cancer Research Institute: Value isn't just about surviving cancer
- David Mitchell, president and founder, Patients for Affordable Drugs: Drugs don't work if people can't afford them
- Usman Azam, president & CEO, Tmunity Therapeutics: How to evaluate breakthrough therapies
- Paul Howard, senior fellow, Manhattan Institute: Price should be based on outcome

Drugs don't work if people can't afford them
From our Expert Voices conversation on drug pricing.
American citizens help fund the basic science behind most drugs, and then we give corporations monopoly power to set the prices at whatever the market will bear. 50-60% of all new drugs are based on research funded by U.S. taxpayers and currently, we pay twice as much for most drugs as people in other wealthy nations.
Drug companies have a responsibility to:
- Acknowledge taxpayers' investment and explain how the price of a drug reflects that investment.
- Publicly commit that when a drug is approved in other countries, U.S. taxpayers will not be charged more than citizens of other wealthy nations given America's unique investment into the science driving drug discoveries.
- Explain how the price of an orphan drug for treating rare diseases will decline as the number of patients receiving the drug expands.
The bottom line: Novartis's new CAR-T drug, Kymriah, is an incredibly important one. But American taxpayers invested over $200 million in CAR-T's discovery. Based on several different data points, we believe the price for Kymriah is about $125,000-150,000 too high. That's disappointing. Drugs don't work if people can't afford them.
Other voices in the conversation:
- Greg Aune, pediatric oncologist, Greehey Children's Cancer Research Institute: Value isn't just about surviving cancer
- Usman Azam, president & CEO, Tmunity Therapeutics: How to evaluate breakthrough therapies
- Austin Frakt, health economist, Department of Veterans Affairs, Boston University and Harvard University: The public should have a say in what a drug is worth
- Paul Howard, senior fellow, Manhattan Institute: Price should be based on outcome

Value isn't just about surviving cancer
From our Expert Voices conversation on drug pricing.
The recent FDA approval of CAR T-cell therapy is a major milestone in the longstanding effort to cure childhood cancer, once almost uniformly fatal.
The problem: Today childhood leukemia is treatable in most cases and 80% of children survive longer than five years. Unfortunately, early exposure to radiation and chemotherapy can have devastating long-term health impacts for childhood cancer survivors. Up to a third of long-term survivors will suffer from at least one life-threatening or debilitating medical problem caused by their "curative" treatment, which can include secondary cancers, severe cardiovascular disease, infertility, and endocrine disorders. Thus, many are trading one difficult disease for a lifetime battling numerous health problems.
Why it matters: Because they selectively target tumor cells and spare normal cells, new therapies like CAR-T presumably will result in less damage to normal tissues and cause fewer long-term health problems. They offer incredible hope to a new generation of childhood cancer patients that they can not only be cured, but can look forward to a productive life without additional health burdens.
The bottom line: While the upfront cost of these new therapies are high, any consideration of value should take into account the health care savings generated by an overall healthier and productive population of childhood cancer survivors.
Other voices in the conversation:
- Greg Aune, pediatric oncologist, Greehey Children's Cancer Research Institute: Value isn't just about surviving cancer
- David Mitchell, president and founder, Patients for Affordable Drugs: Drugs don't work if people can't afford them
- Usman Azam, president & CEO, Tmunity Therapeutics: How to evaluate breakthrough therapies
- Austin Frakt, health economist, Department of Veterans Affairs, Boston University and Harvard University: The public should have a say in what a drug is worth
- Paul Howard, senior fellow, Manhattan Institute: Price should be based on outcome

How to evaluate breakthrough therapies
From our Expert Voices conversation on drug pricing.
The value of breakthrough therapies, such as Kymriah, the first approved Chimeric Antigen Receptor Therapy (CAR-T) should be evaluated with the following filters:
- Are these therapies providing incremental and meaningful benefit versus the available 'standard of care' and with a risk profile that is manageable for most of the patient population it will be used in? The evidence overwhelmingly indicates this is the case for Kymriah being used to treat children with leukemia.
- What is the current cost of alternative therapies for these patients, if they exist? For children with leukemia, their only other hope of a 'curative' treatment is a bone marrow transplant. The average cost of that and associated care is between $800,000 and $1 million, and reported success rates are lower than the new offering of CAR-T, which is only administered once to the patient in a 'transplant light' environment.
- What does it cost to make these therapies and deliver them to a patient? For most manufacturers of these therapies the initial 'cost of goods' will be high, much more than traditional medicines. As manufacturing science of these therapies improves, these costs will go down.
The bottom line: New therapies may cost comparatively less than existing ones — and deliver more.
Other voices in the conversation:
- Greg Aune, pediatric oncologist, Greehey Children's Cancer Research Institute: Value isn't just about surviving cancer
- David Mitchell, president and founder, Patients for Affordable Drugs: Drugs don't work if people can't afford them
- Austin Frakt, health economist, Department of Veterans Affairs, Boston University and Harvard University: The public should have a say in what a drug is worth
- Paul Howard, senior fellow, Manhattan Institute: Price should be based on outcome

Price should be based on outcome
From our Expert Voices conversation on drug pricing.
Innovative drugs like Kymirah deserve innovative reimbursement contracts – paying for value, not by the pill. Novartis is embracing that adage, and offering to waive the drug's $475,000 fee for patients who don't respond.
That's great, but we're not just paying for medicines. Bundled payments for all oncology-associated care (including hospital, ER costs, and physician visits) linked to patient outcomes can encourage providers and drug companies to collaborate — and compete— on delivering the best outcome for each patient as efficiently as possible.
Kymirah can make a great test case for this approach. Treatment centers that specialize in gene and cellular therapies can work with Novartis and other companies to build detailed patient registries that help oncologists use "real-world data" on what really happens to patients — and why — to improve outcomes while reducing unnecessary costs and avoidable side effects. We already take a similar approach with patient registries and bundled payments for organ transplants.
The bottom line: An outcomes-based payment system can help us put more patients' cancers into remission for longer periods of time – with fewer wasted treatments, and less need for follow on therapies. That's greater value for every dollar we spend on cancer care.
Other voices in the conversation:
- Greg Aune, pediatric oncologist, Greehey Children's Cancer Research Institute: Value isn't just about surviving cancer
- David Mitchell, president and founder, Patients for Affordable Drugs: Drugs don't work if people can't afford them
- Usman Azam, president & CEO, Tmunity Therapeutics: How to evaluate breakthrough therapies
- Austin Frakt, health economist, Department of Veterans Affairs, Boston University and Harvard University: The public should have a say in what a drug is worth