North Carolina's plan to cut weight-loss drug coverage for state employees has side effects
Add Axios as your preferred source to
see more of our stories on Google.
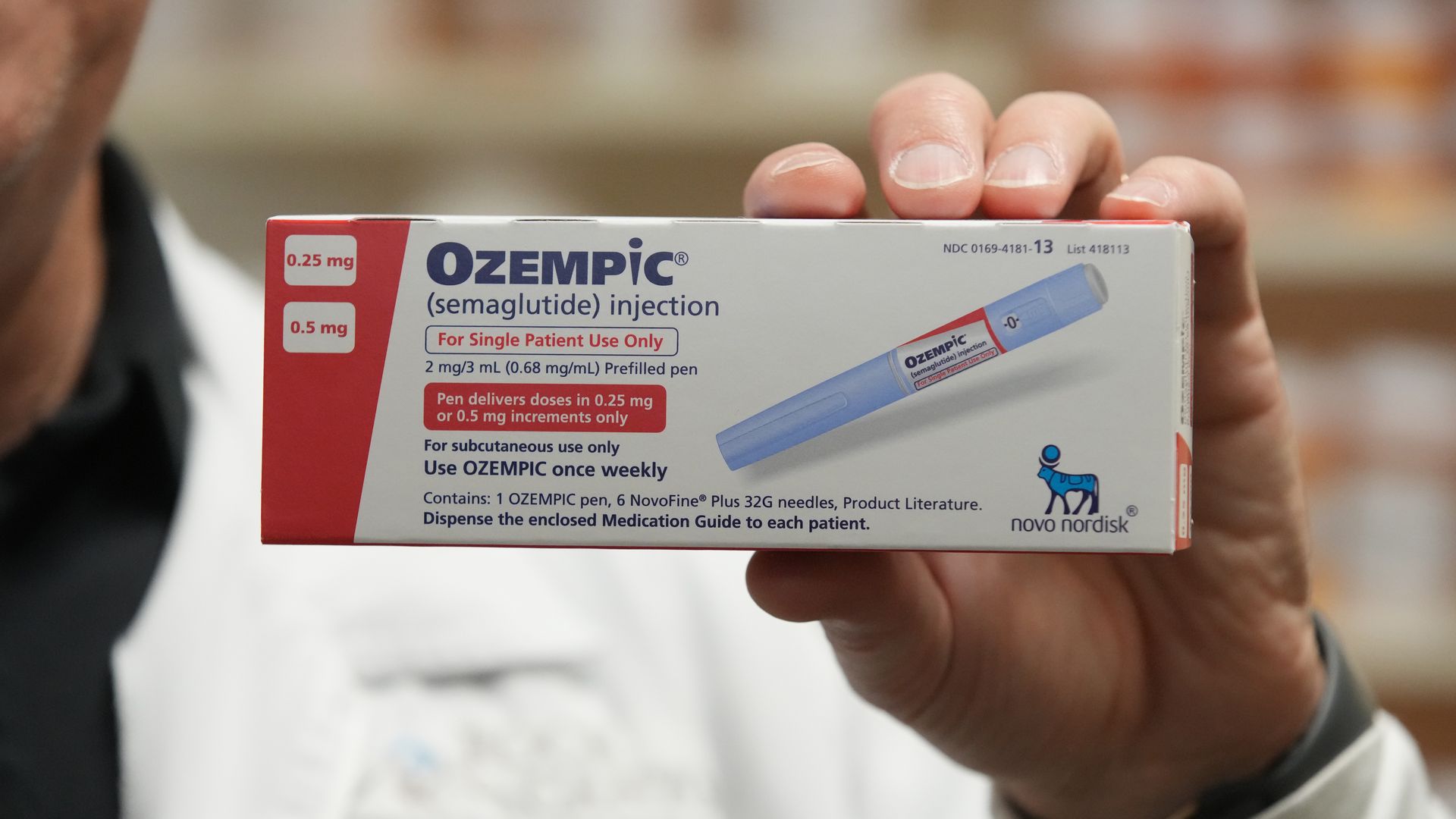
Prescriptions of appetite suppressing GLP-1 weight-loss drugs skyrocketed 300% from 2020 to 2022. Photo: George Frey/Bloomberg via Getty Images
North Carolina's decision to no longer cover weight-loss drugs like Ozempic and Wegovy for state employees is facing public pushback from national groups.
Why it matters: The explosive growth of Ozempic and other drugs known as GLP-1 agonists has led to greater recognition of obesity as a chronic condition rather than a lifestyle disease.
- But it's also sparked major concerns about the potential budget-busting costs of treating the more than 40% of Americans who are obese.
Zoom in: In January, North Carolina became one of the first states — and one of the most prominent employers — to say it would no longer cover the popular, but expensive, weight-loss drugs for its 750,000 state employees.
- "Our state health plan is under siege because of the cost of this one type of drug," outgoing State Treasurer Dale Folwell told Axios. "If we had stayed the course, there was a potential doubling of the premium on state employees."
State of play: Several groups have now come forward to pressure employers and organizations to offer more comprehensive coverage of obesity care.
What they're saying: Sima Sistani, the Durham-based CEO of WeightWatchers (which now prescribes weight-loss drugs), wrote a letter urging the state to change its policy and accusing it of bias against people living with obesity.
- "As a nation, we must stop evaluating coverage of obesity care through a cost-only lens," Sistani wrote in the letter. "The goal of healthcare is not to save money but to improve the health and well being of people."
Zeke Emanuel, a medical ethicist and former Obama health policy adviser, co-wrote a Wall Street Journal opinion piece last week condemning North Carolina's decision to stop covering GLP-1s as weight loss treatments, saying it was unethical.
- "What was said for North Carolina was 'There's a whole swath of people, we're not covering it for them because they're obese.' That is unethical," Emanuel told Axios.
Several health care organizations also came together last month to launch the EveryBODY campaign, which is pushing companies and organizations to include obesity care in their health plans, citing "misunderstandings" about obesity that it says led to insurance restrictions.
- "Obesity should be treated like any other serious chronic disease," said Tracy Zvenyach, policy director at the Obesity Action Coalition.
The bottom line: With more weight-loss related drugs expected to hit the market, and the likelihood that they'll be approved for other conditions like cardiovascular disease, pressure will keep growing on employers to cover GLP-1s and other obesity care.

