Texas kids losing Medicaid insurance in overwhelmed system
Add Axios as your preferred source to
see more of our stories on Google.
More than a million Texans, most of whom are children, lost Medicaid health insurance in recent months as paperwork fell through the cracks.
- Overwhelmed technology, outdated information and a lack of resources for state employees are creating major gaps in the public health system for people with low incomes.
Why it matters: Lapsed coverage for even a month means children miss out on emergency medical care — or get big bills for it — as school sports are underway and flu season kicks in, Graciela Camarena, program director for health outreach and enrollment at Children's Defense Fund-Texas in the Rio Grande Valley, tells Axios.
- Experts have cautioned that the mass loss of Medicaid coverage could erode trust in the health care system and disproportionately affect children and people of color, Axios' Maya Goldman reports.
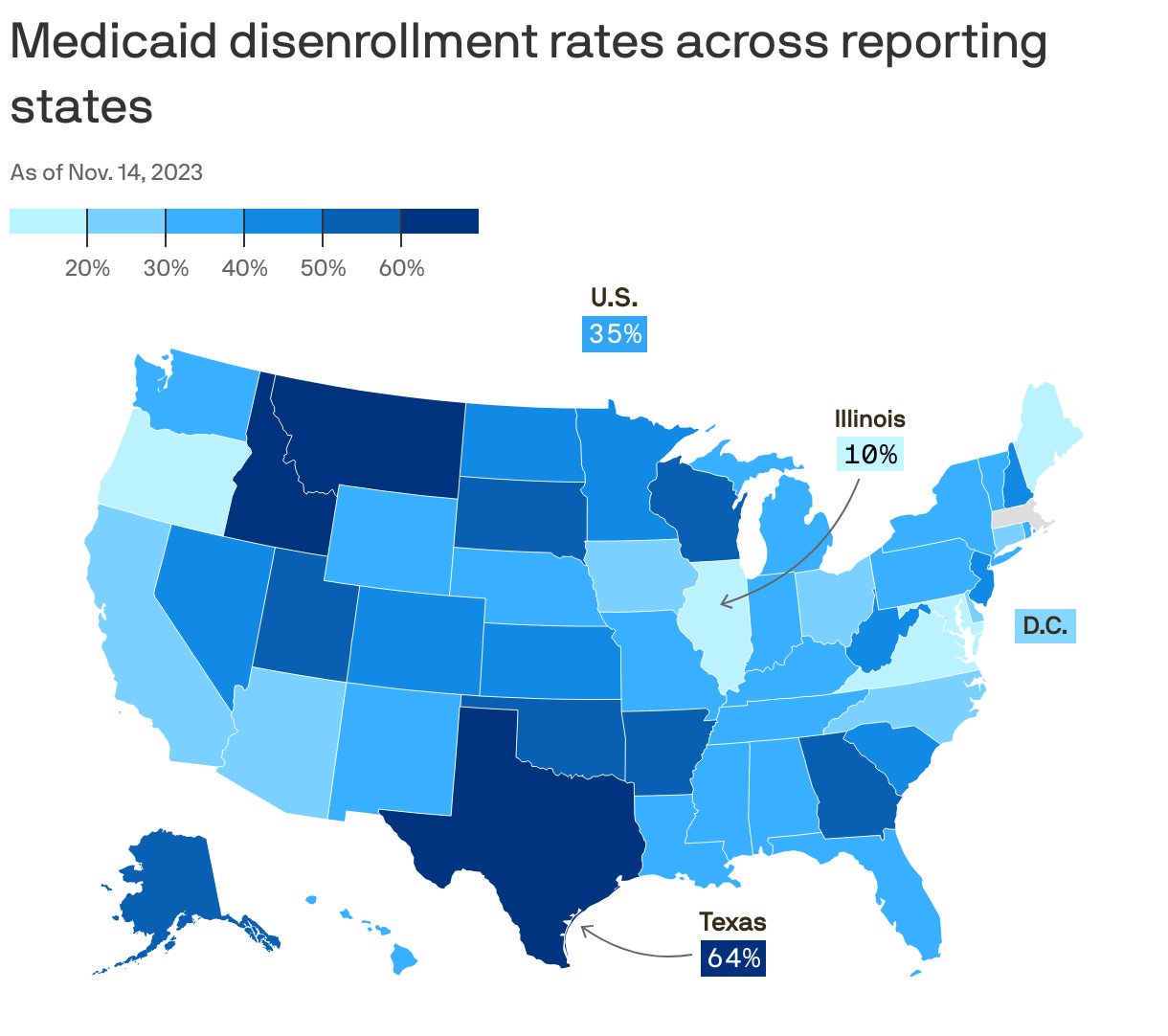
The big picture: Texas is the epicenter of a national problem in which states have struggled to recheck the eligibility of Medicaid recipients who were allowed to keep their coverage during the pandemic regardless of changes in income.
- Nationally, about 1 in 4 Medicaid enrollees said this spring they didn't know where to find insurance if they lost Medicaid coverage, and 15% said they would be uninsured, per a KFF survey.
The other side: State officials spent more than a year preparing to recheck Medicaid eligibility for about 6 million people, Texas Health and Human Services Commission spokesperson Tiffany Young tells Axios.
- "We have open lines of communication with our staff," Young said in an email. "This is a massive undertaking, and when eligibility issues are discovered through our quality assurance process, we work to systematically resolve them to minimize impact to our clients."
How it works: Texans must renew their Medicaid coverage every year. But during the pandemic, a federal law allowed people to remain on Medicaid so they wouldn't lose insurance during the public health emergency.
- That continuous Medicaid coverage ended on March 31 this year. Texas and other states began re-checking eligibility in April.
- But nationwide, 71% of people who lost coverage were removed for procedural reasons, as states struggled to keep up with a high volume of paperwork, per the most recent available data tracked by KFF.
By the numbers: About 1.4 million Texans have lost Medicaid coverage since the state began rechecking eligibility, per KFF.
- About 65% of Texans undergoing the redetermination process have been removed from Medicaid, the highest disenrollment rate in the nation, per KFF.
- Of those who lost coverage, about 68% were removed for clerical reasons like unreturned paperwork — not because they were ineligible.
Yes, but: Nationwide, about 40% of people who lost Medicaid coverage eventually re-enrolled within the year, per KFF.
Context: In Texas, 58% of those losing Medicaid are children. That's in part because Texas is one of 10 states to not expand Medicaid under the Affordable Care Act to cover more low-income adults, advocates tell Axios.
- Texas Medicaid mostly covers children, pregnant people, people with disabilities and older adults.
- To qualify, a four-person household must have income below $59,400. A single person must have income below $28,869.
- Texas has a higher percentage of uninsured residents than any other state, per the U.S. Census Bureau.
What they're saying: "Families usually qualify for Medicaid because of their low income," Camarena tells Axios. "They cannot afford these high medical bills that set them back from getting food on the table."
- An unexpected bill could run anywhere from hundreds to thousands of dollars, depending on the services, Camarena says.
- "Unquestionably we're kicking eligible kids off the program," Stacey Pogue, a senior policy analyst at Every Texan, a policy nonprofit that has advocated for a pause in the Medicaid re-checks, tells Axios.
Details: Pogue identified two main issues leading to high procedural removals in Texas.
- One is that the state does not often use available data from other departments to verify families' income, Pogue says. Texas uses such data in 1% of renewals, but many other states use it 25% of the time, per the nonprofit Texans Care for Children.
- That means employees must manually reach out to recipients for more information, often through mail. But the agency doesn't always have updated addresses for Medicaid recipients.
- The second is that state employees are overwhelmed by a high volume of work and what they say is a lack of resources, leading to a delay in sending action-required notices.
State of play: Texas Health and Human Services employees have anonymously written multiple whistleblower letters since July detailing concerns about the state's Medicaid renewal process and people losing coverage in error.
- That led Texas' Democratic congressional delegation to ask the Biden administration to intervene.
- "These disruptions and coverage gaps risk patients' health and financial stability," the Democrats wrote in a letter.
Of note: Gov. Greg Abbott has not commented on the state's Medicaid redeterminations. A spokesperson declined a request from Axios for an interview or for comment.
Recipients affected by delayed action-required notices were given extra time to return information before the state removed anyone, Young, with Health and Human Services, says.
- The agency has made changes to recruit and retain staff — including up to a 25% salary increase for frontline eligibility advisers, per Young.
- The eligibility adviser vacancy rate stood at 21.2% in March 2022.
- It was 4.4% in April when Texas restarted Medicaid renewals, and 3.7% as of Nov. 2, Young says.
The bottom line: Technology and staffing both need upgrades to improve the situation, Pogue says. Even then, it will take time for the fixes to make a difference.
