States rethink Medicaid enrollment efforts as millions lose coverage
Add Axios as your preferred source to
see more of our stories on Google.
The largest-ever purge of the nation's Medicaid rolls has exposed major cracks in the system for covering the poorest Americans — and is prompting some states to rethink how they connect vulnerable residents to benefits they're entitled to receive.
Why it matters: Millions have been booted from the safety-net program seven months after the expiration of pandemic-era protections, most often due to bureaucratic reasons and not necessarily because they no longer qualify.
- The so-called "unwinding" process, in which states are redetermining Medicaid eligibility for the first time in three years, has highlighted the administrative and technical barriers that typically prevent many who are eligible from signing up or remaining enrolled.
- "It would be a failure if we come out of this with the same old standards and processes we had in place prior to the public health emergency," New York Medicaid director Amir Bassiri told a national board of Medicaid advisers earlier this month.
Catch up quick: States regularly review if people enrolled in Medicaid still qualify based on income or other eligibility factors. But those checks were put on hold during the pandemic, and enrollment in Medicaid and its sister program, the Children's Health Insurance Program, swelled nearly 30% during the pandemic to more than 92 million people at the end of 2022.
- Aside from the difficulty of reengaging tens of millions of people whose coverage had been safe for three years, states' outdated eligibility and technology systems and workforce shortages are adding to the challenge of redetermining who's eligible, said Matt Salo, the former executive director of the National Association of Medicaid Directors.
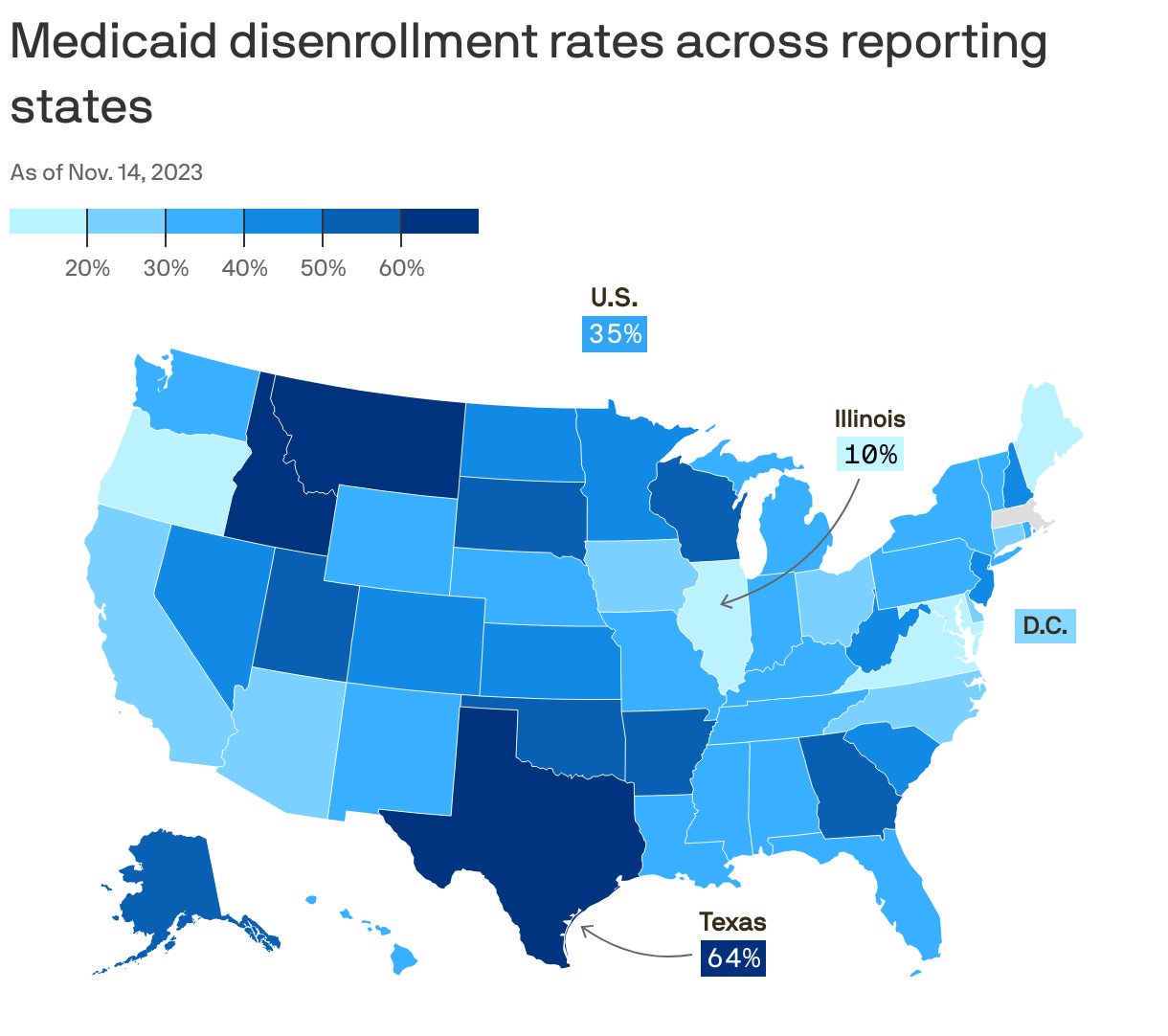
State of play: More than 10 million people nationwide have lost Medicaid coverage since April, including about 7 in 10 who lost their insurance for procedural reasons, according to KFF.
- These reasons vary. Some enrollees never received renewal notices because states don't have their current address. It may not be clear what documents they have to mail in or upload online to remain covered.
- The renewal process can look quite different from state to state, since they have flexibility to administer their programs, which they jointly run with the federal government.
- In New Mexico, 96% of people removed from Medicaid this year have lost coverage for procedural reasons, but that figure is just 7% in Oregon, per KFF's data.
- Even within a state, the process can differ. In New York, 58 local districts each process eligibility determinations for a portion of Medicaid enrollees, said Bassiri, the state's Medicaid director.
- "Each has different capability and sophistication," he said.
States got a three-month heads-up from the federal government before they could resume coverage renewals. Some took a few more months before starting.
- As of August, nearly one-third of states had been warned by the federal government that their Medicaid call center wait times were too long, the Associated Press reported.
- A half-million people, mostly children, were improperly knocked off Medicaid because states were using a faulty method for redetermining their eligibility. States have been restoring that coverage, but they said federal Medicaid officials failed to raise the issue during preparations for the unwinding period.
- States have up to 14 months to redetermine coverage for all Medicaid enrollees, but some have already finished.
- "Any person being improperly disenrolled from health care coverage is unacceptable to this administration," said a Department of Health and Human Services spokesperson. "Many states have stepped up," but HHS "will not be afraid to take enforcement action" if states don't heed the department's call to do more to protect coverage, the spokesperson added.
Zoom out: It's unclear how many people who have lost Medicaid coverage found insurance through an employer or elsewhere. Some, but not many, have signed up for coverage through the Affordable Care Act's subsidized insurance marketplaces.
- An expected increase in the uninsured rate is starting to impact the health care system. Hospitals' uncompensated care as a percentage of operating revenue rose from 6.4% in March to 8.7% in July, according to data compiled by Syntellis Performance Solutions and published by the American Hospital Association.
- The proportion of emergency department visits among people with Medicaid coverage decreased 2.8 percentage points during a similar period, while visits among those not using insurance increased 2.4 percentage points, according to Epic Research.
- "When folks lose their eligibility for Medicaid or the total uninsured [rate] goes up, obviously we feel it. We feel it big-time," said Steve Purves, CEO of Valleywise Health, Arizona's largest public health care system.
Between the lines: The sheer scale of how many people are losing Medicaid coverage due to bureaucratic hurdles may spur long-term improvements to Medicaid eligibility and enrollment systems, experts predicted.
- The unwinding process has brought focus to the "actual nuances, the nuts and bolts, of the eligibility and renewal processes," said Jack Rollins, director of federal policy at the National Association of Medicaid Directors.
- "I do see states really taking a step back and saying, you know, we've got to think differently about how our systems work and how to make them work better for consumers," said Patricia Boozang, senior managing director at Manatt Health.
Zoom in: Governments and organizations that work with Medicaid populations are learning effective ways to keep eligible people enrolled.
- Valleywise Health set up a text messaging program to notify patients when their Medicaid coverage is coming up for renewal.
- About 70% of the center's Medicaid patients so far have kept their coverage, said Valleywise vice president Amanda de los Reyes. Valleywise plans to continue the texting program after the current cycle of redeterminations ends, she said.
- Federal Medicaid officials, meanwhile, have granted states temporary flexibility to make redeterminations easier, like renewing coverage based on an enrollee's SNAP eligibility.
- "We'd love to see those made permanent," Indiana Medicaid director Cora Steinmetz said during the panel discussion with Medicaid advisers this month.
- The Centers for Medicare and Medicaid Services is looking for ways to maintain these flexibilities, a spokesperson told Axios.
- Starting in January, states will be required to keep children continuously enrolled in Medicaid for 12 months before redetermining their eligibility, regardless of any changes in household income.
Reality check: When it comes to addressing issues like Medicaid workforce shortages and updating technology, "unfortunately, sometimes the answers for things like that are you've got to throw a lot more money at it," Salo said.
- States are already bracing for a big jump in Medicaid spending next year as COVID-era support winds down.
