Medicare and Medicaid would cover Ozempic, Wegovy under new Biden rule
Add Axios as your preferred source to
see more of our stories on Google.
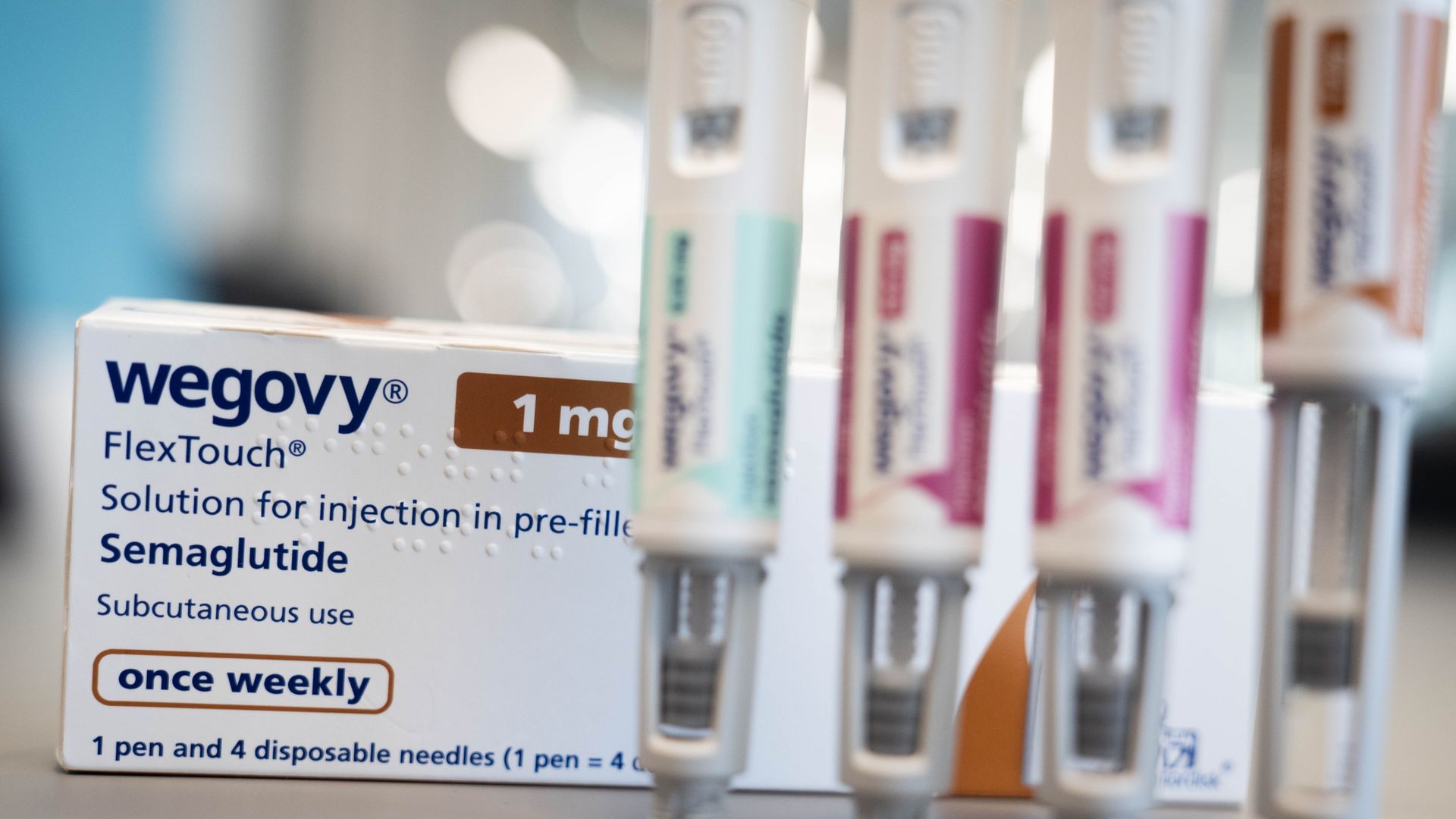
Semaglutide (GLP-1) weight-loss drug Wegovy, made by pharmaceutical company Novo Nordisk. Photo: James Manning/PA Images via Getty Images
The Biden administration on Tuesday proposed requiring Medicare and Medicaid to cover anti-obesity drugs.
Why it matters: The rule would expand access to medications known as GLP-1 agonists for millions of Americans struggling with obesity, who are at higher risk of diabetes, stroke and cardiovascular disease, according to a White House fact sheet.
- The proposal could set up a conflict between pharmaceutical companies and Robert F. Kennedy Jr., President-elect Trump's nominee for secretary of the Health and Human Services Department, who is an Ozempic critic.
Driving the news: Under current law, Medicare is barred from covering drugs for weight loss. That also makes it optional for state Medicaid plans, officials said.
- The new rule proposes a "reinterpretation" of the law, expanding access to the drugs like Novo Nordisk's Ozempic or Wegovy for 3.4 million Americans on Medicare and another 4 million on Medicaid who are obese, per the fact sheet.
- "The medical consensus has evolved. The medical community today agrees that obesity is a chronic disease, it is a serious condition that increases the risk of premature death and can lead to other serious health issues such as heart disease, stroke and diabetes," said Chiquita Brooks-LaSure, administrator for the Centers for Medicare and Medicaid Services, in a call with reporters.
- The proposal could cost taxpayers roughly $40 billion over the next decade, officials said.
State of play: About 40% of American adults are considered obese and therefore at risk of further health complications, according to the Centers for Disease Control and Prevention.
- 22% of people with Medicare had a diagnosis of obesity in 2022, which is more than double the number from a decade earlier and it's believed many more people suffer from obesity without an official diagnosis, CMS administrator Brooks-LaSure said.
- High price tags and insurance restrictions made the drugs difficult to access for many Americans, especially those on Medicare and Medicaid.
- "Without insurance coverage, these drugs can cost someone as much as $1,000 a month," the fact sheet stated.
The big picture: Demand for the drugs has surged in recent years.
- While the drugs were originally approved to treat diabetes, they were later approved for use in obesity as well as heart disease.
- The popularity of Ozempic among celebrities and TikTokers has also contributed to shortages for patients in need.
Go deeper: United States of Ozempic: Where anti-obesity drugs are taking off
Editor's note: This story was updated with additional details.

