Axios Vitals

June 16, 2017
Good morning ... Congress doesn't seem to be too bothered that it's not going to make any Affordable Care Act fixes before insurers' filing deadlines. We try not to get too stressed about deadlines either, but we do enjoy having jobs.
Deadlines, schmeadlines
Insurers must decide by Wednesday whether they're going to participate in 39 states' insurance exchanges next year. And, despite some Republicans' desire to help quell the turmoil already roiling those markets, Congress has run out of time to provide any help.
"Like anything else, there's going to be deadlines and there's going to be real deadlines," said Sen. John Thune, a member of GOP leadership. "We assume, of course, insurance companies are going to work with us and there's going to be some flexibility on their part. But we also know that we gotta move as quickly as we can."Why it's a problem: As Caitlin Owens points out, even if Congress includes some sort of stabilization measures in their health care bill, those steps won't do much for the 47 counties where no one is selling insurance next year — and carriers won't be able to enter those markets after next week's deadline, no matter what Congress comes up with.For your finger-pointing pleasure: A new analysis by Oliver Wyman concludes that two thirds of the rate increases in 2018 will be caused by the uncertainty over whether insurers will get paid for their cost-sharing reduction subsidies and whether the Trump administration will enforce the individual mandate.
Everybody is unhappy on health care
- House Republicans aren't happy about President Trump calling their bill "mean" after he leaned on them so hard to pass it. "For him to turn around and do this, it's stunning. I can't believe it," one lawmaker told our colleague Jonathan Swan.
- Sen. Lisa Murkowski isn't happy about the process. "I can't show to my constituents back home anything concrete because we don't have anything," she said in an interview with Vox.
- Murkowski isn't the only one grumbling about all the secrecy, as the New York Times reports.
- Conservatives are unhappy on the merits, fearing the bill will pull too hard to the center, per the Wall Street Journal.
The “essential benefits” insurers would most likely drop
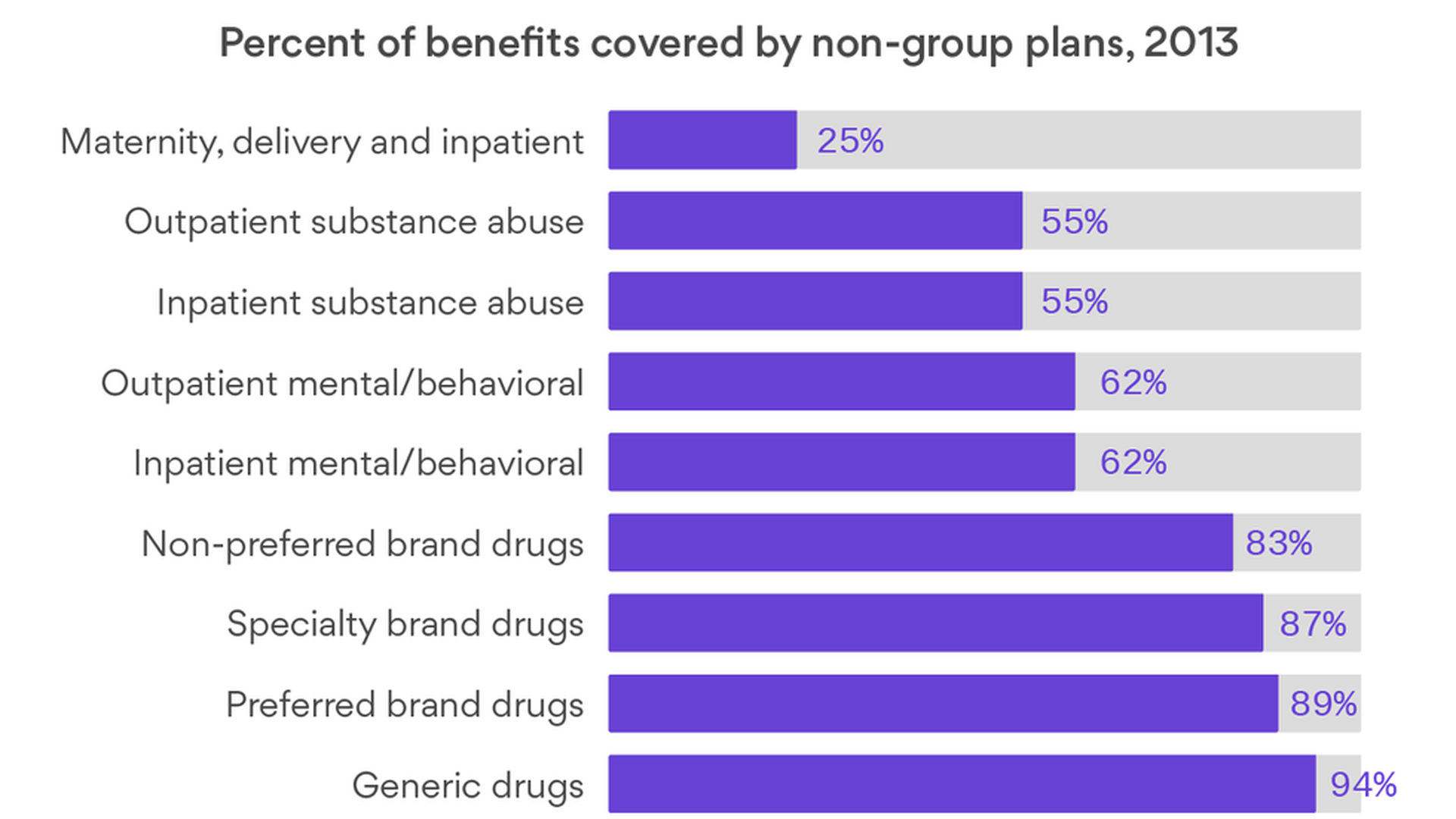
The Senate's health care bill will probably allow states to waive the ACA's "essential benefit" mandates. But would insurers really quit covering those services if they're allowed to? A new Kaiser Family Foundation brief suggests that they would — and that maternity care might be the first to go. (You might hear Democrats mention this once or twice over the next few weeks.)
Kaiser looked at more than 8,000 plans, from all 50 states, that were on the market before the ACA's benefit mandates took effect, to see how widely they were already covering each of the law's essential benefits. Check out the graphic and you can see the results — only 25% of plans were covering maternity benefits.
New FDA chief wants faster approval for digital health tech
FDA commissioner Scott Gottlieb is pretty excited about new medical apps and other digital health tech, so he's launching a new initiative to try to get them to market faster. In a blog post yesterday, he announced the centerpiece of the new Digital Health Innovation Plan: He wants to let third parties certify new products that aren't considered high risk.
How it would work: The third parties would look at whether a company "consistently and reliably engages in high quality software design and testing." For higher-risk products, Gottlieb would still have the FDA do its usual premarket review, but that process would be streamlined.
Why it matters: Everyone wants cool new medical apps, but — as with everything else with the FDA — the challenge is how to speed up the reviews without sacrificing safety. It's worth keeping an eye on it, but Gottlieb was adamant during his confirmation hearings that he'd never trade off safety for speed.
Trump might promote value-based drug pricing...
Trump administration officials are having a meeting today to bat around some ideas for executive actions they can take on drug prices. And one idea has emerged that will make health care nerds very happy, per Bloomberg: The White House might promote value-based pricing, in which insurers pay for drugs based on how well they work on specific diseases and patients.Why it matters: That's actually an idea that wouldn't get a big fight from the pharmaceutical industry. The Pharmaceutical Research and Manufacturers of America has been pushing for legislative and regulatory changes to make it easier to promote those kinds of arrangements. But without legislative changes, the Trump administration may have to settle for using them only in federal programs, like Medicare Part D.Our thought bubble: Our thoughts are with the speechwriter who gets to tell Trump how to explain value-based pricing. We have enough trouble explaining it ourselves.
...but value-based pricing might not work
Research published yesterday in the New England Journal of Medicine throws some cold water on the promise of value-based purchasing, at least in hospitals. Hospitals that are part of the program — which conditions some of their Medicare payments on a complex set of performance metrics — don't seem to perform any better than hospitals that aren't, according to the NEJM article.
The bottom line: Both groups of hospitals have improved since value-based purchasing took effect, but at about the same rate.
Yes, but: The NEJM authors noted that another, somewhat similar ACA policy — penalties for hospitals that readmit a lot of patients — seem to be working pretty well. That program might be more effective because it's simpler, the authors said, and because it uses penalties instead of bonuses.
Apple’s play for Athenahealth?
Christina Farr at CNBC reported this week that Apple is looking into ways to turn iPhones into medical record repositories. That jolted the imagination of Citi analysts, who put out a report (h/t CNBC's Meg Tirrell) suggesting Apple could acquire cloud-based electronic health record company Athenahealth — which is under pressure from an activist investor to either improve profits or sell.
Our thought bubble: It's not inconceivable. An Athenahealth price tag could be more than $6 billion, based on industry estimates. Apple would have no problem paying that, and it would give Apple a cloud-based platform that many doctors already use. But there are a lot of hurdles in the way, including doubts about whether CEO Jonathan Bush would concede selling his company.
What we're watching next week: Biotechnology Innovation Organization annual convention in San Diego, June 19-22. Mylan annual shareholder meeting, June 22.
Place your bets: When do you think the Senate will vote on health care? Send us your predictions, comments, complaints, tips, etc.: [email protected] and [email protected].
Sign up for Axios Vitals

Healthcare policy and business analysis from Tina Reed, Maya Goldman, and Caitlin Owens.