Axios Future of Health Care

January 03, 2025
Good morning, and Happy New Year! I hope your holiday season was restful and full of good times.
Today's word count is 895, or a 3.5-minute read.
1 big thing: 2025's obesity battle
For all the changes in recent years in how obesity is understood and treated, 2025 is shaping up to feature familiar battles over whether the condition is a disease or the product of lifestyle choices.
Why it matters: Obesity is a major public health threat in the U.S., and while new drugs have finally given doctors and patients a tool to meaningfully treat the disease, rejection of those drugs in favor of lifestyle changes at a policy or cultural level could blunt important public health progress.
- But high-profile skeptics of the drugs have a point: They don't address the underlying causes of the country's obesity epidemic.
Where it stands: 2024 ended with a clash between Robert F. Kennedy Jr., President-elect Trump's nominee for HHS secretary, and Elon Musk over GLP-1s for weight loss.
- "The first line of response should be lifestyle. It should be eating well, making sure you that you don't get obese, and that those GLP drugs have a place," Kennedy told CNBC last month.
- "Nothing would do more to improve the health, lifespan and quality of life for Americans than making GLP inhibitors super low cost to the public. Nothing else is even close," Musk wrote on X around the same time.
The big picture: Kennedy and Musk are emerging as influential voices in the Trump administration, each with the power to shape popular opinion as well as government policy around coverage and potentially even pricing of the drugs.
Between the lines: Lifestyle and new anti-obesity medications both play a role in the obesity narrative, experts say. But they're not substitutes for one another.
- Americans' unhealthy diet and increasingly sedentary lifestyle — a product partially of changes in how we make a living — are likely behind the decades-long rise in obesity rates, and reversing those lifestyle trends could help prevent more people from developing obesity to begin with.
But researchers have found that obesity causes biological changes that make lifestyle adjustments alone a poor treatment plan.
- "Once you have the disease of obesity and you go on a diet and you exercise and you lose weight, your body's hormones think you're starving to death," said Caroline Apovian, co-director of the Center for Weight Management and Wellness at Brigham and Women's Hospital.
- The body is "going to increase the hunger hormone and decrease the satiety hormones until you gain that weight back," she added.
- Plus, "with no support, people will typically go back to their typical eating habits and exercise habits," said Thomas Wadden, a professor of psychology at the University of Pennsylvania. "Hard work alone is not going to make people successful in the context of the current food and activity environment."
And lifestyle changes on the scale that would be necessary to make long-term dents in obesity rates are unrealistic, experts say.
- "Whatever is in the environment that has caused this disease is not going away," Apovian said. "We're not going to get rid of ultra-processed food. The cat's out of the bag. So RFK — you're right, yeah, but we're never going to get there."
Details: GLP-1s work by reducing a person's hunger levels and combating the biological changes made by obesity.
- Obesity rates stopped climbing this year, likely related to Ozempic use.
- But the drugs' high price tag and frequent lack of insurance coverage puts them out of reach for millions of Americans who could benefit. Plus, patients have to keep taking the drugs for them to remain effective, and they can have unpleasant side effects.
The bottom line: "Treating patients with drugs is the simplest way to deal with the problem at this point, but it really is sort of a moral hazard, because it doesn't require us to change the environment that keeps creating more obese people," Wadden said.
2. By the numbers: GLP-1 use surges
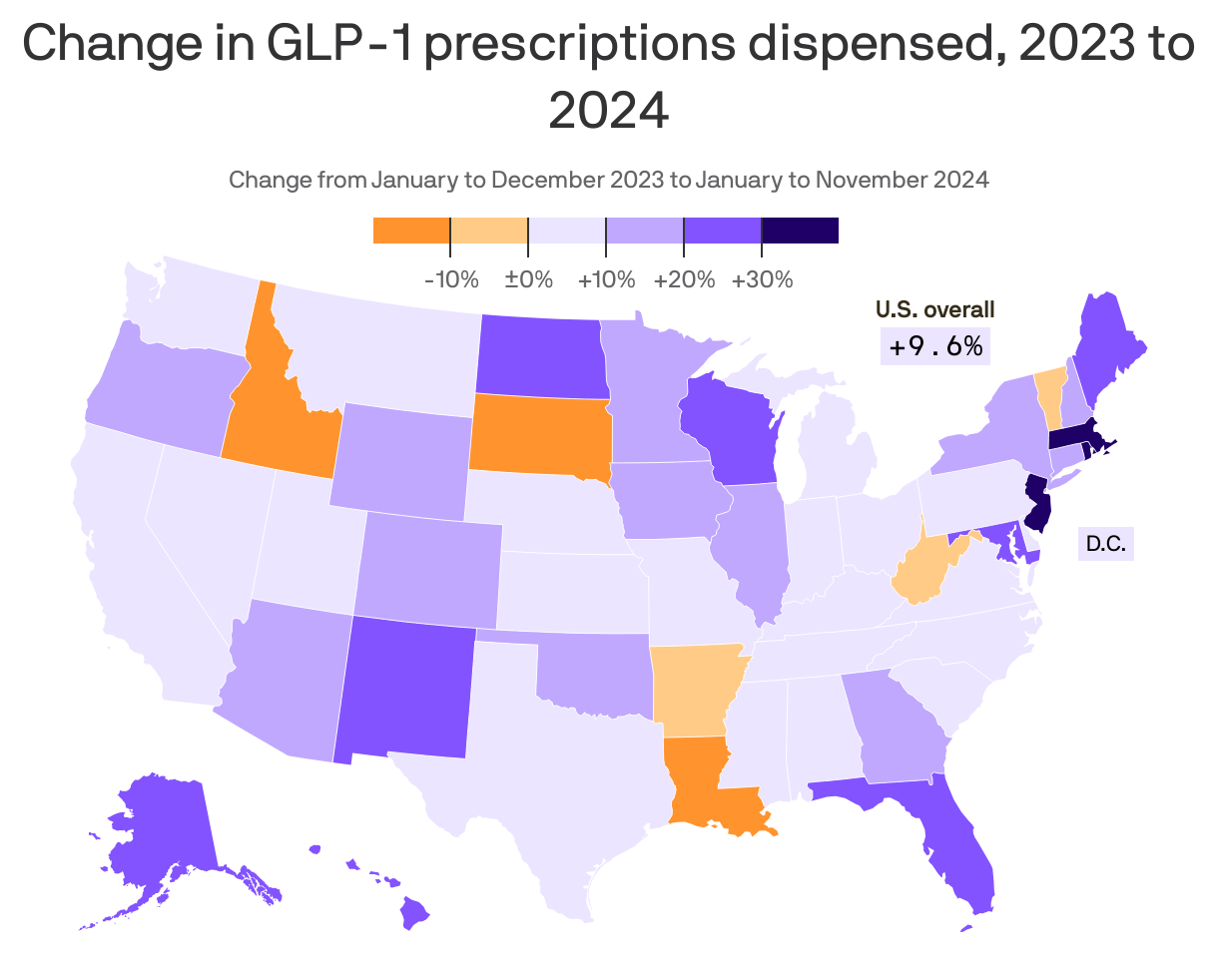
The number of prescriptions for GLP-1 drugs — which are also used to treat diabetes — jumped roughly 10% in 2024, according to insurance claims data provided to Axios by health analytics company PurpleLab.
Why it matters: The data, which shows double-digit growth in 23 states, offers a snapshot of the sustained growth in demand across the U.S. for the drugs hailed as game-changers in the fight against obesity, Axios' Tina Reed reports.
Between the lines: The most prescriptions dispensed went to adults ages 55 to 65 (29%), followed by seniors 65 and older (26%).
- The vast majority of prescriptions went to commercially insured patients.
The data is based on a collection of roughly 7.5 billion claims from private insurers, as well as Medicare — which only covers GLP-1s to treat diabetes — and Medicaid.
- The data lumps the prescriptions together, so it's not possible to tease out how often these drugs are being prescribed for obesity versus diabetes or heart disease.
3. What I'm reading
Here are a few of the things that earned my click after more than a week offline!
🍟 Kidney stones are becoming more common among children, and some experts blame ultra-processed foods, the Washington Post reports.
🧪 Stat compiled a list of the 10 biggest medical advances of 2024.
🤝 The WSJ created a fun data graphic exploring the deals that helped UnitedHealth Group become so enormous over time.
💉 Bookmark this, because it's probably going to come up a lot: Vaccines don't cause autism, but scientists say there is no singular thing driving the rise in cases, the New York Times reports.
Thanks to Nicholas Johnston and Adriel Bettelheim for editing and Matt Piper for copy editing.
Sign up for Axios Future of Health Care


