There are 500K cholera cases in Yemen— and a global stockpile of at least a million vaccines
Add Axios as your preferred source to
see more of our stories on Google.
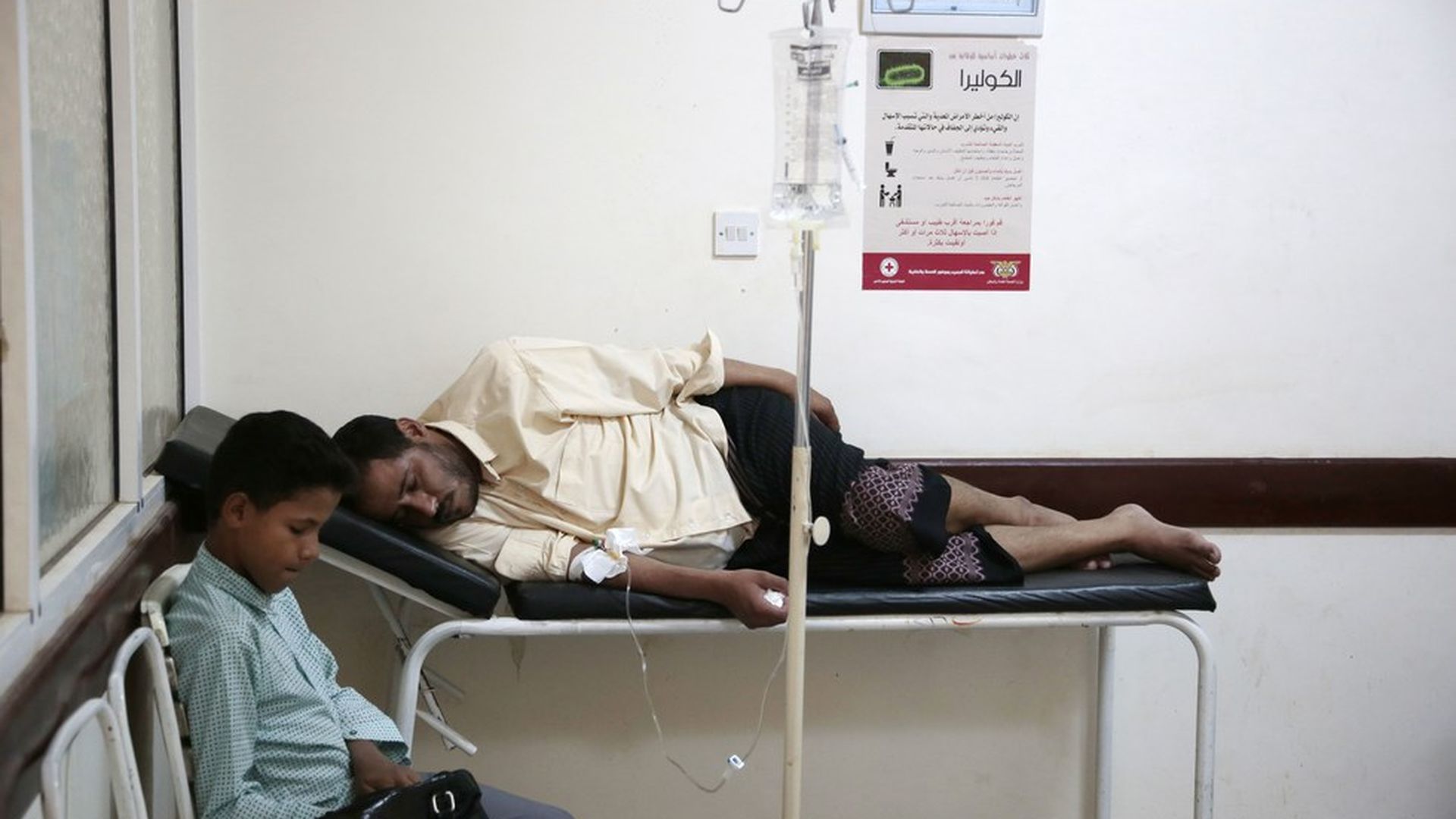
Associated Press
Earlier this week the WHO reported there have now been more than 500,000 cases of cholera in Yemen since April — making it one of the world's largest and fastest growing epidemics of the diarrheal disease to date.
Yes, but: In July, the organization made a surprising announcement that it wasn't moving forward with plans to begin administering half a million doses of cholera vaccine that were standing by for delivery, saying it would be ineffective given the security situation in the country and the epidemic's rapid escalation. Instead they intend to focus on improving sanitation and access to clean water and treatment.
Expert opinion: I spoke with cholera experts who have been involved in vaccination campaigns around the world. All noted they haven't worked in Yemen but from a global perspective are concerned the current plan in the country doesn't reflect what's known about the vaccine's effectiveness, and could perpetuate a belief that vaccinating people in the midst of an epidemic won't have an impact.
Two beliefs:
Once an epidemic is underway, vaccinating won't have an impact.
- "It's misguided," says David Sack of Johns Hopkins who chairs a task force on oral cholera vaccine (which WHO participates in). "The fact that it wasn't given earlier isn't a reason to give it whenever you get it."
- Andrew Azman, also from Hopkins but based in Malawi, points to the success of using the Shachol vaccine in the midst of a 2012 outbreak in Guinea to stop transmission.
- Modeling by Azman and his colleagues found evidence that single doses of vaccine can afford some short-term protection against infection.
- "Obviously you have the biggest impact if you vaccinate before an epidemic or at the earliest stages but you can still avert plenty of cases and plenty of deaths well after the peak of an epidemic."
It is only effective to vaccinate people who haven't been infected with the disease.
- Louise Ivers, who has led Partners In Health's cholera vaccine efforts in Haiti, where a seven-year epidemic of cholera rages on, says there is no harm in vaccinating people who are already exposed to cholera or have natural immunity to it.
- Its less efficient to vaccinate large numbers of people who have already been infected, but vaccinating some in the interest of protecting all those that are still at risk is worthwhile, Ivers said.
WHO spokesperson Gregory Härtl: "If you can "blanket" vaccine coverage before people are infected, they will not get infected, thus reducing the number of people who can spread the disease, whereas if you try to vaccinate once the cholera outbreak is in full swing, the number of people already infected and able to transmit the disease is already so great that the effectiveness of (scarce) vaccine is greatly diminished."
The vaccine: One of the least expensive and widely used — Shachol— is $1.85 per dose and requires limited health training to be delivered orally. A recent summary of studies found cholera vaccines are 76% effective in the field.
Ivers: "Water and sanitation have been the way we historically deal with cholera. But in Europe, thousands of people died over the decades it took us to build infrastructure... It's very hard to immediately deliver clean water to thousands or millions of people. Vaccine is the bridge. We know it works."
Sack: "I'm sympathetic to the difficulties in providing vaccine but the idea that they are going to improve sanitation when they can't give a simple oral vaccine flies in the face of reality... This is often thought of as a dichotomy — vaccines or sanitation. These are not opposing options. They need to be integrated."
The bottom line: Cholera is a global disease increasingly affecting people, especially those living in poverty and conflict, around the world. "It is 100% preventable and 100% treatable. No one should die of diarrhea," said Ivers.
