Sepsis, the sneaky killer, is the focus of a new push for treatments
Add Axios as your preferred source to
see more of our stories on Google.
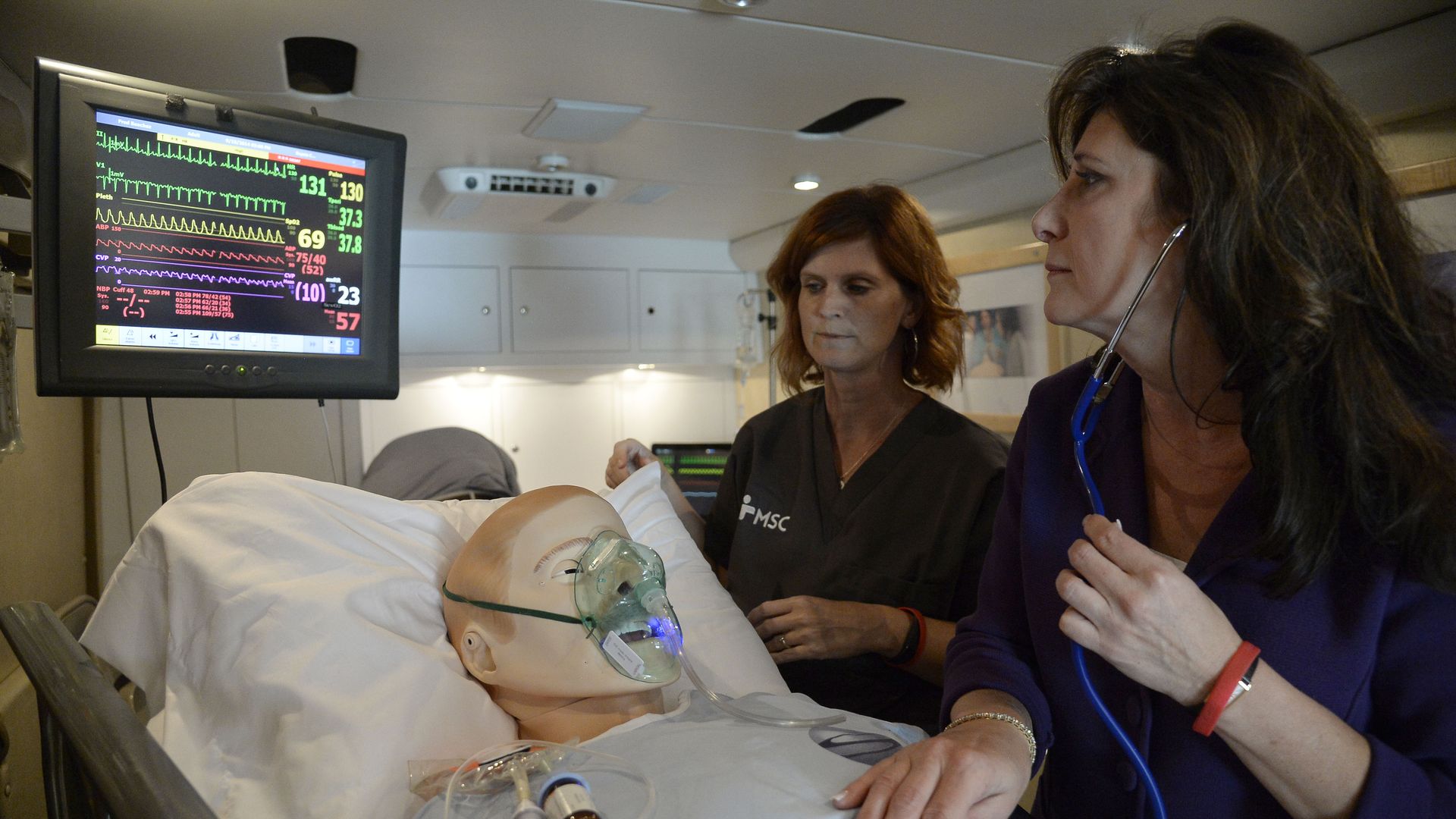
Sepsis survivor Pamela Popp checks out a sepsis medical training demonstration using dummies. Photo: John Leyba, The Denver Post via Getty Images
Combatting sepsis — the body-wide immune response to an infection that can lead to amputations, the loss of organs or death — continues to elude researchers, who are trying to develop a consistent and effective treatment.
Why it matters: Sepsis affects more than 30 million people worldwide every year, killing roughly 6 million. But, it's tricky to treat and quick to develop, leaving doctors with little option but to flood the body with multiple antibiotics and other therapies once the blood infection has developed.
"Sepsis is a medical emergency... and incredibly complicated."— Runa Hatti Gokhale, CDC sepsis expert
What we know: Gokhale says any type of infection can turn into sepsis, but the most frequently identified germs linked to sepsis include Staphylococcus aureus (staph), Escherichia coli (E. coli), and some types of Streptococcus.
- At least 1.7 million Americans develop sepsis every year, of whom 270,000 die — making it a leading cause of death in the U.S.
- CDC is focused on a campaign on the "challenge of preventing sepsis and recognizing it earlier," Gokhale says.
- Treatment protocol tends to start with antibiotics ASAP, followed by other steps.
Between the lines: There's growing concern about the general practice of hitting patients with multiple antibiotics within the first three hours of admittance in an effort to combat the infection, largely due to rising antibiotic resistance.
- Gary Eldridge, president and CEO of the pharmaceutical company Sequoia Sciences, says antibiotic resistance and the problem of sepsis is "vastly worse than anyone thinks," because the data is published every 3–4 years while antibiotic resistance continues to grow.
Urinary tract infections (UTIs) are 1 of the 4 main types of infections linked with sepsis, along with lung, skin and gut infections, Gokhale says.
- Recurrent UTIs are of particular concern because often a patient is given automatic refills and "there's no database to go to that says how many refills a person has gotten," says Eldridge, whose company is currently working on a recurrent UTI vaccine.
- UTIs also have been found to be increasingly resistant to antibiotics as well.
- Tara deBoer, postdoctoral researcher at UC-Berkeley, says her team is focused on UTIs because if the appropriate antibiotic is not given to the patient right away, "the infection moves from the bladder to the kidneys and there's a big risk of it moving toward the bloodstream..."
What's next: Because it's such a huge problem, there's lots of active research, including into new vaccines. Eldrige says his company, Sequoia Sciences, is also working on a recurrent UTI vaccine, for example.
Researchers are also focusing on better diagnostics and treatment. DeBoer, who's also the founder of BioAmp Diagnostics, says her startup is working on improving the DETECT diagnostics test developed by her team at Berkeley. It's designed to help doctors know right away if patients have a UTI bug that's resistant to the largest class of antibiotics, known as beta-lactam antibiotics. They hope to have this product ready in 3 to 5 years.
There's also a push for better treatment. A recent study in the U.K. shows that a machine-learning tool might be able to improve the treatment of sepsis by cross-referencing patient variables with its database to determine optimal treatments.
Go deeper:
