Axios Vitals

March 10, 2022
Good morning.
Today's word count is 890, or a 3-minute read.
1 big thing: Pharmacists push for enhanced role in post-pandemic life
Illustration: Sarah Grillo/Axios
Pharmacies that say they've been a linchpin in the U.S. pandemic response are pressing for key regulatory changes and higher payment rates to cement their enhanced role in patient care.
Why it matters: Pharmacies have become fixtures of pandemic life through testing, vaccinations and, increasingly, dispensing antivirals.
Driving the news: The Biden administration's test-to-treat initiative, which began this week, has ignited a fierce debate over what pharmacists can and cannot do.
- The initiative allows patients to get tested for COVID in a pharmacy and be prescribed antivirals at the same location if they're found to be positive. But only pharmacies with qualified providers — like those with on-site clinics — can participate, under the FDA authorization for both Merck and Pfizer's COVID antivirals.
- Pharmacists are pushing for the FDA exclusion to be lifted.
The big picture: The push isn't the first time during the pandemic that pharmacists have argued they are well-qualified for a more active role in patient care.
Between the lines: Broadening pharmacists' formal role in patient care could open the door to them getting paid more.
- For example, pharmacists are currently only paid a fee for dispensing the antivirals by pharmacy benefit managers, which many have argued is prohibitively low. Other providers — like physician assistants and nurse practitioners — can bill for consultations and dispensing the pills.
- But even if pharmacists are allowed to order the pills for patients, there's no clear mechanism under current law for them to get paid the way other providers are, pharmacists say.
What we're watching: The pharmacists are set to lose their enhanced pandemic role when the public health emergency expires, setting up a test of how policymakers will approach a post-pandemic future.
2. COVID cases continue to plummet
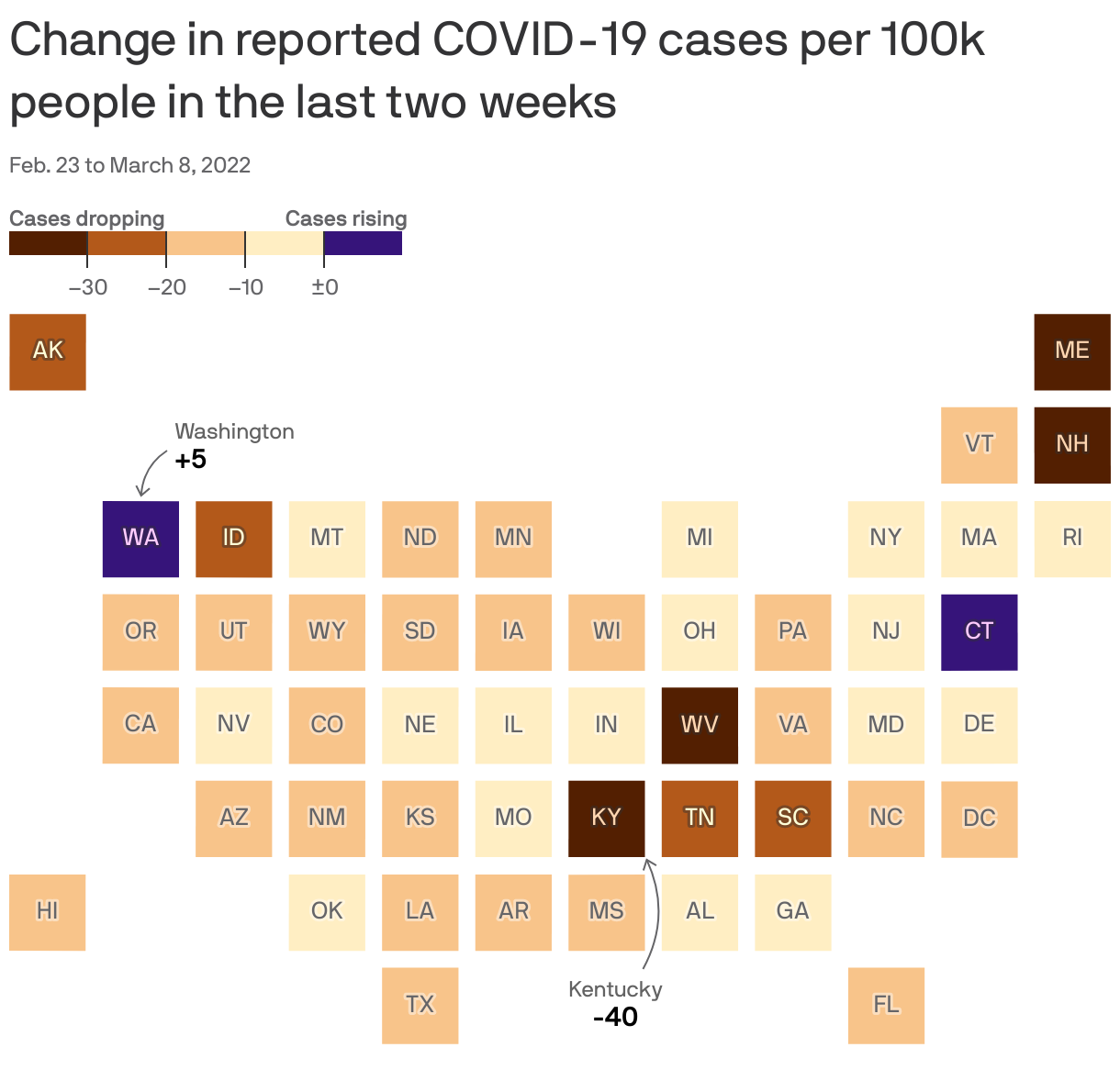
Coronavirus cases have continued to plummet nationally and in nearly all states, and daily deaths are also dropping, Axios' Kavya Beheraj and I report.
Why it matters: COVID precautions have already been lifted across most of the country as pandemic fatigue runs deep. The virus will probably be with us for the long term, but these improving metrics show Americans are moving on with their lives more safely.
By the numbers: Daily deaths fell by 24% over the last two weeks, from an average of more than 1,900 the week of Feb. 23 to 1,451 over the past week.
- Deaths fall only after the number of cases and hospitalizations do, because they're a lagging metric. Thus, a drop in the number of deaths is the truest sign that the Omicron wave is almost over.
- Cases fell by 48% over the same time period, and were averaging around 40,000 a day the week of March 8.
Yes, but: That daily death rate may be down from the pandemic peak, but it's still a lot of deaths, many of which are avoidable.
What we're watching: How low case rates fall is strongly connected with what the ongoing demand on the health system will be.
- Especially amid staffing shortages, hospitals only have so much capacity at any given time, meaning the baseline caseload going forward still matters.
3. New COVID funding in legislative trouble
Yesterday's twist in which billions in emergency COVID-19 funding got yanked from a sweeping congressional spending bill is scrambling the pandemic response at a critical moment, as the U.S. faces dwindling supplies of vaccines and therapeutics and a tapped-out pandemic account, Axios' Adriel Bettelheim writes.
Why it matters: The $15.6 billion for pandemic preparedness that House Democratic leaders had intended to pass as part of a massive funding package already wasn't enough to protect the U.S. from future waves of the virus.
- Deferring action could leave the country dangerously exposed if the virus re-emerges.
- "Without additional COVID response resources, the results are dire: In March, testing capacity will decline; in April, the uninsured fund — which offers coverage of testing and treatments for tens of millions of Americans who lack health insurance — will run out of money; and in May, America's supply of monoclonal antibodies will run out," said a White House official.
Background: The administration primed Congress for a COVID funding request.
- But Democrats fractured over the way the spending deal would have offset the cost of half of the new COVID aid by clawing back state and local funds already allocated in last year's American Rescue Plan.
What's next: The House released a revised version of the COVID relief legislation, which doesn't claw back the funding, as a standalone bill. But that will almost certainly die in the Senate.
4. Border dispute may threaten plasma supply
Drug companies have asked federal courts to overturn the U.S. border officials' decision to stop allowing Mexican nationals to cross the border to be paid to donate blood plasma, the Wall Street Journal reports.
Why it matters: The plasma is a critical component of treatments for some neurological and autoimmune diseases, and pharmaceutical companies have said that up to 10% of the plasma collected in the U.S. usually comes from Mexican nationals who have entered the country on visitor visas.
- U.S. officials stopped the practice last year because they viewed it as labor for hire, which isn't allowed under visitor visas.
What they're saying: Advocacy groups are concerned about how the change will affect patients dependent on treatments made from plasma.
- "We're very, very nervous that we're just on the cusp of possibly a very major shortage," Lisa Butler, executive director of Philadelphia-based GBS|CIDP Foundation International, told the Journal.
Sign up for Axios Vitals

Healthcare policy and business analysis from Tina Reed, Maya Goldman, and Caitlin Owens.
