Axios Vitals

September 05, 2024
Happy Thursday! Today's newsletter is 999 words or a 4-minute read.
🚨 Situational awareness: Buffalo Bills safety Damar Hamlin is due to start in the team's season opener on Sunday for the first time since he suffered a cardiac arrest during a Monday Night Football game in January 2023.
1 big thing: Data tracking flap shows HIPAA limits
The end of a dispute between the Biden administration and hospitals over their use of website tracking technology could leave patients' data vulnerable to being shared with online marketers, data brokers, and social media platforms.
Why it matters: The case highlights the limits of the Health Insurance Portability and Accountability Act, which dates to 1996 and wasn't designed for the digital age.
Driving the news: The Department of Health and Human Services last week dropped an appeal after a federal judge in Texas in June ruled it overstepped its authority by blocking hospital websites from using tracking technologies that capture IP addresses on their public-facing webpages.
- The American Hospital Association sued HHS last year after the agency told hospitals that they were violating HIPAA by using the tracking tools.
The big picture: Websites scoop up data to improve user experience of the site, track the success of their content, and retool it for more clicks.
- But privacy experts say third-party companies could collect crumbs of information from website visits that can reveal personal health information to data brokers and advertisers.
Between the lines: Hospitals say they've been put in a tough position and applauded HHS' decision to abandon its appeal.
- "They were putting these restrictions that could expose hospitals to civil penalties for every YouTube video on the value of COVID vaccines if we gave IP addresses to Google," said American Hospital Association general counsel Chad Golder.
The other side: Many patients may not feel comfortable with their health provider sharing with third parties every search for health information, said University of Pennsylvania researcher Matthew McCoy, who studies the use of trackers on hospital websites.
2. Health worker squeeze will vary by state
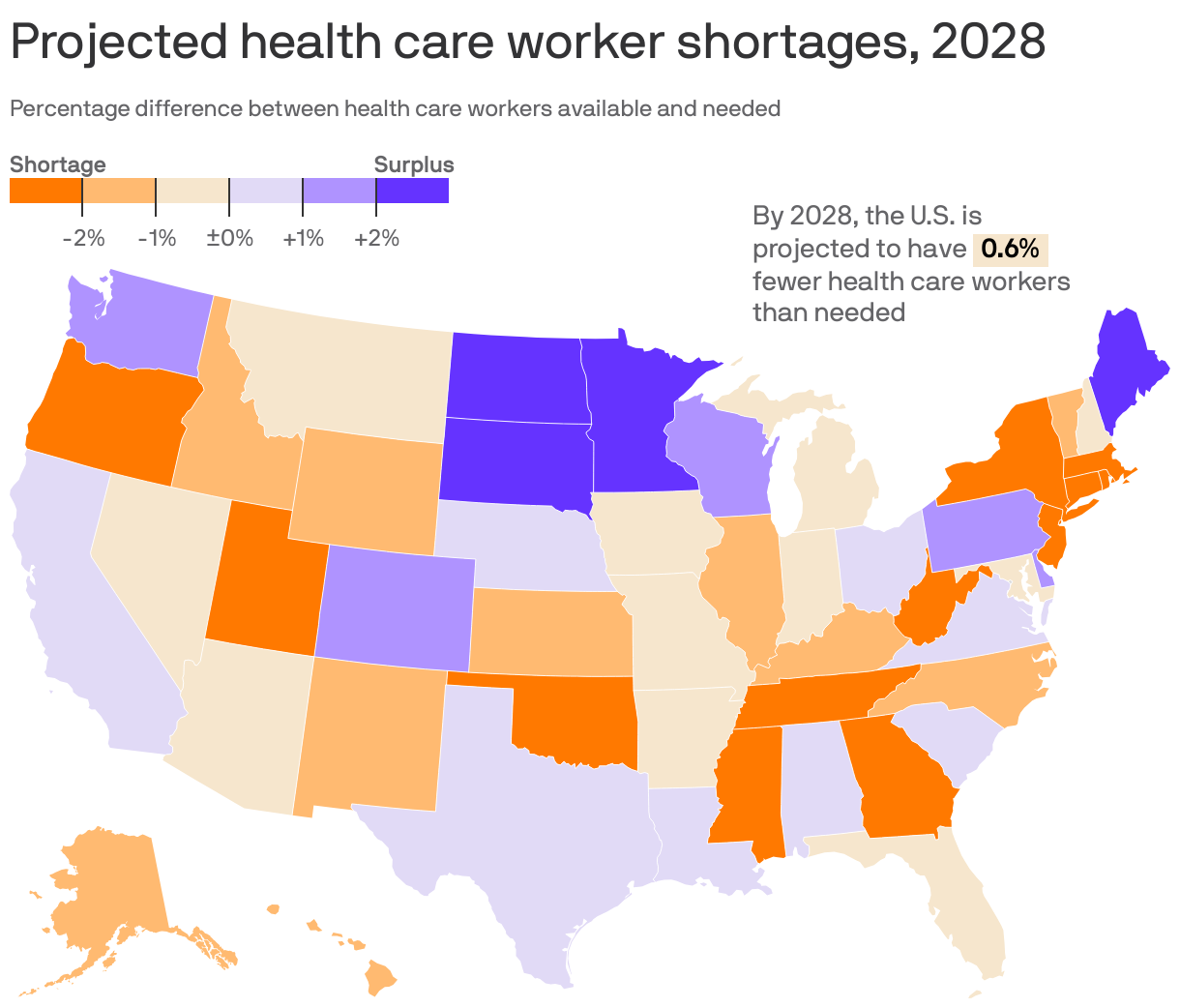
Continued worker burnout and more demand for care from an aging population will drive health care workforce shortages into 2028 — though with significant variations by state, according to a Mercer analysis.
Why it matters: While there's been considerable attention paid to physician shortages, the analysis highlights an acute need for more nurse practitioners, even in states like California and Texas that will have overall surpluses of health workers.
By the numbers: The U.S. is expected to be short 100,000 health care workers by 2028, Mercer projects.
- New York will be short about 61,000 health care workers, or a more than 4% gap between supply and demand. New Jersey, Tennessee, Georgia, and Florida could all be more than 10,000 workers short of meeting patient demand.
- North Dakota, meanwhile, will have a nearly 5% surplus of health care workers by 2028.
Zoom in: Most states should have enough registered nurses to meet patient needs in 2028, and the country as a whole is expected to have a surplus of 30,000 RNs that year.
- But nearly every state will be short of nurse practitioners, despite employment of NPs growing faster than nearly all other jobs, per the Bureau of Labor Statistics. Only 13 states will be able to meet the demand for nursing aides.
3. Humana exiting 13 Medicare Advantage markets
Humana said yesterday it plans to leave 13 Medicare Advantage markets next year and scale back plan offerings in other areas, in the latest insurer response to financial pressures in the program.
Why it matters: Hundreds of thousands of enrollees will have to find new doctors or make other care arrangements.
Driving the news: Humana CFO Susan Diamond told the Wells Fargo Healthcare Conference in Massachusetts that the insurer is dropping out of counties where performance has been unsatisfactory and expects to lose a few hundred thousand enrollees as it prioritizes profitable markets, Modern Healthcare reported.
- She didn't specify what markets will be affected, but said Humana will continue selling MA plans in every state and is committed to attractive regions like South Florida, the publication reported.
Catch up quick: Other big MA players like UnitedHealth, CVS Health, and Centene have been sizing up their options since the Biden administration this spring cut base payments for 2025 as part of a plan to make MA payments more accurate.
Zoom out: More than half of Medicare enrollees now get their coverage from MA plans, which experts say are overpaid and cost taxpayers tens of billions of dollars more than they should.
- The health plans point to rising costs from higher demand for medical services as patients catch up on care deferred during the pandemic.
4. Pap smear alternative being sent to providers
The first self-collection kits for cervical cancer screening were shipped to doctor's offices and other health care facilities today, Axios has learned, providing patients with an alternative to Pap smears.
Why it matters: The less-invasive self-swabs allow health clinics that don't have speculums, stirrups, and other equipment to start offering screening.
- It's an alternative to Pap smears, which can cause extreme discomfort, including for those patients with a history of sexual trauma or chronic pain.
The big picture: About a quarter of U.S. women are overdue for cervical cancer screening, according to the National Cancer Institute. Women in the South, where screening and preventive care lag behind the rest of the country, are more likely to die from the treatable disease.
State of play: The Food and Drug Administration approved the test from BD (Becton, Dickinson and Company), along with a version by Roche, in May. Roche's test will be available later this fall, the New York Times reported last month.
- Australia, Denmark, the Netherlands, and Sweden already use self-collected cervical cancer swabs.
How it works: The new test allows patients to collect their own sample of cells from vaginal walls while at a doctor's office, much like they'd take their own urine sample, said Jeff Andrews, vice president of global medical affairs for diagnostic solutions at BD.
5. Catch up quick
📈 New breast cancer diagnoses among Asian American and Pacific Islander women are rising much faster than in many other racial and ethnic groups. (KHN Health News)
🦠 A Mayo Clinic study suggests that being vaccinated against COVID-19 does little to prevent long COVID. (CIDRAP)
🐖 A startup that genetically edits pig organs for human transplant won a new round of venture capital funding. (Axios)
Thanks for reading Axios Vitals, and to senior health care editor Adriel Bettelheim, managing editor Alison Snyder, and copy editor Patricia Guadalupe. Please ask your friends and colleagues to sign up.
Sign up for Axios Vitals



/2024/09/04/1725489866009.gif?w=3840)

