Axios Vitals

March 22, 2022
Good morning, Vitals readers. Today's newsletter is 776 words or a 3-minute read.
1 big thing: The future standard of COVID surveillance
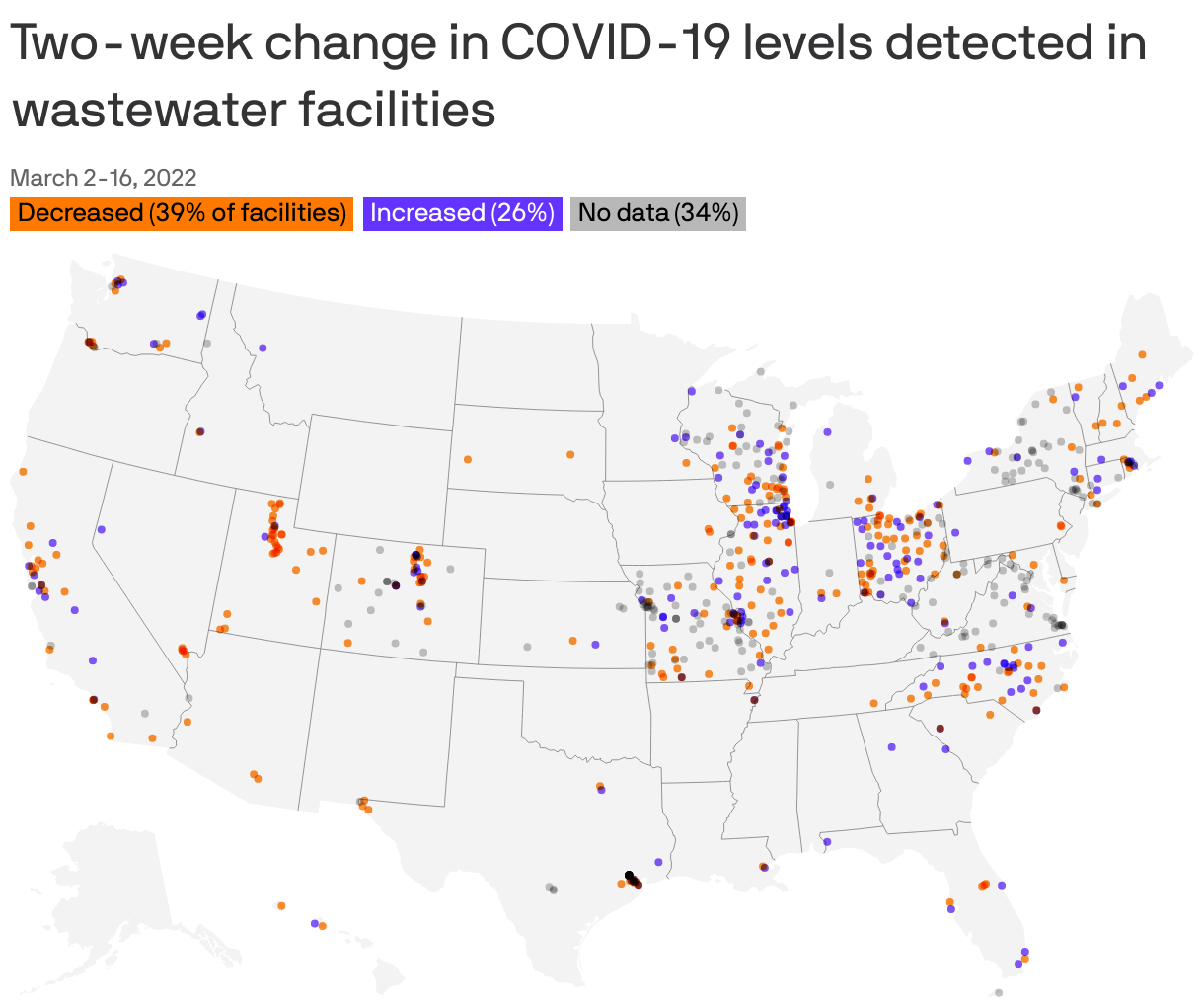
A COVID-19 wave similar to Europe's may soon arrive in the U.S. But public health authorities aren't getting a full picture because a hoped-for national early warning system remains a patchwork quilt, Axios' Kavya Beheraj and I report.
State of play: More than 700 sites around the U.S. report wastewater surveillance data to the National Wastewater Surveillance System, set up by the CDC in 2020 to identify case surges and new variants.
- Plenty of places around the country including Washington, D.C., as well as Chicago, Des Moines and the Twin Cities are using sewage surveillance.
- But as Politico recently reported, many sites don't regularly report, and only 12 states routinely submit data, leaving "gaping holes" in surveillance.
- There's also concern that the dashboard can be misinterpreted because it reflects percentage changes in virus detection with only limited context, Kaiser Health News reported.
Yes, but: Wastewater surveillance gained wide acceptance in the 1990s with efforts to eradicate polio. Experts say investment in this kind of testing is "critical" as research has shown it can be used to accurately track trends in COVID-19 transmission.
- "[The CDC] and others should be focused on ramping up this critical surveillance tool — a minimum 100x around the US. The cost is pennies compared to the cost of being taken off guard (again)," tweeted Michael Mina, chief scientific officer at the biotech software company eMed.
- It's additionally important with the broad adoption of at-home testing, whose results don't always reach health departments, Mark Osborn, who leads efforts to collect wastewater surveillance for the state of Minnesota, told Axios.
- "Everyone will use a drain at some point during the day," he said. "We lose a bit of the analytics we had earlier in the pandemic where you had to go to a clinic to get tested and all those results went to the Department of Health."
2. Little follow up on opioid addiction drugs
Fewer than a third of patients who were given drugs in emergency departments to treat opioid addiction follow up and continue their treatments, Axios' Adriel Bettelheim reports from a new RAND Corp. study.
The big picture: Emergency departments give the drug buprenorphine to individuals with opioid addiction who don't already receive medication treatment, then link the patients to health providers who can provide ongoing care.
- But that only works if local clinicians are accepting new buprenorphine patients. Studies indicate many aren't treating large numbers of patients or not accepting new ones.
By the numbers: The study in the Annals of Emergency Medicine looked at 92% of prescriptions filled at U.S. retail pharmacies before and during the pandemic and found 71.5% of patients who filled buprenorphine prescriptions from emergency physicians didn't fill subsequent scripts from other clinicians — a trend that intensified after the public health emergency was declared.
The bottom line: Researchers say there may need to be new initiatives, like creating bridge clinics, to help people transition to community care, as well as payment changes.
3. Increased diabetes risk linked to COVID
Illustration: Annelise Capossela/Axios
Those who've recovered from COVID-19 within the past year have a significantly increased chance of being diagnosed with Type 2 diabetes compared with people who haven't been infected, a study published Monday in the journal Lancet Diabetes and Endocrinology found.
Why it matters: The increased risk translates into 1% of people who've gotten COVID developing diabetes "who otherwise wouldn't have," the Wall Street Journal reported.
By the numbers: Researchers used the national databases of the Department of Veterans Affairs to build a cohort of 181,280 participants who had a positive COVID-19 test between March 2020 and September 2021.
- They said the disease mechanism isn't clear, but they suspect it could be due to direct factors such as a hyperactivated immune response or broader environmental changes from the pandemic that might have indirectly helped shape outcomes.
⚡️ 4. Health care industry lightning round
- Three kidney care providers — Fresenius Health Partners, Cricket Health and InterWell Health — plan to merge in deal valued at $2.4 billion. (Fierce Healthcare)
- Computational journalism startup Applied XL raised $3.5 million to focus on the life sciences with "broader ambitions" to address the "health of people, places and the planet." (Axios Pro)
- Even as Novavax's COVID shots began going into arms in the Netherlands on Monday, its stock fell amid weak vaccine uptake in Germany. (Motley Fool)
5. Quote du jour
"I’ve been included in a kind of imaginary version of the United States, because a lot of these pandemic plans sort of pretend that vulnerable people like me live often in a little bubble somewhere. And we don't."— Beatrice Adler-Bolton, a disability justice advocate and writer based in New York told Axios Today podcast host Niala Boodhoo about how immunocompromised individuals are coping with the end of COVID restrictions.
Sign up for Axios Vitals

Healthcare policy and business analysis from Tina Reed, Maya Goldman, and Caitlin Owens.