Infertility treatments could become more inclusive, accessible for Californians
Add Axios as your preferred source to
see more of our stories on Google.
A new, more expansive definition of "infertility" could bring help to hopeful LGBTQ+ and single parents in California and beyond.
Why it matters: Redefining the condition could lead to broader insurance coverage of fertility services like egg freezing and in vitro fertilization for all people who need help starting families — not just heterosexual couples.
- It could also bolster ongoing legislative efforts to make fertility coverage more inclusive in states like California, where some prior attempts have failed.
Driving the news: The American Society for Reproductive Medicine redefined infertility to include people who need medical intervention, such as donor eggs or sperm, to achieve pregnancy.
- It's no longer limited to when a man and a woman can't get pregnant after a year of unprotected intercourse or intrauterine insemination — or six months for women over 35.
- The updated language applies to anyone who needs help having children, regardless of relationship status, gender identity or sexual orientation.
Between the lines: "There's been a real issue with getting access to treatment for certain causes of infertility including for single people [and] people in same-sex relationships … so it became clear that we need to explicitly address that," ASRM spokesperson Sean Tipton told Axios.
Zoom in: California only requires insurers to offer infertility treatment coverage, but that does not include IVF coverage, according to infertility advocacy group Resolve.
- Religious organizations and employers who are self-insured are exempt.
- Meanwhile, the state does require health insurance companies to cover the cost of fertility preservation procedures, which is particularly helpful for cancer patients.
What we're watching: While the new "infertility" definition creates one avenue to more inclusive coverage, California legislators are pursuing another.
- State lawmakers are considering a bill that would require health insurance plans to cover the diagnosis and treatment of infertility and fertility services, including IVF.
- It also expands the definition of infertility to include coverage for LGBTQ+ individuals and surrogates.
- "Historically, many cannot afford the out-of-pocket costs of treatment, and LGBTQ+ individuals have been largely excluded in California due to a hetero-normative definition of infertility," state Senator Caroline Menjivar said in a statement.
- Yes, but: Previous legislative attempts to expand coverage to include IVF, diagnosis and treatment for single persons, same-sex couples and transgender people stalled.
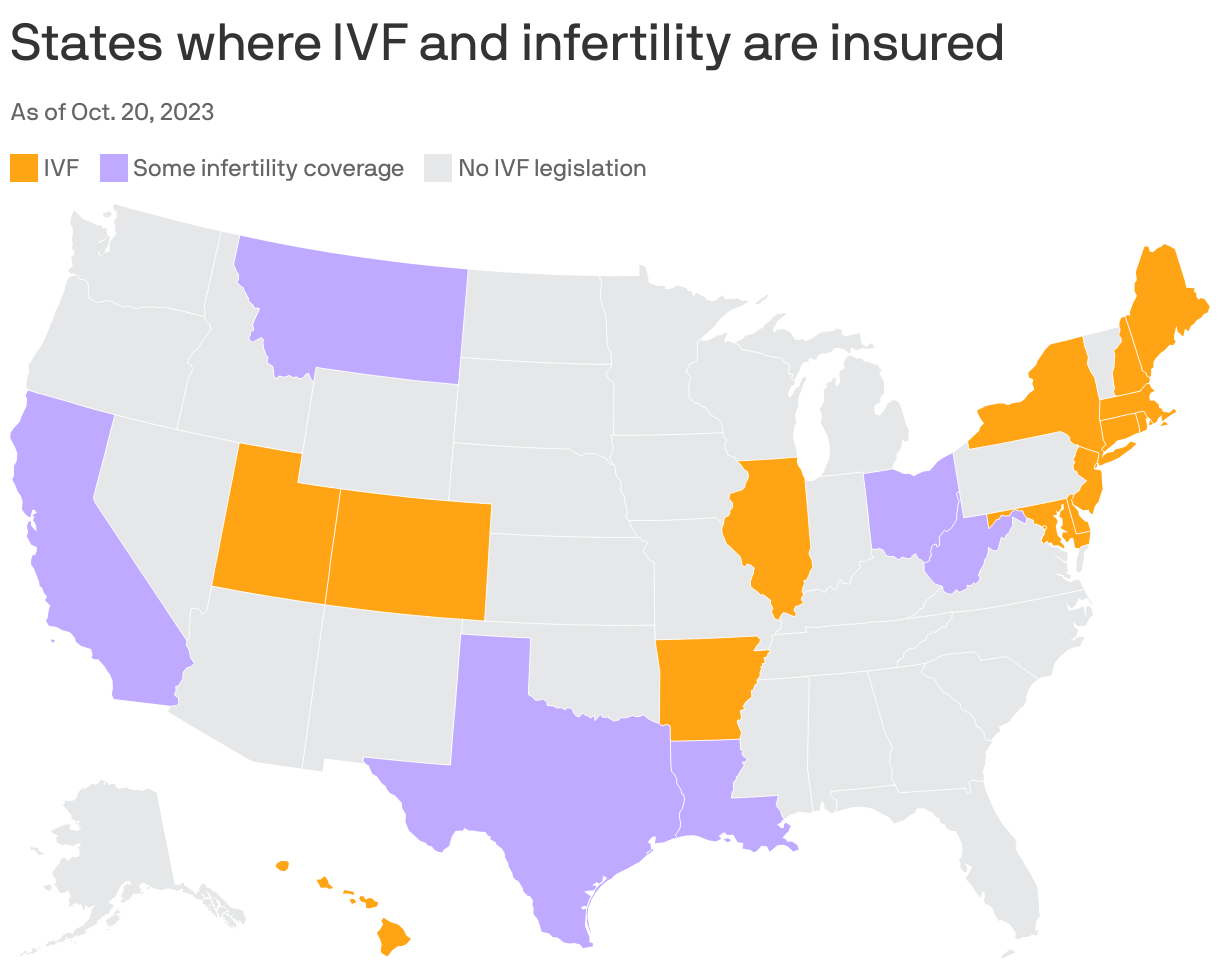
Zoom out: As of now, 21 states plus Washington, D.C., require some workplace health plans to cover at least some form of fertility coverage. Of those, only eight states have policies inclusive of LGBTQ+ communities and single parents, according to Betsy Campbell, chief engagement officer at Resolve.
State of play: Despite the growing interest in fertility care — and more employers offering fertility benefits to stay competitive in the labor market — insurance coverage for the often-expensive services remains limited.
- IVF is pricey, with the average cost of one cycle is $12,400, according to ASRM.
- Still, several studies suggest fertility insurance coverage does not significantly increase the cost of medical plans.
What they're saying: A more inclusive definition of infertility is "a game-changer," because a number of insurance plans rely on the ASRM definition of what's a disease to determine coverage, infertility specialist Lucky Sekhon told Axios.
- With this update, "insurance companies can't discriminate. … It gives people ammunition to fight policies for more coverage," she says.

