Monkeypox messaging debated as outbreak enters new phase
Add Axios as your preferred source to
see more of our stories on Google.
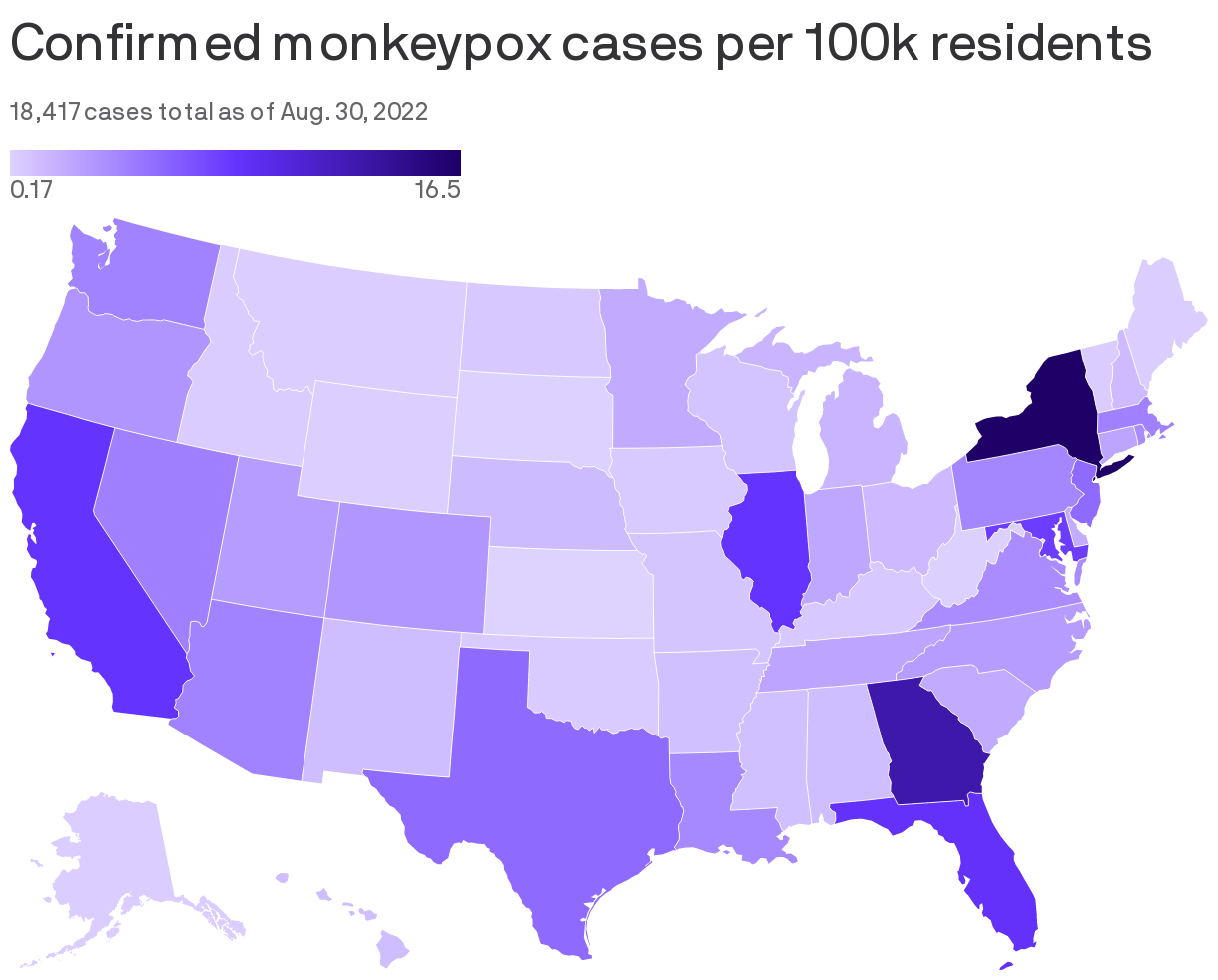
Monkeypox cases may be slowing in the U.S., but the perils of communicating who is most at-risk and getting those people the resources they need is still challenging public health officials and providers.
Why it matters: Monkeypox infections are seen primarily among men who have sex with men, but emphasizing that transmission route risks stigmatizing gay and bisexual men.
- The head of the World Health Organization urged men at risk to reduce the number of sexual partners "for the moment" while WHO officials emphasized that monkeypox can infect anyone in close contact with an infected person.
- The CDC has made no such recommendation, saying anyone can get monkeypox. But the agency adds it's "using specific channels" to send information about the illness to gay and bisexual men of different racial and ethnic backgrounds.
Driving the news: After three months of rising caseloads, the global outbreak may be peaking amid evidence of less risky sexual behavior among gay and bisexual men and more people getting vaccinated, the Washington Post reported, citing its own tracking over seven days.
- But messaging around the risk is becoming even more critical as the virus spreads to smaller outlying communities and vaccine supplies tighten.
- The experience of COVID and HIV showed an inverse relationship between those at greatest risk and those who get vaccinated, which can worsen health disparities, pooling disease in a "viral underclass," Northwestern University professor Steven Thrasher wrote in Scientific American.
- "There's a concern that people getting vaccines may not be the ones most at-risk," Anna Person, a physician at the Vanderbilt Comprehensive Care Clinic, which serves HIV patients, told Axios.
Between the lines: A key point of contention is whether to classify monkeypox a sexually transmitted infection, like HIV, or herpes, which also have multiple modes of transmission.
- Some like Thrasher say it's important to understand how infections are transmitted sexually to understand mechanisms of disease and prevent transmission whenever possible.
- Testing for monkeypox during routine STI screenings would give a higher-resolution view. Authorities should also study why people with very low levels of HIV are overrepresented among monkeypox cases, Thrasher wrote.
Yes, but: That categorization could downplay how monkeypox can be transmitted through other types of close contact and risks stigmatizing sex between men.
- "You can recognize that there are differences and that's important to do, but it doesn't mean it has to be the emphasis or message of the campaign. It just tells you who the messaging needs to go to," Joseph Lee, a professor of health education and promotion at East Carolina University, told NPR.
And yet, there are few cases cases confirmed in children, women or close household contacts of monkeypox patients.
- "People should recognize that while different routes of transmission are possible, we have very few cases like this," Abraar Karan, a Stanford University infectious diseases fellow, said of a patient who tested positive after international travel and no reported sexual contact.
The big picture: Health agencies and providers are figuring out a communications strategy while having to make do with dwindling resources and dealing with growing equity issues.
- The vast majority of vaccines and treatment have gone to white people so far, CDC data show.
- In the most recent week of data available, 33% of confirmed cases were in Black people; 32% were in Hispanic people and 30% were among white people.
- Vaccine data that collected the race of the recipient show that 50% of those with first doses are white, however, while 24% with first doses are Hispanic and just 11% were Black.
- There are 17,431 cases confirmed nationwide, a likely undercount.
The bottom line: Whether or not cases keep falling largely depends on the ability of providers to get vaccines out to those who need them most, and raising awareness in communities at risk.
- "Take vaccines out to people who need it rather than expecting them to come to us to get vaccinated," said Wafaa El-Sadr, a Columbia University epidemiologist who heads the International Center for AIDS Care and Treatment Program.
