Despite insurance coverage, few people with hepatitis C get treatment
Add Axios as your preferred source to
see more of our stories on Google.
Only a fraction of the more than 2 million American adults with Hepatitis C are getting antiviral treatments, even when their insurance will pay for it, the Centers for Disease Control said in a report out Tuesday.
Why it matters: Hepatitis contributes to about 14,000 U.S. deaths a year, and the opioid crisis and the unsanitary use of needles by drug users has driven a spike in cases.
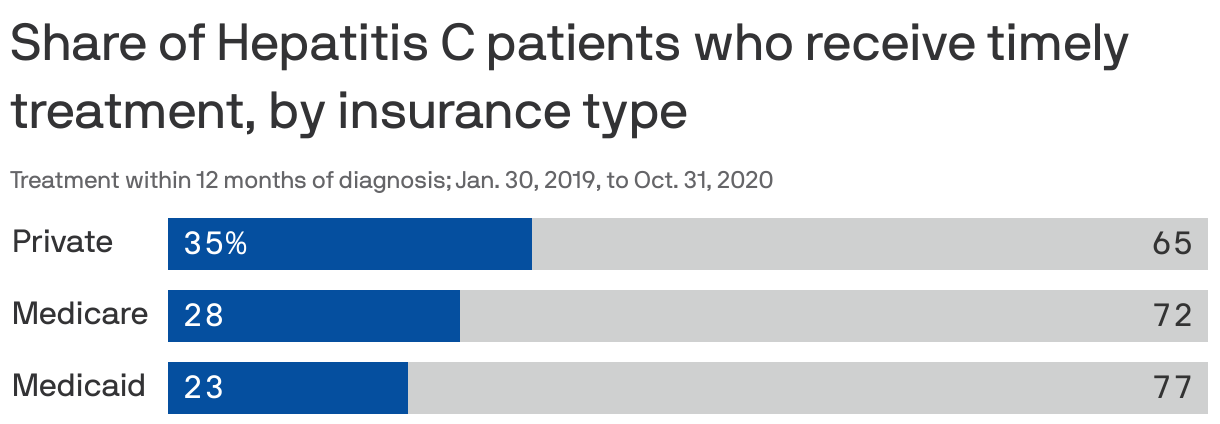
Driving the news: Just one in three people with diagnosed hepatitis C who have private insurance started treatment after diagnosis, and just one in four people with Medicare and Medicaid did so in that same timeframe.
- Younger adults, under the age of 40, are accessing treatment at the lowest rates, which concerns health officials since this is the group most likely to spread hepatitis C.
- Medicaid patients had lower odds of starting treatment in states with prior authorization restrictions and other barriers to care.
- Medicaid recipients who were white were likelier to start hepatitis C treatment than nonwhite patients, the CDC report shows.
Flashback: Cost is a major factor. The latest and most effective drug was approved by the FDA in 2014, but a course of this medication could cost upwards of $90,000 when it was first made available.
- While the number of patients seeking treatment increased from 2014 to 2015, barriers like limited insurance coverage to lack of providers offering treatment have driven case rates higher and treatment rates lower over the past decade, despite the cost of the treatment dropping.
- "Availability and accessibility of treatment are not the same," Jonathan Mermin, CDC director for hepatitis prevention, told reporters Tuesday.
The bottom line: CDC officials are pressing states, providers and insurers to do more to enable access to treatment, especially for people with substance use disorders.
