Profits swell when insurers are also your doctors
Add Axios as your preferred source to
see more of our stories on Google.
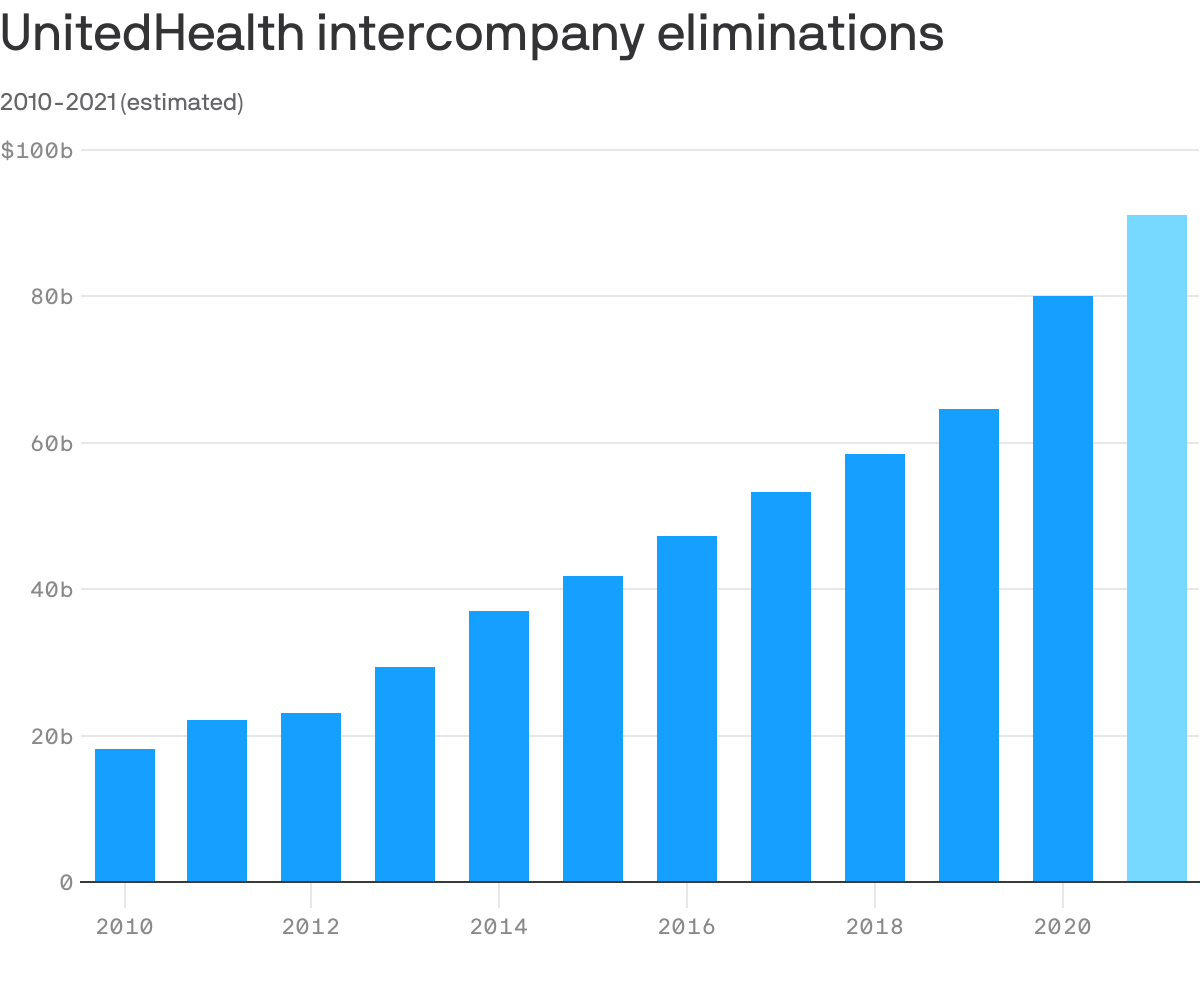
UnitedHealth Group isn't just making more money because people deferred care throughout the coronavirus pandemic. It's making more money because it's owning a bigger piece of the health care system.
The bottom line: Insurers keep more of the premiums they collect when they also own the medical providers that are paid those premium dollars. And no insurer has expanded as aggressively into care delivery over the years as UnitedHealth.
Zoom in: Each quarter, UnitedHealth reports what it calls "intercompany eliminations."
- This is when money transfers from one part of the company to another. UnitedHealth can't record the transaction as revenue because it is just paying itself.
- For example, if a worker with UnitedHealthcare insurance goes to a surgery center or physician practice owned by Optum? That's an intercompany elimination. A 70-year-old with a UnitedHealthcare Medicare Advantage plan fills a prescription through Optum's specialty pharmacy? That's one, too.
By the numbers: UnitedHealth recorded $43.8 billion of eliminations in the first half of 2021, putting it on pace for roughly $91 billion for the entire year.
- That amount would be four times as much as the eliminations UnitedHealth recorded a decade ago.
The big picture: Federal law caps health insurance profits to 15-20% of collected premiums, depending on the type of market.
- But there are no limits to how much profit a provider can keep. So if an insurer can steer its members toward its own providers, the company is able to keep a lot more of those premium dollars.
- It's no surprise, then, that other insurers like Bright Health are mimicking what UnitedHealth has been doing.
