May 10, 2021 - Health
Some health providers are charging insurers over $1,000 for COVID tests
Add Axios as your preferred source to
see more of our stories on Google.
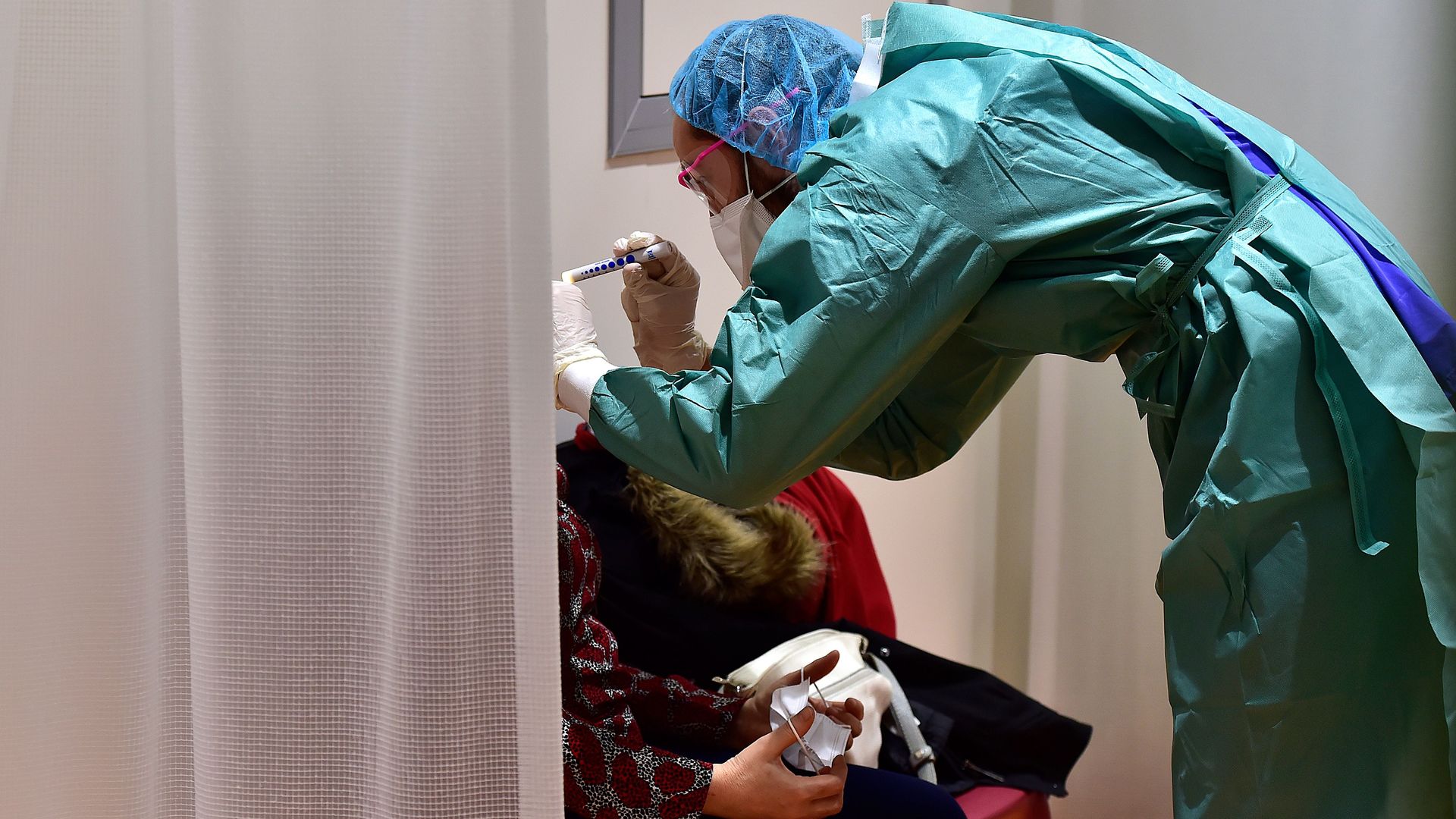
Photo: GEORGES GOBET/AFP via Getty Images
Add Axios as your preferred source to
see more of our stories on Google.

Photo: GEORGES GOBET/AFP via Getty Images