Scientists successfully grow entirely new skin for 7-year-old
Add Axios as your preferred source to
see more of our stories on Google.
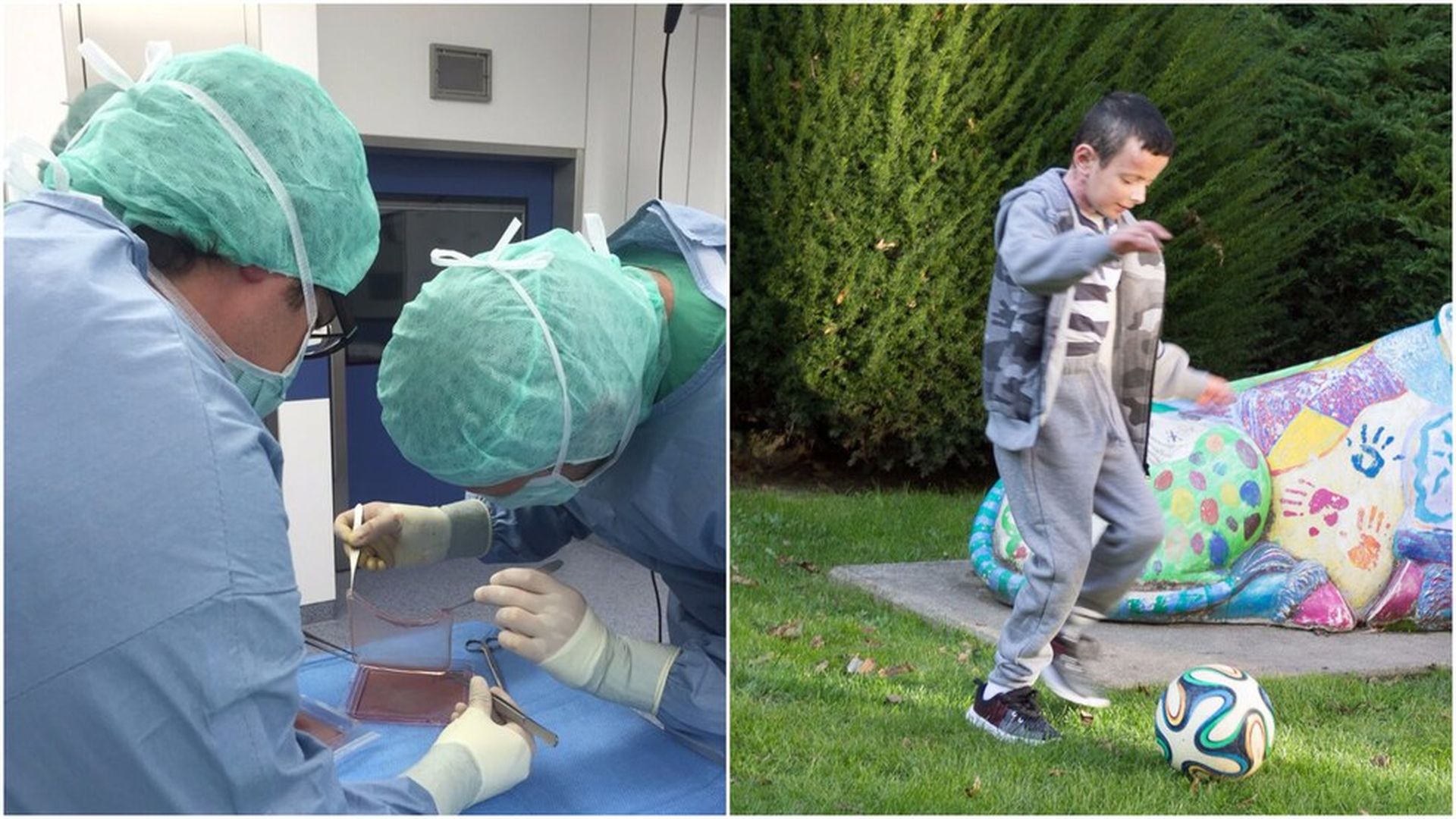
One of the transplant procedures (on left) that helped the patient (on the right). Photos: Ruhr-University Bochum
Scientists successfully used stem cell and gene therapy to replace 80% of the skin of a 7-year-old boy affected by an incurable genetic skin disease, they report Wednesday in Nature.
Why this matters: This is the first time researchers have been able to regenerate virtually the entire epidermis and also provides a blueprint for other stem cell and gene therapies. And, while the scientists cautioned more testing is needed to see if this could be used for the roughly 500,000 people worldwide with different forms of this particular disease, they said this experiment was a success.
"The kid is now back to school, is playing soccer and spending holidays with other kids," one of the study authors, Tobias Hirsch, said during a conference call with journalists.
The disease: The patient has junctional epidermolysis bullosa (JEB), which is a severe and often lethal genetic disease caused by mutations in one of three genes: LAMA3, LABM3 or LAMC2. The disease affects the protective outer layer of the skin, called the epidermis, but often not the inner layer, called the dermis. JEB makes the epidermis fragile, causing it to blister easily and eventually creating open untreatable wounds that can lead to infections, cancer and death. In his case, morphine was used to control the pain associated with the disease.
The backstory: The boy was admitted to the burn unit of a children's hospital in Germany after a 6-week infection, with complete epidermal loss on 60% of his body. All therapeutic approaches at the hospital failed, including a regime of antibiotics, constant dressings and nutrition, and a rejected skin transplant from the father.
The patient's doctors, Hirsch and Tobias Rothoeft, reached out to Michele De Luca from the Centre for Regenerative Medicine at Unimore in Italy. De Luca, who in prior experiments had successfully grafted small patches of epidermis for a couple of patients, agreed to join them.
"[S]caling up the process should not be minimized. This is a huge undertaking and the fact that it worked essentially with the first grafts that were placed is pretty remarkable," George Cotsarelis, a dermatologist at the University of Pennsylvania who was not part of this study, told Axios.
What the researchers did: The team of scientists took a small biopsy from the part of the boy's skin without lesions, genetically corrected the LAMB3 gene, and grew a transgenic epidermal graft that contained a mix of stem cells (holoclones) and two other cell types: paraclones and meroclones. They did three separate grafts and tested the skin regularly to see how the skin changed, since skin tends to regenerate itself roughly once a month.
What they found: "His epidermis is stable, robust, and doesn't blister at all, and his functionality is quite good," De Luca said during the conference call. Hirsch added that as opposed to other graft patients, parts of the new skin on this boy shows some hair follicles and the patient does not need to use ointment, which is something other graft patients tend to require for the rest of their life.
De Luca said the recipe for success appears to be the combination of the three types of cells, with the stem cells as the key for long-term stability.
Follow up: Rothoeft said the patient went from "being on morphine the whole day to no drugs at all at the moment." He said the team is debating on whether they should replace the small percentage of the boy's skin that has not yet been grafted, since those areas continue to blister.
What it means for others: "The Herculean efforts required to perform this type of procedure make it difficult to imagine commercializing this approach. The regulatory burden and the costs are astronomical," Cotsarelis told Axios. De Luca says they currently have two clinical trials to continue advancing the safety and effectiveness of these transplants. However, he warned that other forms of the disease may not have the same response since "that involves another gene, another protein, another location."
