Sep 7, 2018 - Health
Judge vacates Medicare Advantage overbilling rule
Add Axios as your preferred source to
see more of our stories on Google.
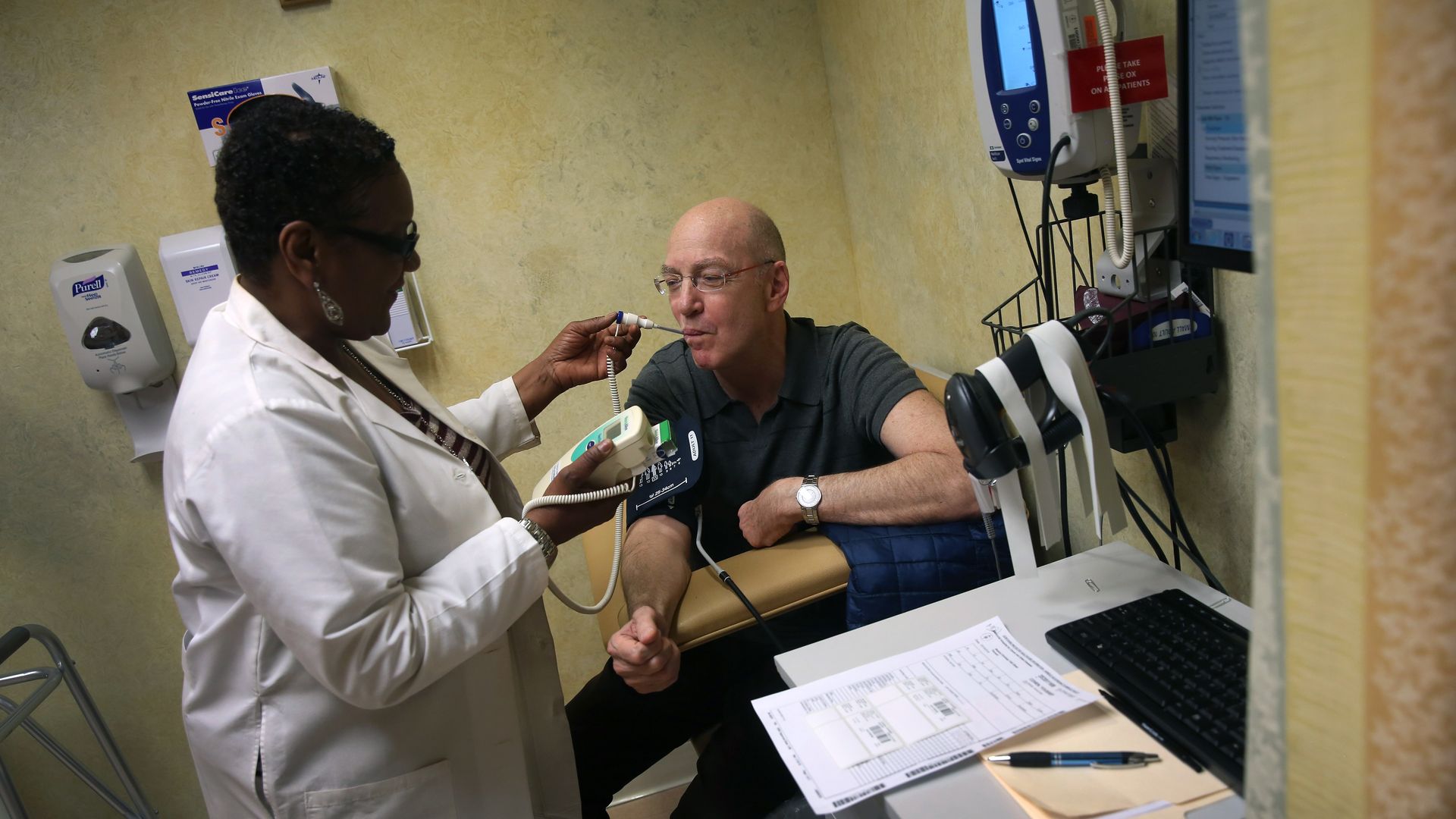
A nurse checks the vitals of an elderly patient. Photo: John Moore/Getty Images
Add Axios as your preferred source to
see more of our stories on Google.
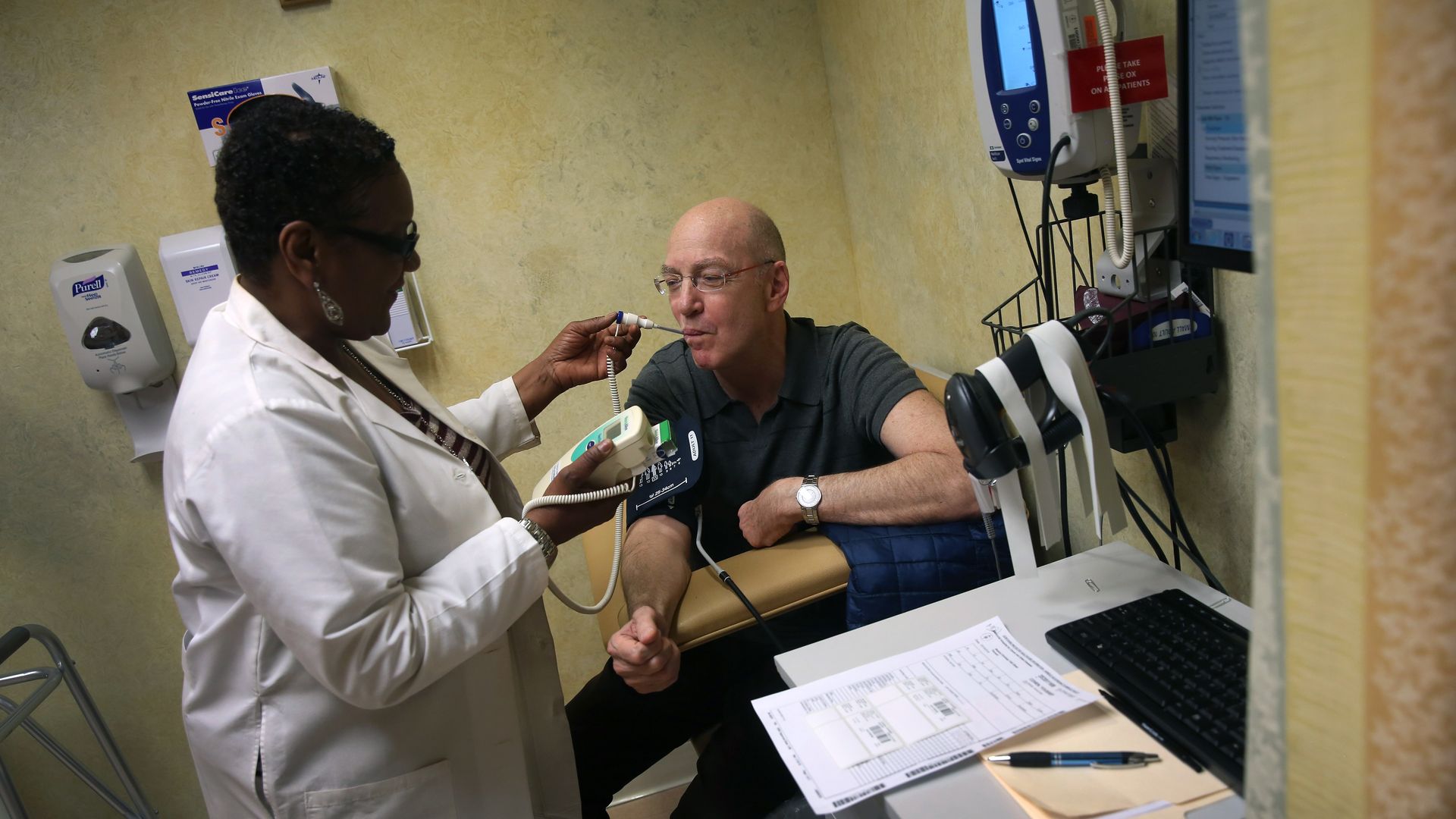
A nurse checks the vitals of an elderly patient. Photo: John Moore/Getty Images