Axios Vitals

May 27, 2025
Welcome back! Today's newsletter is 941 words or a 3.5-minute read.
1 big thing: Why Trump needs Congress on drug prices
One of the drug industry's biggest guardrails against President Trump's "most favored nation" drug pricing plan is the fact that it's less enforceable without the involvement of Congress.
Why it matters: Enshrining such a policy in law would be proof of GOP evolution on drug prices — or at least the party's willingness to break with its traditional aversion to government price-setting.
- It would also likely enable policy changes resulting in deeper reductions in what Americans pay for drugs, potentially slashing manufacturers' revenue and creating global disruption.
- But for now, Trump isn't asking much from lawmakers as they deal with a sweeping overhaul of Medicaid and government spending battles.
State of play: Trump issued an executive order this month calling for the U.S. to pay less for drugs than other comparable countries. Manufacturers are expected to hit targets based on the lowest price in Organization for Economic Cooperation and Development nations with a GDP per capita of at least 60% of the U.S. GDP per capita.
- Analysts have noted it isn't apparent how the plan would overcome legal hurdles.
- The EO "lacks a clear legal mechanism for implementation, a positive for the industry," Capstone analysts wrote. "Ultimately, any substantive price-setting beyond the Inflation Reduction Act's Medicare negotiation will be tested in litigation."
Flashback: Trump tried to enact a similar most favored nation policy during his first term, but it was halted by the courts after the drug industry sued. The idea was eventually abandoned by the Biden administration.
- The courts blocked Trump's plan based on how it was implemented, not on the merits itself — "something the administration could relatively easily fix," said Washington University law professor Rachel Sachs.
- But there were also legal challenges to the underlying policy, and there almost certainly would be again should the executive order ever translate into actual regulation.
2. Integrated behavioral health on the rise
Insurers increasingly are paying for behavioral health services that are delivered alongside primary care, according to a new claims analysis from Milliman.
Why it matters: The idea of coordinating mental health care with physical health care has been around since the 1990s. But Medicare billing codes created in 2017 have made such arrangements viable in both private and public insurance markets, the report shows.
Context: The system, known as the collaborative care model, involves having a patient's primary care provider, behavioral health manager and psychiatric counselor create and carry out a mental health treatment plan.
- Traditionally, mental health care is delivered separately from physical health care, which can make it difficult to coordinate across providers.
- The collaborative care model has been found to improve outcomes, and real-world evidence shows it can also reduce costs. Health systems began piloting the model using grant funding before Medicare introduced billing codes for the services.
What they found: The number of Medicare Advantage enrollees receiving behavioral health services through the collaborative care model has increased eightfold since billing codes became available in 2017.
- About 2,600 MA beneficiaries got collaborative care in 2018, compared with 20,780 in 2022, Milliman found.
3. Just how many Americans are taking GLP-1s now
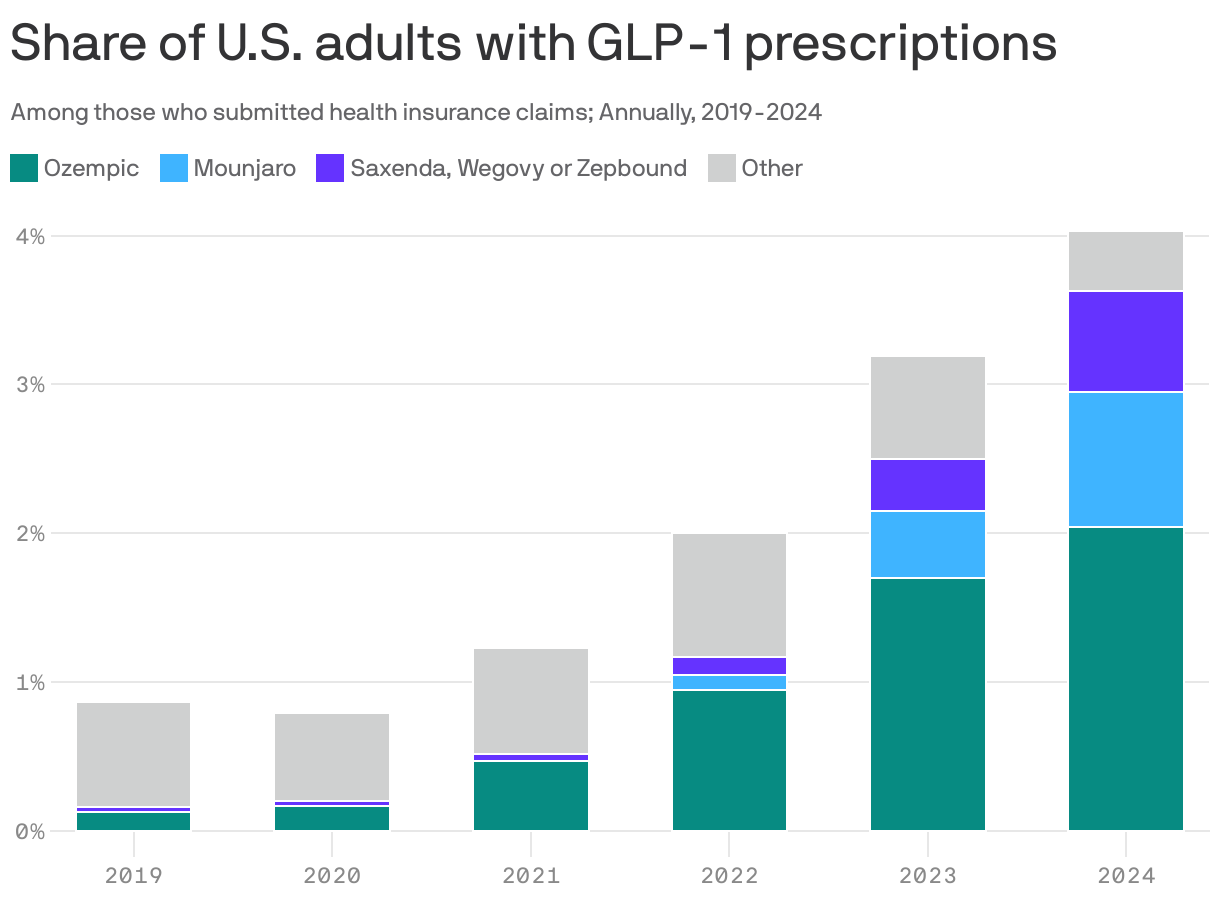
More than 2% of U.S. adult patients are taking GLP-1 drugs to treat being overweight or obese, up nearly 600% over six years, according to a report from FAIR Health provided first to Axios.
Why it matters: The data from FAIR Health's repository of over 51 billion commercial health claim records shows how use of the drugs specifically for weight loss has exploded and now accounts for roughly half of all users.
Details: In all, roughly 4% of Americans were taking GLP-1 drugs in 2024 for either overweight, obesity or Type 2 diabetes.
- The data shows Novo Nordisk's Ozempic is still by far the most commonly taken GLP-1, followed by Eli Lilly's Mounjaro.
- The percentage of adults who were prescribed a GLP-1 drug but did not have bariatric surgery increased from 2.5% in 2019 to 11.2% in 2024 while the the percentage of adult patients who had bariatric surgery decreased 41.8%.
Yes, but: The data still shows a dearth of treatment for patients with overweight or obesity.
- More than 80% of patients diagnosed as overweight or obese did not receive a GLP-1 prescription, bariatric surgery or behavioral health service in 2024.
4. Midi launches longevity program for women
The women's telehealth company Midi said Tuesday it's launching a longevity care program that will be covered by private insurers nationwide.
Why it matters: Longevity care is booming, but it mostly serves the wealthy. As preventive health messaging and midlife care becomes more common, telehealth businesses are pushing to broaden access.
Midi is advertising the program, called AgeWell, as the first longevity offering designed specifically for women — and covered by payers in every state.
- The company contracts with some major health insurers including Aetna, BlueCross BlueShield and UnitedHealthcare.
How it works: Accepted insurance will cover an annual diagnostic visit as well as hormone therapy, bloodwork and screenings. There isn't a membership fee, but copays could still apply.
- Patients who join will be asked to complete a panel of blood tests, come back for a virtual visit to discuss the results and receive a tailored care plan.
Yes, but: Some genetic tests are not yet covered. Also, Midi is not in network with managed care plans and doesn't participate in Medicaid or Medicare.
5. While you were weekending
👨🏼🍳 FDA commissioner Marty Makary suggested it would be more effective to treat diabetes with cooking classes instead of "just throwing insulin at people." (Independent)
👀 The VA's health care system has been plunged into crisis amid canceled contracts, hiring freezes and layoffs, internal documents show. (The Guardian)
🥬 An E. coli outbreak sickened more than 80 people. The public was not notified after an investigation. (KFF Health News)
Thanks for reading Axios Vitals, and to senior health care editor Adriel Bettelheim and copy editor Matt Piper. Please ask your friends and colleagues to sign up.
Sign up for Axios Vitals