Axios Vitals

September 03, 2019
Good morning. I can now blame my inability to function on less than 8 hours of sleep on my parents, who love naps just as much as I do.
Today's word count is 780, or ~3 minutes.
1 big thing: The war over Medicare Advantage audits
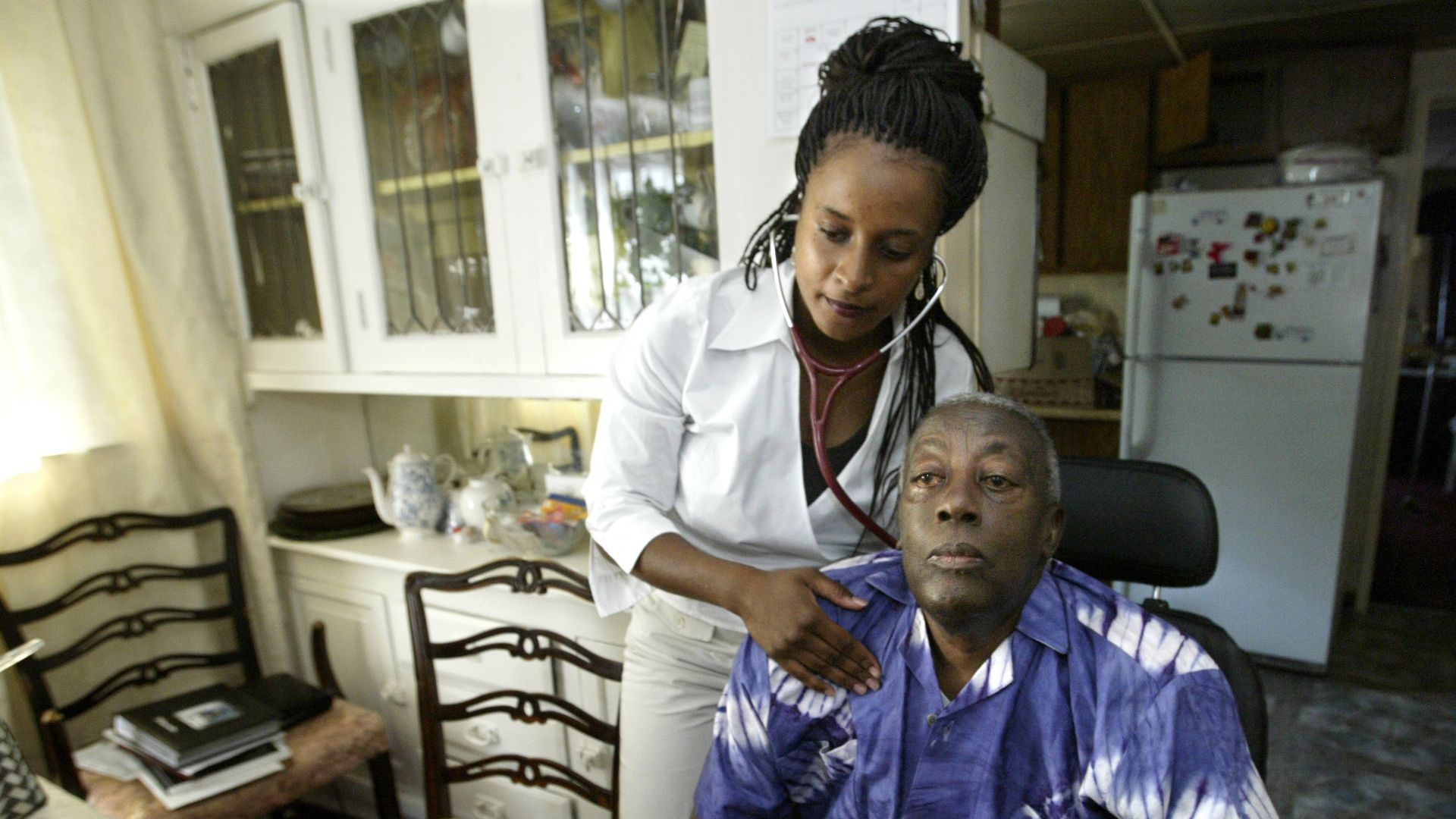
A doctor visits an older adult at his home. Photo: Mel Melcon/Los Angeles Times via Getty Images
The health insurance industry again is attacking federal proposals that would more aggressively audit Medicare Advantage claims for improper coding — audits that would save taxpayers upwards of $4.5 billion over the next decade, Axios' Bob Herman reports.
The big picture: Medicare Advantage is the growth engine of the insurance industry, which has successfully delayed changes and neutered audits.
Between the lines: The audits, called "risk adjustment data validation," have created paranoia among insurers for years. The federal government created the audits as a way to make sure insurers' records of patients' diagnoses matched up to their medical records.
- Medicare Advantage insurers have exaggerated diagnoses as a way to get higher payments from the federal government, costing taxpayers billions of dollars over the past decade.
Driving the news: The Centers for Medicare & Medicaid Services gave the industry until the end of August to send in more comments on a beefed-up auditing process. Insurers still hate everything about it.
- America's Health Insurance Plans, the industry's primary lobbying group, told CMS 8 times in its comment letter to withdraw the entire rule.
- The Blue Cross Blue Shield Association and several regional insurers criticized the idea of removing a formula that adjusted Medicare Advantage overpayments based on errors in the regular Medicare program.
- Centene warned the audits could lead to more "market consolidation."
The Medicare Payment Advisory Commission again stood alone as a supporter of the government's auditing process.
What's next: Federal officials will make a final call on the auditing changes later this year, with the entire industry pressuring them to kill or substantially scale back their changes. It's possible insurers would take this to court if the changes go through.
2. Lung illnesses raise vaping concerns
Most of vaping's negative headlines have been about the rise in teen vaping, but the recent lung illnesses around the country have raised broader questions about its health impact, the New York Times reports.
Driving the news: The Centers for Disease Control and Prevention issued a warning on Friday to teenagers and other consumers, cautioning them against buying bootlegged and street cannabis or e-cigarette products in the wake of the lung illnesses.
The rationale for e-cigarettes is that they're a healthier alternative to cigarettes. But while the health consequences of smoking cigarettes are well-documented, we don't yet know the long-term effect of vaporizing ingredients and then inhaling them.
- We do know, however, that vaping gone awry can be problematic — for example, if oil droplets get inhaled or if toxic substances are vaped.
- "Inhaling oil into your lungs is extremely dangerous behavior that could result in death," Thomas Eissenberg, a professor at Virginia Commonwealth University, told NYT. "That is probably the biggest message we can get out of this."
- Yes, and: The rise of vaping coincides with the spreading legalization of marijuana, which can also be vaped.
The bottom line: "The outbreaks have created a crisis for two emerging industries — e-cigarettes and legal cannabis — that have pitched themselves as beneficial to public health," NYT writes.
3. The disability care funding conundrum
Even as medical advances have both prolonged and enhanced the lives of people with disabilities, the care they need can be prohibitively expensive, the L.A. Times reports.
The Times profiles Sylvia Colt-Lacayo, an 18-year-old with a degenerative neuromuscular disease who received a full ride to Stanford University.
- Her housing and tuition were covered, but she then faced the daunting task of figuring out how to pay for the 18 hours of daily assistance that she'd need in the absence of her mother's care.
The big picture: While federal and state insurance will pay for people with disabilities to live in a nursing home, if they choose to live elsewhere in the community, care is often underfunded.
- "We have an institutional bias in this country," Kelly Buckland, executive director of the National Council on Independent Living, told the Times. "The bias is that if you become disabled or old, you need to go someplace else. You need to go to an institution."
4. Even shoppers can get surprise medical bills
Illustration: Lazaro Gamio/Axios
Plenty of patients don't call ahead to receive estimates of how much their care is going to cost, but even those who do may not receive an accurate quote, as evidenced by Kaiser Health News and NPR's latest Bill of the Month story.
- The patient profiled timed his hernia repair to when it made the most financial sense, and then called his hospital, surgeon and anesthesiologist for price estimates ahead of time.
- The anesthesiologist never called them back, but both the hospital and surgeon's bills ended up being more than double the estimate.
Why it matters: This is an example of, in KHN's words, the "perfect health care consumer," and shows that even the most active patients can easily become victims of the health care system's billing practices.
5. While you were weekending...
- The Washington Post digs into the story of a VA pathologist who misdiagnosed thousands of veterans for years, and how the VA failed to stop him.
- Public health officials' fears are becoming realized in a rural West Virginia county, where there has been a spike in HIV cases related to the opioid epidemic, Politico reports.
- A new study has found that weight-loss surgery can significantly reduce diabetic patients' risk of heart disease and death, Bloomberg writes.
- KHN's Elisabeth Rosenthal details in a column for the NYT why politicians are often loath to criticize hospital costs.
Sign up for Axios Vitals

Healthcare policy and business analysis from Tina Reed, Maya Goldman, and Caitlin Owens.