Axios Vitals

December 14, 2017
Good morning ... With only about 48 hours left in open enrollment, the deadline-driven sign-up surge is well under way — but still unlikely to catch up to last year.
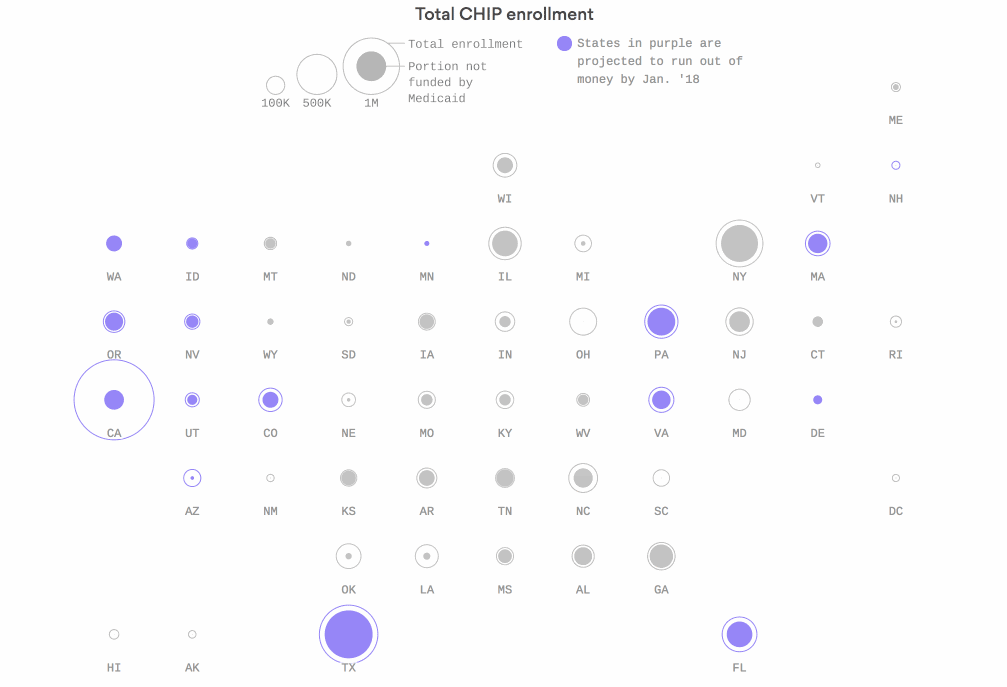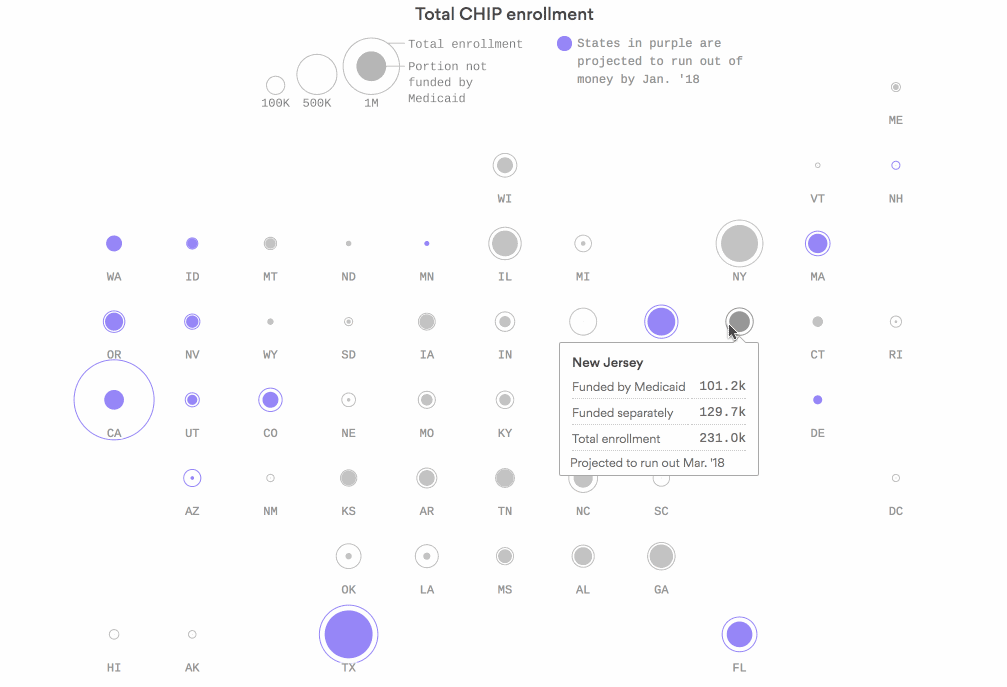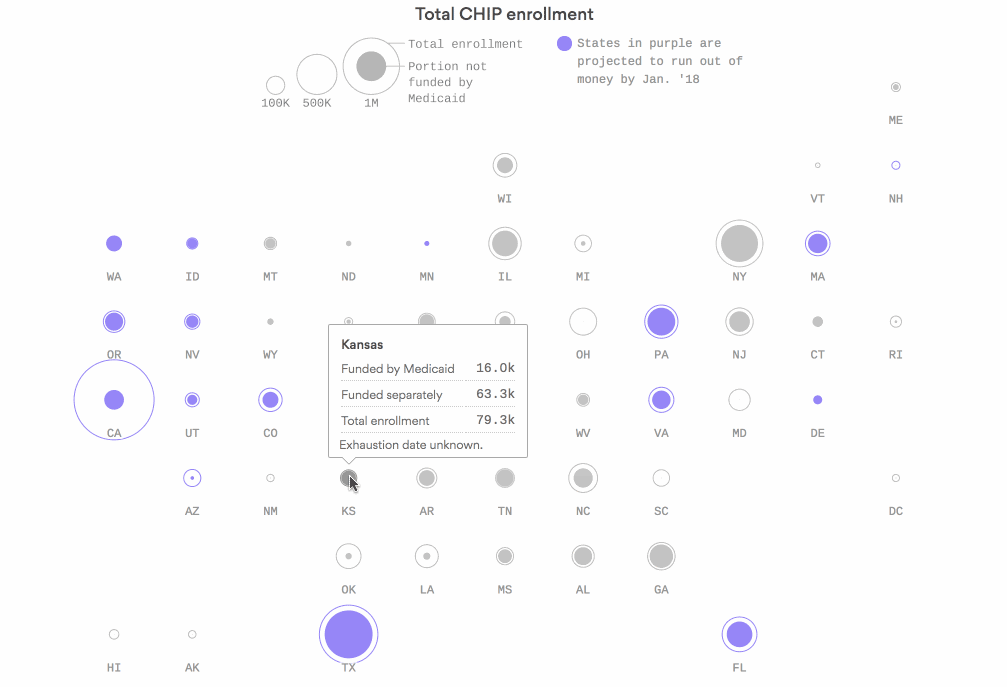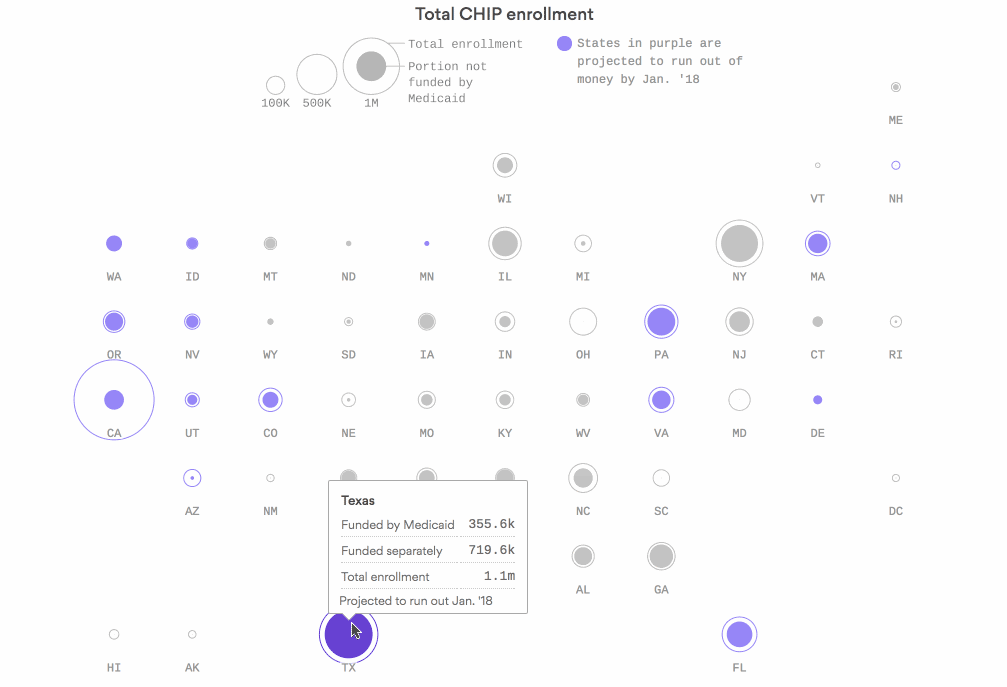
Where CHIP money will start to run out next
Sixteen states are in danger of running out of federal funds for the Children's Health Insurance Program by the end of January if Congress doesn't renew funding — including California, Texas and Florida. In several of those states, very little CHIP coverage is tied to the Affordable Care Act's Medicaid expansion — and those are the kids in the greatest danger of losing their coverage.
Why it matters: The Centers for Medicare & Medicaid Services is tapping into old CHIP funding to help keep states afloat. But it's already about a third of the way through that money, and it'll start to fly out the door even faster as more states — and bigger states — start to need emergency funds.
Go deeper: Check out the interactive graphic.
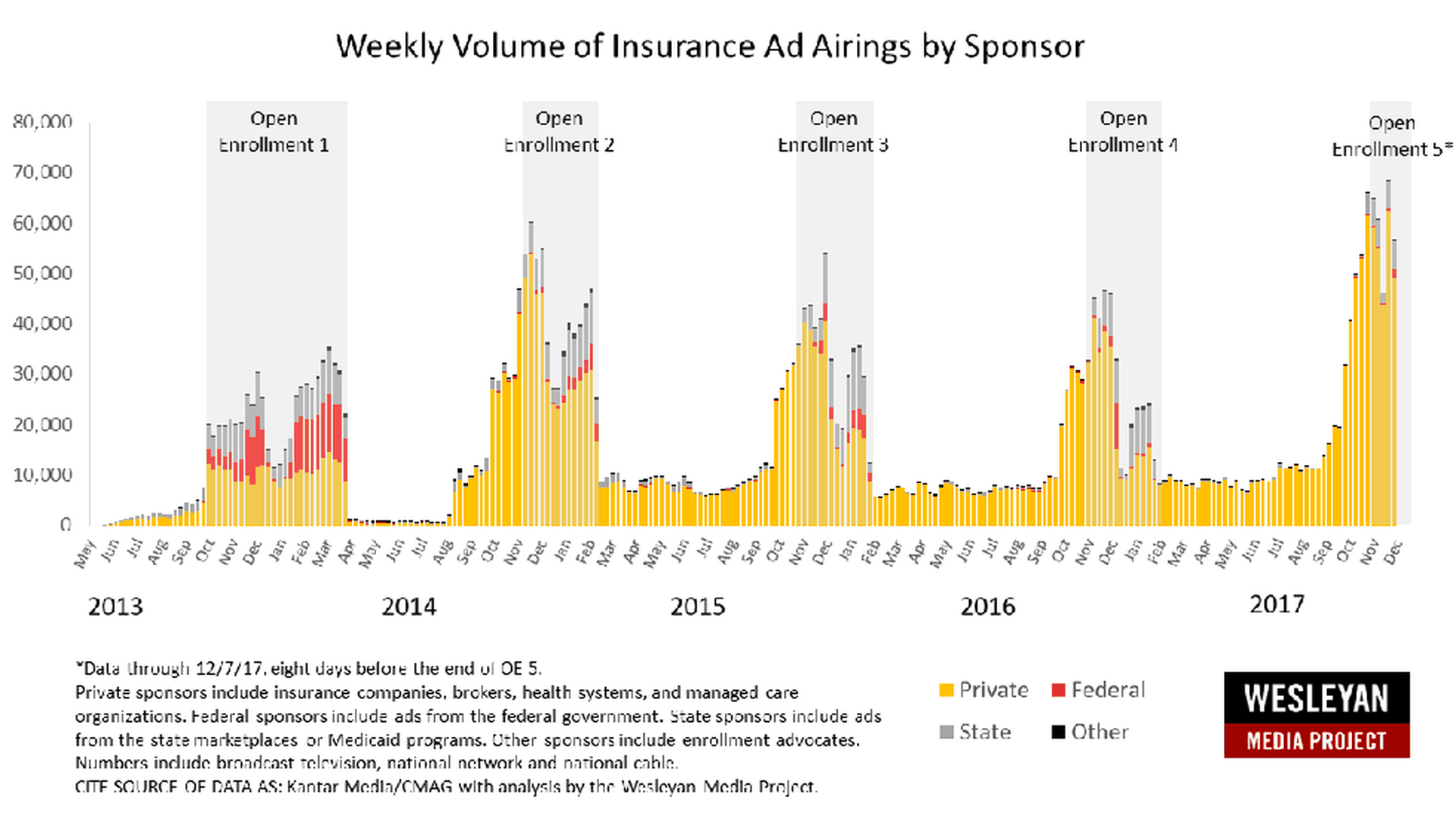
Insurers making up for Trump’s cuts to ACA advertising
Insurance companies have stepped up their advertising for plans sold through HealthCare.gov, and might even be on track to outpace all of the advertising — including government-sponsored promotions — from last year's enrollment period. That's according to new research from Wesleyan University that tracks TV advertising for ACA coverage.
The details:
- Insurers ran a lot more ads during the early part of this year's enrollment window than they have at the beginning of previous years' signup periods. That's not too surprising, since the window is a lot shorter this year.
- Insurers have also stepped up their advertising in the wake of the Trump administration's decision not to run a single TV ad — at least so far — promoting ACA enrollment.
- If the industry's pace continues through the last few days of open enrollment, it could surpass the total number of ads, from all parties, that ran last year.
Yes, but: President Trump also slashed the budget for a different type of outreach — grants that helped community groups and other certified “navigators" reach out personally to the uninsured and assist them in comparing their options.
- The administration says those programs didn't work, returning only a handful of enrollees despite receiving large grants.
- But the Obama administration had consistently said in-person outreach was more effective than advertising.
Equifax hack is creating HealthCare.gov snags
People who froze their credit to try to protect themselves after the massive Equifax hack might have a hard time signing up for health insurance, Kaiser Health News reports.
How it works: HealthCare.gov verifies consumers’ identities using information tied to their credit histories. And people who have blocked access to their credit histories — as many people did in the wake of the Equifax breach — are in some cases finding that HealthCare.gov can’t complete its normal process, and therefore they can’t finish enrolling.
The catch: There are workarounds — you can upload or mail in a set of documents to help establish your identity. A call to another credit agency, Experian, can often clear things up. Consumers can also un-freeze their credit, although the government says it’s not recommending that.
- The problem is that tracking down documents or getting on the phone with Experian can be time-consuming, and is also the sort of hassle people often put off — but a surge of new customers are just now making their way to HealthCare.gov, and the sign-up window closes on Friday.
CMS may ramp up scrutiny of Part D plans
The Centers for Medicare & Medicaid Services might hire a contractor to track whether the companies that sell Medicare prescription drug plans are doing a good enough job, my colleague Bob Herman reports.
Why now: Several Medicare drug plans have been reprimanded for some serious violations, and CMS wants to figure out what's going on.
- CMS barred Arkansas Blue Cross and Blue Shield from enrolling people in its 2018 Part D plans, due to concerns the insurance company was profiting excessively.
- WellCare Health Plans was slapped with a $1.2 million fine earlier this year for a host of Part D violations, including unjustified denials of some members' drugs.
- UnitedHealthcare faced a $2.5 million fine in 2016 after the federal government discovered the insurer's Medicare drug lists were riddled with improper requirements that denied drug access.
Threat level: There's no guarantee CMS will hire a contractor, but the agency is testing the waters to see if an outside company can help determine "whether the Part D formulary and benefit offerings are being administered as approved" by law, according to a document outlining potential responsibilities.
Capitol Hill speed read
House and Senate Republicans have a deal to reconcile their tax bills.
Details of the reconciled tax bill, per the Wall Street Journal:
- The individual mandate: still repealed.
- The deduction for medical expenses: not repealed.
- The plan: vote next week; no waiting for Democratic Senator-elect Doug Jones to be seated.
A new spending bill, tied to Sen. Susan Collins' health care demands, is still in flux.
- The House released a bill last night that would only fund defense programs and CHIP. That's not happening.
- House Freedom Caucus chairman Mark Meadows expects both of Collins' health care demands — funding for the ACA's cost-sharing subsidies and a new reinsurance fund — to be included in the real spending bill, once it's released.
- Collins is under the same impression.
- Meadows says he won't support those provisions, and neither would most of the Freedom Caucus. So Republicans would need Democratic votes in both the House and Senate to avoid a government shutdown. But we kinda knew that was coming.
The Molina era is officially over
Mario Molina has resigned from the board of Molina Healthcare — the health insurance company that his dad started and that he led before getting ousted this past May.
Here's what Molina had to say in a phone call with Bob:
- He was not forced off the board. “I’m very proud of what we accomplished…but now I want to do something different.”
- So what’s next? Running his medical clinics. “And on Thursday I’m going to Disneyland.”
- Molina, who has been critical of Republican health care efforts, also will remain active on Twitter, where he’s advocated for CHIP and ACA enrollment.
What we're watching today: CHIP and the tax bill.
Anything else going on? Let me know about it: [email protected].
Sign up for Axios Vitals

Healthcare policy and business analysis from Tina Reed, Maya Goldman, and Caitlin Owens.