Axios Vitals

February 05, 2019
Good morning ... Situational awareness: Senate Finance Committee Chairman Chuck Grassley has asked 7 pharmaceutical companies — AbbVie, AstraZeneca, Bristol-Myers Squibb, Johnson & Johnson, Merck, Pfizer and Sanofi — to testify at a hearing later this month on drug prices, after the industry didn't send anyone to Finance's last hearing.
Was this email forwarded to you? Sign up here.
1 big thing: Hospitals' prices keep going up
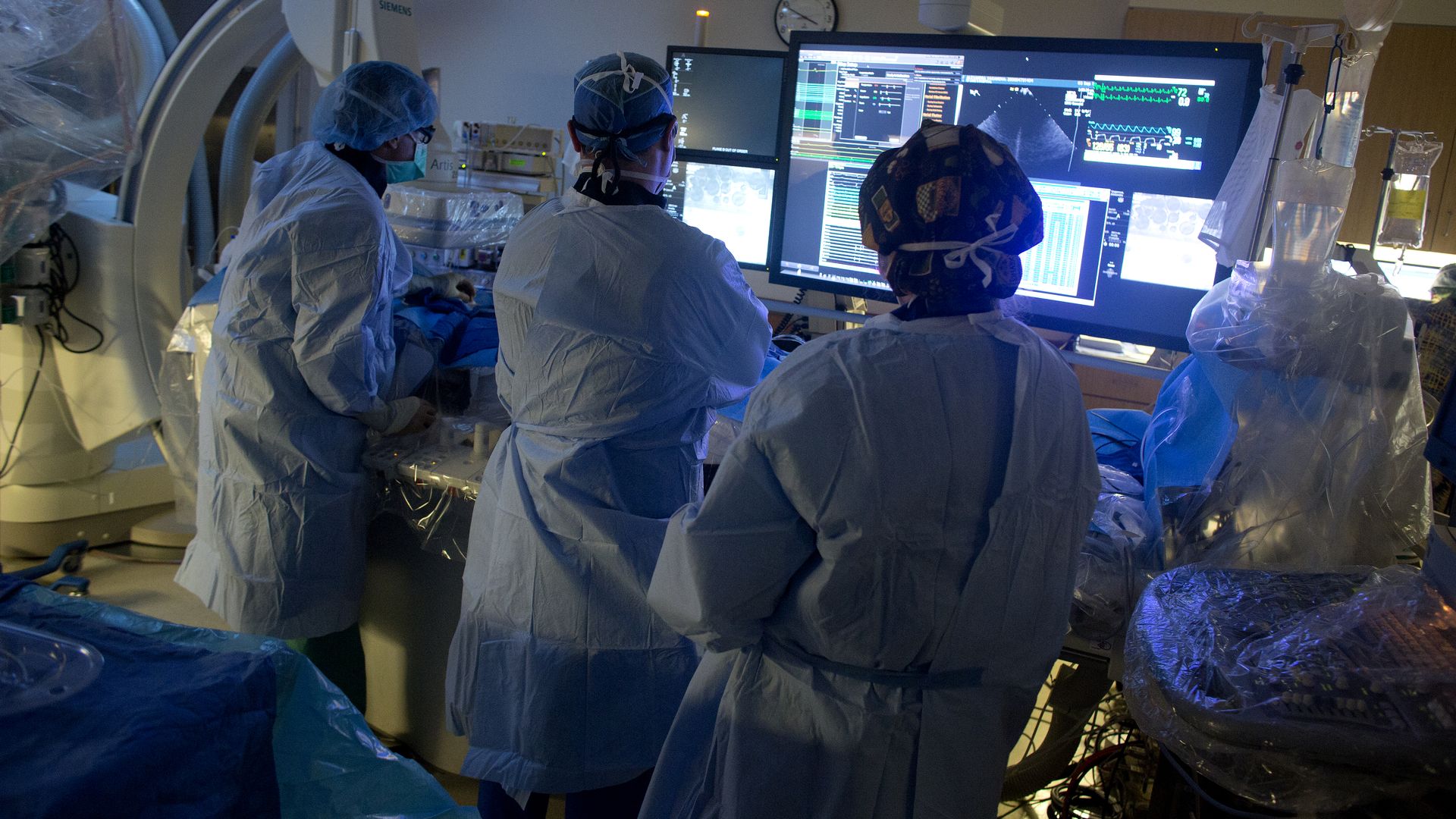
Photo: Andrew Lichtenstein/Corbis via Getty Images
Hospitals are very expensive and they keep getting more expensive, very quickly.
Driving the news: Hospital fees are rising much faster than doctors' fees, and hospitals are driving almost all of the price increases for certain common procedures, according to a new study published in Health Affairs.
Details: The study focused on 4 common procedures, using insurers' claims data to track the real prices patients and insurers paid for those services between 2007 and 2014.
By the numbers: For inpatient care, hospitals' prices rose 42% over that period, compared to 18% for doctors. Hospitals’ fees for outpatient care went up 25%, compared to 6% for doctors.
- About 80% of the total cost goes to the hospital, whether you're in an inpatient or outpatient setting.
- As care has gotten more expensive, hospitals have driven the increase. The total cost of a vaginal delivery, for example, went up by roughly 30% over this 7-year period — and hospitals' fees accounted for almost 90% of that increase.
Prices are also highly variable, even within the same city.
- Now that the federal government is forcing hospitals to post their prices online, Kaiser Health News dug into the data to see what hospitals are charging for the same services.
- For example: What’s the price for a liter of IV fluid? At one Los Angeles hospital, it's $146. At another L.A. hospital just a few miles away, it's $383. At New York Presbyterian, it's $473.
- These are hospitals' sticker prices, not the prices you and your insurance plan would actually pay.
The bottom line: For patients, figuring out what a hospital visit will cost is all but impossible. For economists looking at the system as a whole, the cost of hospital care is a little clearer: It's high, and climbing fast.
Go deeper: Think drug costs are bad? Try hospital prices
2. Pfizer's best-seller isn't what you think


You’ve heard of Lyrica, Lipitor and Viagra. But Pfizer's best-selling drug over the past 4 years isn’t one of its famous names: It's Prevnar 13, a vaccine that protects against pneumonia and other infections.
- And the federal government had a big role in boosting its sales, Axios' Bob Herman reports.
By the numbers: Pfizer has collected $23.4 billion in Prevnar 13 sales since 2015, including $5.8 billion last year.
- The price of a single Prevnar 13 shot this year, before taking out rebates and discounts, is about $195 — a 5% increase from 2018 and 79% higher than its list price from 2010.
Prevnar 13 got a big boost in 2015, after the federal government recommended the vaccine for people older than 65 and required insurance plans to cover it. Before it became so widely used among seniors, it had mostly been prescribed to children younger than 2.
What’s next: The patent for Prevnar 13 doesn't expire until 2026, several years after some of Pfizer's other growing medications, like Ibrance and Xeljanz, will have lost their patent protection.
3. Utah's Medicaid rollback advances
Utah's state Senate passed a measure yesterday to roll back the Medicaid expansion that voters adopted last November, sending the bill on to the state's House, the Salt Lake Tribune reports.
Why it matters: Utah isn't just testing the bounds of overruling a referendum — it's also testing whether the Trump administration will approve a partial expansion. That's never been done before.
- If the administration doesn't grant that waiver, Utah's bill would automatically repeal the entire expansion.
👀 "The only way that we can honor the will of the voters is to ignore the will of the voters," one Republican senator said, according to the Tribune, referring to the costs of the 2 expansions.
- The partial expansion would cost the state much more than the full expansion, but lawmakers say those costs would fall if they get their waiver.
4. Who has employer-based coverage


The number of people getting health insurance through their jobs has been growing over the past few years, as the Kaiser Family Foundation’s Drew Altman wrote last week. And that raises the stakes for Democrats' debate about whether to scrap employer-based coverage.
Between the lines: Those benefits are concentrated mainly among higher-income workers, my colleague Caitlin Owens notes.
- As you move down the income ladder, the number of people with employer-based health insurance falls, even after you account for unemployment.
- Just 28% of full-time workers with an income below the poverty line have employer-based health benefits, according to Kaiser's data. Among workers who make at least four times the poverty limit, that number is 87%.
One big reason: Lower-wage workers are less likely to have the option. Just 33% of the poorest workers have an employer plan available, compared to almost 80% of the wealthiest employees.
Go deeper: How health insurance contributes to income inequality
5. Med schools get a dose of health policy
Health policy is all the rage — in politics, economics and now, increasingly, in medical school.
Why it matters: Policy decisions have a big impact on providers, and med students are pushing for a curriculum that will give them a better grasp of the broader health care system, outside of clinical practice, Bloomberg Law reports.
- "They know that the world is changing around them, but they don't always know what those changes are," Jonathan Oberlander, who chairs the Department of Social Medicine at the University of North Carolina, Chapel Hill, told Bloomberg Law.
Med students' options can include new electives, a 3-week immersion course and even a mock congressional hearing in which students play on the roles of various interest groups to learn "just how difficult the politics are," Oberlander said.
- The organization that accredits graduate programs is also imposing a new rule this year to "incorporate consideration of value, delivery, and payment into their care" into residency programs, per Bloomberg.
Sign up for Axios Vitals

Healthcare policy and business analysis from Tina Reed, Maya Goldman, and Caitlin Owens.