Axios Vitals

September 01, 2017
Happy Friday, and this is it — my last issue of Vitals! But not to worry. I'm passing the torch to Sam Baker next week (after the holiday weekend on Tuesday), and you will be lucky to have him in your inbox every morning because he will make Vitals better, smarter, and faster.
Thanks to all of your for your time and attention, and please encourage all of your friends to sign up as Sam reboots the franchise. I'll start a broader role at Axios next week, so keep in touch and let me know what we can do better: [email protected].
Lessons for the next act on health care
When Congress comes back next week, it's going to start the next chapter on the Affordable Care Act — and it probably will set its sights a lot lower for changing the law, now that the repeal effort has collapsed. There are a lot of lessons Republicans can learn from the failure of that effort — and a few that Democrats can learn too, if they're honest about their own experiences since the ACA became law.
Here are the main lessons for the next round:
Do it step by step. That's how Senate HELP Committee chairman Lamar Alexander says he wants to handle it, starting with a limited bill to stabilize the ACA markets.
Republicans have to decide what they want. Stanford's Lanhee Chen said it became clear during the repeal debate just how deeply divided conservatives are on health care policy — and that will continue to be an issue during the next steps.
The details matter. It wasn't just John McCain who said a big health care bill should go through hearings. Lisa Murkowski said her "no" vote was meant as a warning that "We're not ready to go to the floor to wrap this up," as the Alaska Dispatch News reported at the time.
If one party owns it, it doesn't last. This is a lesson for both parties. When Democrats passed the ACA on their own, it was only safe as long as a Democrat was in the White House. If Republicans rewrote the health care system by themselves, they would have been taking the same risk. (So, Democrats — single payer? Really?)
Ditch the talking points. Former Senate GOP aide Rodney Whitlock said the Alexander-Murray hearings could help by forcing Republicans to face the need for the risk sharing protections. They could also force Democrats to figure out what they're actually willing to do to improve the ACA.
Don't overpromise. Funny thing about both the repeal debate and the original ACA debate — they both promised lots of winners and no losers. That doesn't happen in health care. As Whitlock put it: "In health care, there's no such thing as a free lunch."
You can change the ACA, but you're not going to get rid of it. Unless Senate Republicans find that 50th vote — and there's no sign that they're anywhere close — the next chapter is going to be about putting a more conservative stamp on it. Turns out John Boehner was right.
How Alexander and Murray will get senators on board
We all thought Caitlin Owens was on vacation this week, but her sources didn’t know that! Per Caitlin, Alexander and Murray are planning to invite senators who aren’t on the HELP Committee to meet with the witnesses before each hearing. There’s one round of hearings on their stabilization effort next week, and another round the following week.
Between the lines: It could be a good way to increase the buy-in from Republicans and Democrats before Alexander and Murray introduce their bill — if it helps convince them what needs to be done to end the turmoil.
About those HHS advertising cuts...
The Department of Health and Human Services blew up a quiet health care week yesterday with its announcement that it's going to cut the ACA advertising budget by 90% for next year.
Why the cuts? HHS officials say they're trying to be cost-conscious — because ACA enrollment this year actually fell despite $100 million in advertising.
Normally, with this kind of debate about cost effectiveness, you get a healthy debate from both sides. But it was pretty one-sided yesterday.
- There were plenty of Democrats and other ACA supporters blasting the Trump administration for “sabotage."
- But if you were looking for the “Thanks for being fiscally responsible, HHS" messages, you wouldn't have found much — other than House Energy and Commerce Republicans cheering a separate set of cuts to “navigators" who help sign people up.
Why it matters: The consensus from pro-ACA health care experts is that cutting the advertising budget will only drive up premiums — because healthy people won't sign up.
- “Not smart," tweeted Venrock's Bob Kocher, a former Obama administration health care adviser.
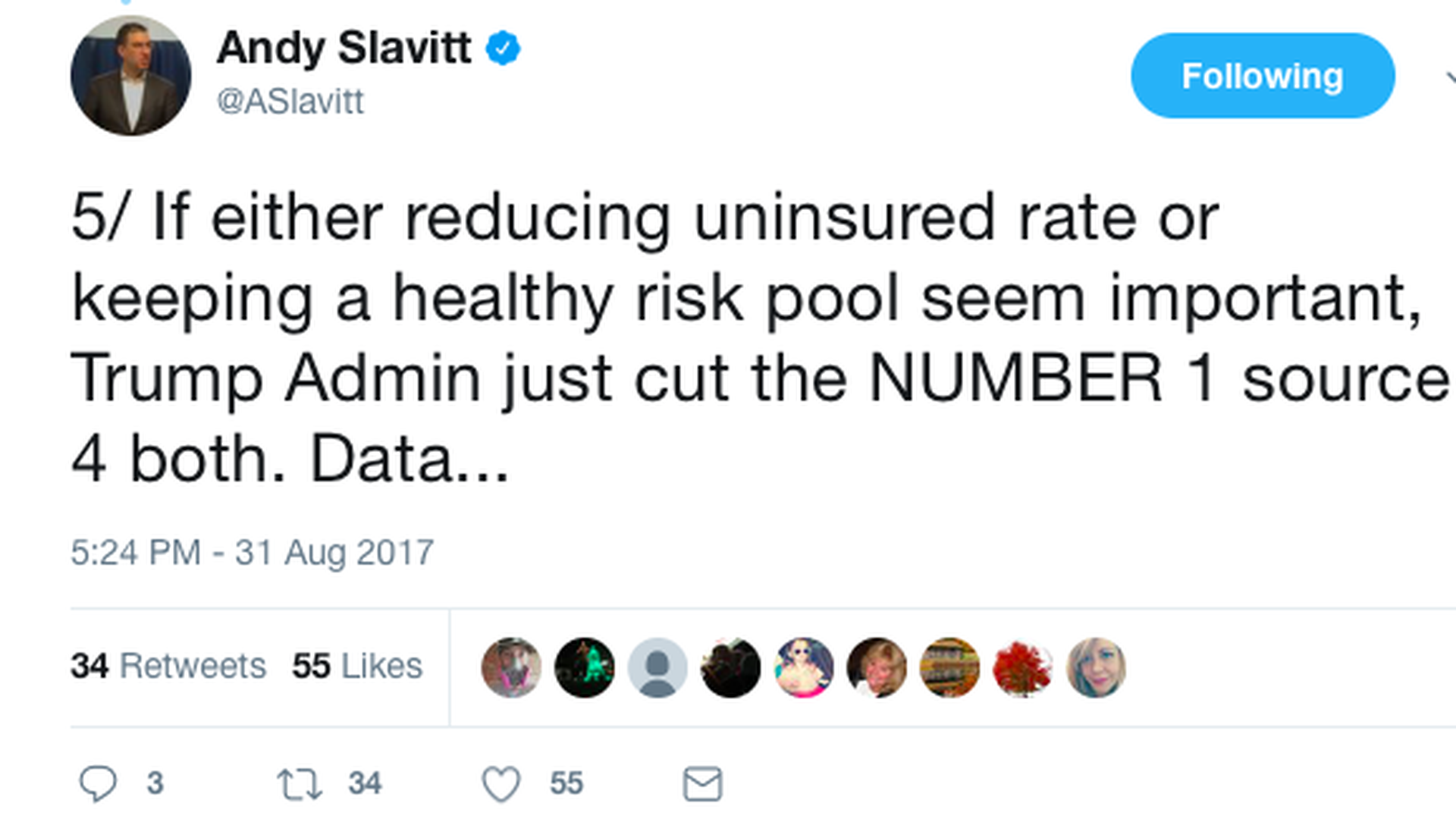
- Andy Slavitt, who ran the Centers for Medicare and Medicaid Services under former President Obama, says a 90% cut in ad spending means a "dramatic cut" to ACA enrollment next year — “which means a worsening risk pool, higher government outlays, less competition, and higher premiums paid by American families."
The bottom line: The Trump administration insists its actions are about cost-effectiveness. "Judging effectiveness by the amount of money spent and not the results achieved is irresponsible and unhelpful to the American people," said HHS spokeswoman Caitlin Oakley. If so, the silence from budget hawks is deafening.
The looming Tar Heel health care giant
ICYMI yesterday, Bob Herman reported that UNC Health Care and Carolinas HealthCare System — two rather profitable not-for-profit health systems based in North Carolina — want to merge. The combined public system would be bigger from a revenue standpoint than other major medical system giants like Partners HealthCare in Boston or Dignity Health along the West Coast.
Here's what Bob advises us to watch next:
The impact: If the systems are able to merge, layoffs appear inevitable. (“Restructuring would be required," according to an internal memo from UNC CEO William Roper). But more broadly, it would become a lot more difficult for a health insurance company to exclude the UNC-Carolinas system from networks, given its size and affiliation with a cutting-edge medical school.The rationale: Roper and Carolinas CEO Gene Woods spoke with reporters yesterday. They naturally said the deal wasn't about reducing competition and trotted out the line of "advancing care." In particular, they want to find ways to improve care in rural areas, which North Carolina has struggled with.The big question: How will antitrust wonks at the Federal Trade Commission respond? Carolinas and UNC mostly operate in different parts of North Carolina, but they command a lot of inpatient market power in their respective areas. (The Justice Department is already suing Carolinas for allegedly stiffing competitors.)The bottom line: Despite what Roper and Woods say, they are indeed reducing competition. The systems did not immediately respond to whether they did any antitrust planning.Looking ahead: Mergers beget mergers. Other health systems in North Carolina like Novant Health and Duke University Health System are looking smaller right now.Don't forget: Catholic Health Initiatives and Dignity Health are still evaluating their own megamerger.
The Kasich-Hickenlooper tradeoff
If you look at the health care plan Ohio Gov. John Kasich and Colorado Gov. John Hickenlooper released yesterday, you might have trouble finding a lot for Republicans to like — other than a few state flexibility options, like letting states combine waivers and adapt ones that have been approved in other states.
Yes, but: Greg Moody, director of Ohio's Office of Health Transformation, tells me the other steps the plan would take to stabilize the markets — like funding the ACA's cost-sharing reduction payments and reinsurance programs to help limit insurers' losses — would make it easier for states to pursue the waivers. That's because it's easier for them to try some of the obvious reforms, like alternatives to the individual mandate if the markets are stable.
Key quote: “The federal government's responsibility is to create stability in the markets in the short term. That then clears the path for states to take action."
Medigap changes are coming
Turns out that HHS was doing other things yesterday too, and Bob was paying attention. It put out a notice reminding everyone big changes are in store for Medicare supplemental insurance policies, known as Medigap plans. Roughly 12.6 million people have a Medigap plan to help fill in the coverage holes in the traditional Medicare program.
What's changing: Any Medigap policy that covers the annual Medicare Part B deductible ($183 this year) will be eliminated starting Jan. 1, 2020, and will not be available for new Medicare enrollees. Those plans are the most popular.
Why: It's required by the payment law MACRA. Although nearly all of that law is about changing how Medicare pays physicians, one tiny section forbids the sale of any Medigap plan that covers that Part B deductible. The goal is to give seniors more "skin in the game."
Ripple effect: Eliminating these types of Medigap policies could push seniors to choose Medicare Advantage plans instead, perhaps without understanding the tradeoffs.
What we're watching next week: Senate HELP Committee hearings on bipartisan ACA stabilization bill, Sept. 6 (insurance commissioners) and Sept. 7 (governors). 2017 Wells Fargo Healthcare Conference in Boston, Sept. 6-7; Senate Finance Committee hearing on CHIP reauthorization, Sept. 7; markup of Senate funding bill for HHS, dates TBD.
Also, Kasich and Hickenlooper discuss their ACA proposal at a joint American Enterprise Institute-Center for American Progress event, Sept. 8. RSVP here.
What we're watching in two weeks: Senate HELP Committee hearings on bipartisan ACA stabilization bill, Sept. 12 and 14. Also, Healthcare Security Forum, sponsored by the Healthcare Information and Management Systems Society, Sept. 11-13.
Sign up for Axios Vitals

Healthcare policy and business analysis from Tina Reed, Maya Goldman, and Caitlin Owens.