Axios Future of Health Care

October 17, 2025
Good morning, and welcome back. We're mixing things up and tapping into one of the original key themes of this newsletter and a big driver of the week's news: health insurance.
- We're also on top of the latest headlines and unpacking the White House's IVF drug pricing deal.
1 big thing: Unsubsidized health insurance is unaffordable
Something big is being missed in the congressional showdown over enhanced Affordable Care Act subsidies: Health insurance premiums are eye-wateringly expensive for the average person without some kind of subsidy.
Why it matters: Health care in the U.S. is expensive, we know, we've all heard it a million times. But most of us don't really feel its full expense, which removes a lot of the urgency to truly address health care costs.
- Whether it's through government tax credits or employer premium assistance, most Americans with private health insurance don't pay the entirety of their premium.
- But we're all paying the freight one way or another, either through taxes or paycheck deductions.
State of play: The past few weeks have been full of dire warnings from Democrats and their allies about what will happen if the enhanced ACA subsidies from the pandemic era are allowed to expire at year's end.
- The gist is that millions of Americans will have sticker shock when they're exposed to more or all of the premium cost, and many will ultimately opt out of buying coverage. That's all probably true.
- Of course, allowing the enhanced subsidies to expire would just make the law's structure revert to its original state.
- And that's why some savvy Republican-aligned commenters are asking if that means the ACA is broken, or if the original version was unworkable.
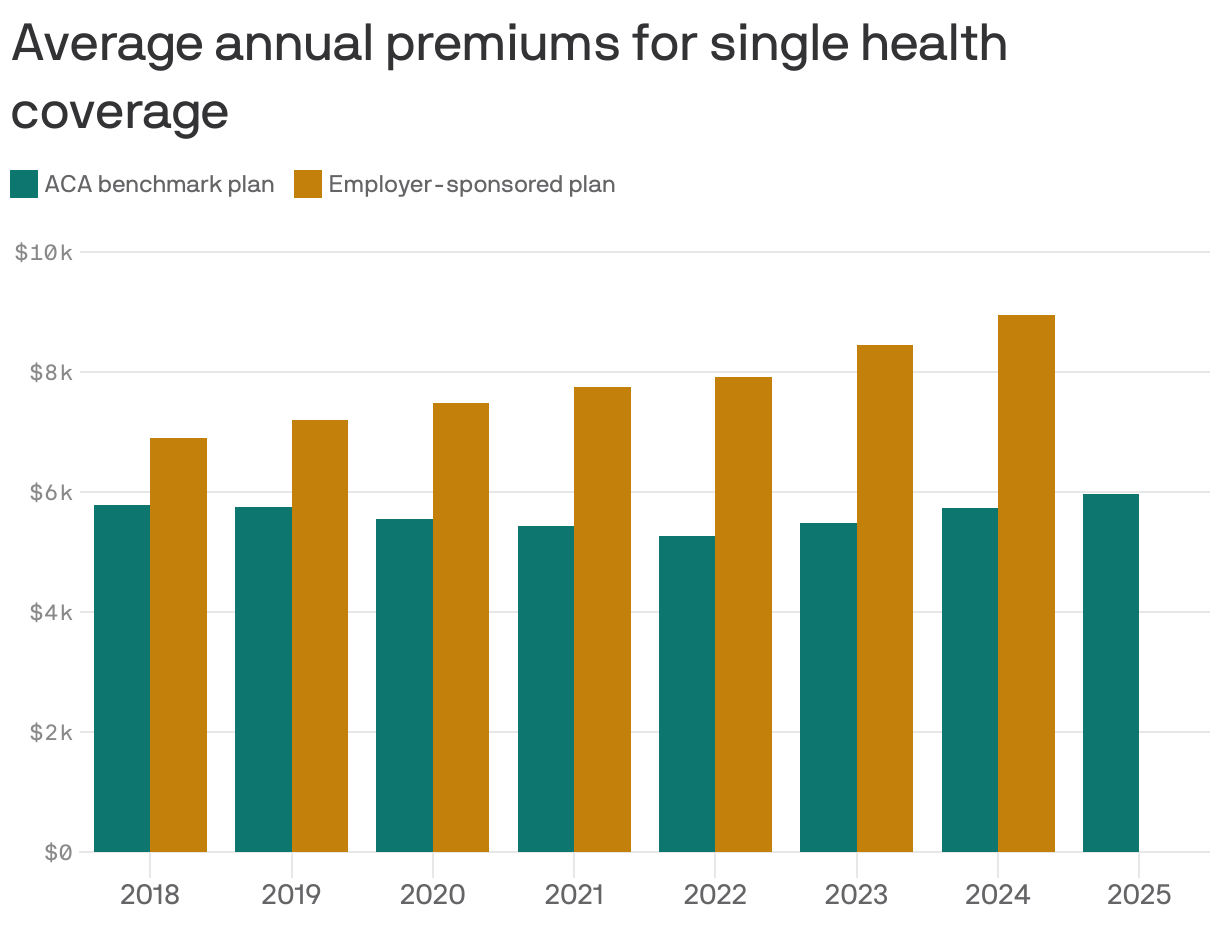
Reality check: Premiums have gone up — a lot, in some cases. But that's not unique to the ACA marketplace, and premiums are even pricier in the employer market.
By the numbers: This year, the average premium for a benchmark ACA plan is $497 a month, or nearly $6,000 a year, according to KFF.
- The average employer-employee premium for single coverage was $8,951 last year, also according to KFF.
- The average premium for family coverage was a whopping $25,572.
Let's do some math. Without any form of subsidization, a single person making $60,000 would spend 10% of pretax income on an ACA plan, and 15% on an employer plan.
- Now let's say that $60,000 income is supporting a family of four. The average premium without subsidies would cost that family 43% of its pretax income.
- The median U.S. family income, according to the Census Bureau, was $83,730 in 2024. Health insurance premiums would be 31% of pretax income.
Between the lines: The definition of "affordable" is obviously very subjective, but it seems safe to say that some of these numbers — especially for families — aren't meeting it.
What we're watching: Open enrollment is coming, and people with ACA coverage aren't the only ones facing premium increases.
- Health benefit costs are expected to increase 6.5% per employee in 2026, according to Mercer. Many employers are planning to limit premium increases by raising out-of-pocket costs for employees.
- On average, ACA marketplace plans are raising premiums about 20% in 2026, according to KFF.
- How much of that increase gets passed on to enrollees will depend on whether the enhanced subsidies are extended, but the premium increases are partially due to insurers having accounted for the subsidy expiration.
The bottom line: Policymakers have two broad options: They can keep fighting over who pays for what, or they can do bigger, systemwide reform.
- If you're waiting for the latter, don't hold your breath!
2. Why this drug deal is different
The drug pricing deal announced yesterday between the White House and EMD Serono followed the same contours as recent Pfizer and AstraZeneca deals.
- But the way that it involves drugs used in in vitro fertilization may have more direct implications for patients.
Between the lines: IVF often isn't covered by insurance, so many Americans pay out of pocket. That means they don't get discounts negotiated by intermediaries on IVF drugs.
- Last year, just over a quarter of large firms offering health benefits covered IVF services, according to KFF (the same survey used in the above item!).
For people who would otherwise pay list prices, buying the drugs at a heavy discount on TrumpRx could generate meaningful savings.
- It's less clear who stands to benefit from buying other drugs commonly covered by insurance via the new platform, which goes live in January.
By the numbers: The drugs offered by EMD Serono on TrumpRx will include three therapies that, when all used during a course of IVF, will be offered at an 84% discount off list prices, according to the company.
- About half of patients who currently take the fertility drugs pay fully out of pocket for them, said Libby Horne, head of EMD Serono's fertility practice.
- And even patients with insurance coverage of IVF often have annual or lifetime benefit maximums, which can get depleted by IVF services, she added.
- "Patients today may be paying the list price or accessing self-pay prices … but these [TrumpRx] prices represent a significant discount versus both of those," Horne told me.
Yes, but: The cost of IVF is driven by more than just drugs.
- The average cost of one IVF cycle in the U.S. is $21,600, according to Carrot, and people often require more than one round. Medications and injections cost from $3,000 to $7,000.
- "There are many parts to IVF and fertility treatment that go far beyond the cost of the actual drugs," said Alina Salganicoff, director of the Women's Health Policy Program at KFF.
Thanks to Adriel Bettelheim and David Nather for editing and Brad Bonhall for copy editing.
Sign up for Axios Future of Health Care


