Axios Future of Health Care

August 16, 2024
Good morning, we're leading with the obvious this week: Medicare's negotiated drug prices. Let's get to it!
Today's word count is 1,117, or a 4-minute read.
1 big thing: Analysts shrug
Unless you were under a rock, you saw yesterday's news that Medicare negotiated a better deal than the private market for some of the program's top-selling drugs.
Why it matters: So what? How meaningful is that difference, and what will the longer-term effects be?
- Some seniors will likely pay less out of pocket for drugs (that's a whole topic that we're not going to get into right now), and that obviously matters to patients. But how pharma interprets the negotiated prices and reacts to them will have a huge impact on future drug development.
Our thought bubble: Democrats are thrilled, Republicans are appalled. The drug industry is complaining publicly but telling investors everything is fine.
- For all of the uproar this law caused when it was passed, the financial world's reaction to today's rollout made everything seem pretty good — for now (more on that below).
Between the lines: The announced prices — an overall 22% reduction in net spending but no details on individual drugs' net price reductions — are less drastic than some feared.
- "There are strong price reductions, but it also shows there is plenty of room for the industry to continue to make some profits on these drugs," Vanderbilt's Stacie Dusetzina said.
Analysts are reacting much more neutrally than the politicians.
- In a note titled "CMS Spins, Pharma Wins (Relatively)," Raymond James analyst Chris Meekins wrote that "the impact is far less than politicians proclaimed and the industry as a whole seems to be managing this fine so far."
- And in a note titled "Sigh of Relief," Leerink analysts concluded that "22% is not as bad as anticipated earlier this year," though recent earnings calls had assuaged fears somewhat.
Where it stands: No one knows for sure the net prices of Part D drugs, much less what they would have otherwise been in 2026. But there are some estimates, and Medicare's negotiated rate is generally lower than those estimates.
- Here's a comparison from American Enterprise Institute economist Ben Ippolito, using data from this study.
The big picture: If there's anything everyone agrees on, it's that America's high drug prices make up a grossly disproportionate bulk of pharma's revenue compared with the rest of the world's.
- Critics — which include many politicians from both parties! — say all that means is that America is getting ripped off.
- Pharmaceutical companies and some experts say that this subsidization allows drug companies to keep searching for and investing in new therapies despite too-low prices in other countries.
Regardless, that tasked the administration with figuring out how much of a revenue haircut — or a subsidy reduction — drug companies could take without sacrificing the new drugs we want them to continue bringing to market.
- So far, that haircut seems to be pretty manageable.
- "We've shown that it can be done successfully and the sky doesn't fall," said Harvard's Aaron Kesselheim. "It's not surprising to me that the markets haven't come crashing down, because I think this process was not set up to bankrupt the pharmaceutical industry."
2. Why this may not be a good crystal ball
There are several reasons why the outcome of negotiations over this particular group of drugs may not say much about future outcomes.
- Many of them were already about to get generic competition, which may not be the case for drugs selected down the road. Most of them are already highly rebated.
- And the number of drugs any given company is receiving a negotiated price for will likely go up over time, as more drugs enter the program each year.
- "The financial impact will be a lot worse when companies have many drugs negotiated rather than just one or two in '26 that are going off patent anyway," said Leerink's David Risinger.
Plus, positive earnings calls may not reflect the full picture.
- "Over time, will they adjust and make money? Big pharma — of course. It's small pharma … that's getting severely impacted," said Joe Grogan, the former director of the United States Domestic Policy Council in the Trump administration.
- "They're figuring out how to continue to make money, but it doesn't alter the fact that it upset their R&D expenditures and their R&D plans, and it's going to leave fewer therapies and fewer treatments down the road," he added.
- "Medicine development is a long and complex process, and the negative implications of these changes will not be fully realized for decades to come," said PhRMA CEO Steve Ubl in a statement before the rates were released.
And perhaps the biggest wild card of all: Different administrations could take different approaches — and nothing requires any given administration to be consistent.
- "They have flexibility to negotiate harder in coming years, and maybe they didn't want to poke pharma in the eye too hard in the first year," Risinger said.
- "The problem is it's unpredictable so it's hard to forecast," former FDA commissioner Scott Gottlieb told me. "These will ultimately be political decisions, and as much as CMS says there's a process and a formula, there isn't."
The bottom line: For now, it looks like the Biden administration found a way to save the government some money — it helped me to consider how I'd think about a 22% sale in my personal life — without really upsetting the drug market.
- That balance may not be reproduced going forward.
3. Anti-obesity drug coverage price tag
Speaking of Medicare spending — if you are paying any attention at all, you know that there's a huge debate over whether Medicare should cover anti-obesity drugs.
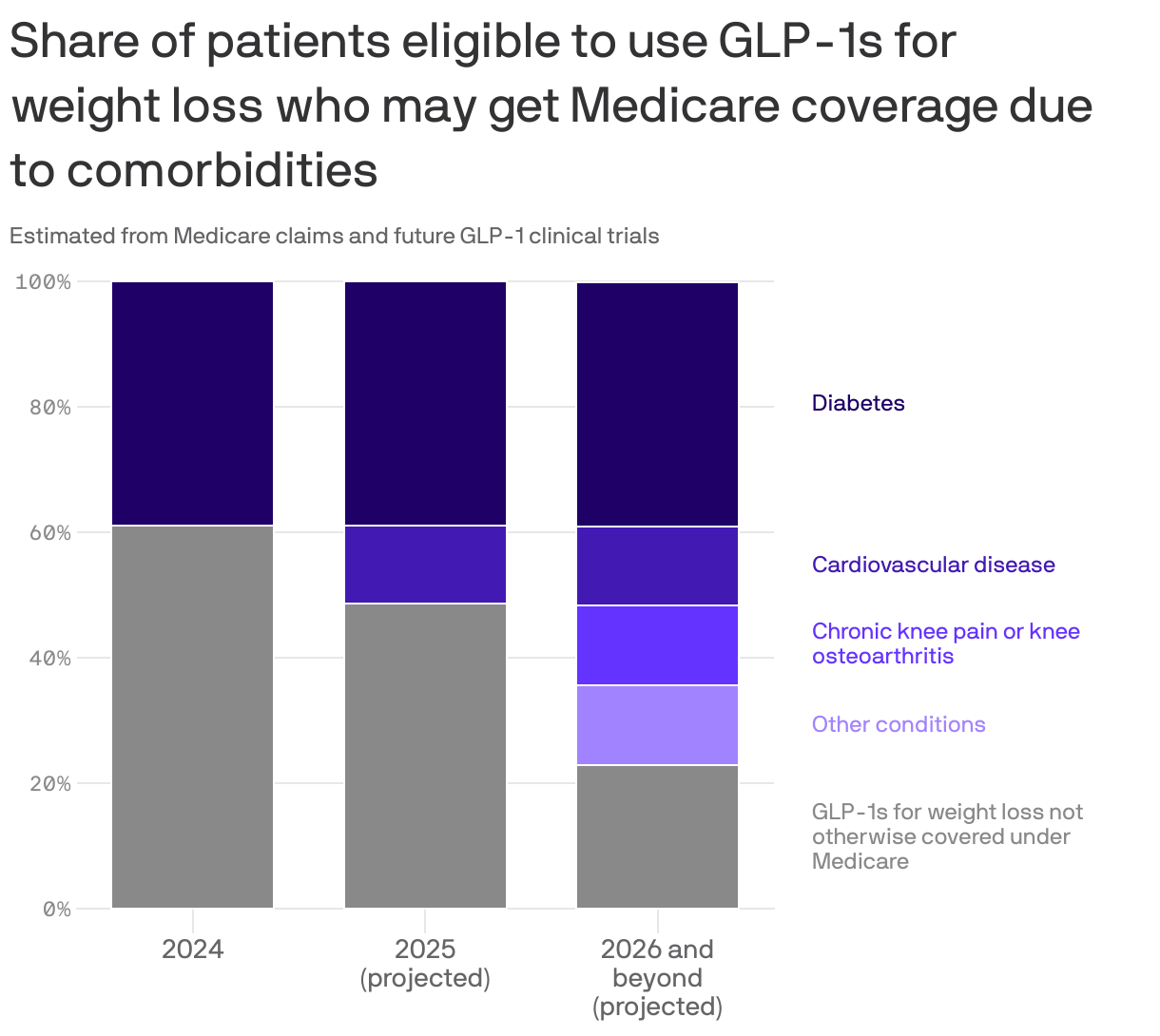
Driving the news: A newly published study in Health Affairs not only gives an estimate for how much such coverage would cost taxpayers, but also illustrates how this may be an overblown debate given all of the other conditions GLP-1s may soon be approved for.
- Medicare already covers them as diabetes treatments, for example. If it also turns out they are effective against knee pain, Medicare would have to cover them for that use in the next few years — it's just weight loss it doesn't cover.
- And millions of patients who'd qualify to use GLP-1s for weight loss have these other conditions that may soon make them eligible for coverage anyway.
By the numbers: The study estimates Medicare coverage, if it started in 2025, to increase spending by $3.1-$6.1. billion a year.
- A very important variable: Those numbers assume only 5%-10% of the newly eligible patient population are prescribed a GLP-1 for weight loss.
The intrigue: Just to go full circle here, semaglutide — the active ingredient in Wegovy and Ozempic — is expected to be eligible for Medicare negotiations as soon as next year, which would mean a 2027 price implementation date.
- That makes estimating how much weight loss coverage would cost even more complicated.
Thanks to Nicholas Johnston and Adriel Bettelheim for editing and Matt Piper for copy editing.
Sign up for Axios Future of Health Care


