Axios Cleveland

November 11, 2024
Good morning, Monday!
🇺🇸 This Veterans Day we're honoring those who have served by focusing this special newsletter on them.
- If you are a veteran, here's where to find a free meal or deal.
Your local team is off today but will return to your inbox tomorrow.
Today's newsletter is 871 words — a 3-minute read.
1 big thing: Psychedelics offer hope for PTSD
Veterans are campaigning to take psychedelic therapy for post-traumatic stress disorder mainstream, despite the Food and Drug Administration's rejection of an ecstasy-based therapy in August.
Why it matters: About 29% of veterans who fought in Afghanistan and Iraq will have PTSD at some point in their lives, according to the Department of Veterans Affairs. Veteran suicide rates are also higher than in the general population.
- "The thirst is very palpable among our generation" of veterans for alternative mental health therapies, Allison Jaslow, CEO of Iraq and Afghanistan Veterans of America, told Axios.
Catch up quick: Psychedelics like magic mushrooms, LSD and ecstasy can alter a person's state of mind and cause hallucinations.
- It's been nearly impossible to research their effects, because they've been criminalized and classified as controlled substances since 1970.
- But interest in psychedelics' potential to treat mental health conditions — particularly in veterans — has grown in recent years.
- The FDA in 2017 granted fast-track review of a PTSD treatment that mixes ecstasy with talk therapy.
The VA started funding research into psychedelic therapies this year. Congress also passed bipartisan legislation directing the Pentagon to study the treatments.
- In the meantime, more than 1,200 veterans traveled to other countries for psychedelic therapies through one nonprofit alone, said Jesse Gould, founder of that organization, Heroic Hearts Project.
But the FDA in August rejected the therapy it had originally fast-tracked, following an independent review that highlighted concerns like missing safety data and allegations of misconduct in clinical trials.
Zoom in: The decision felt like a major setback to veterans.
- "It was emotionally just gut-wrenching, thinking about all of those veterans, and all the other people, for that matter, that were just really counting on being able to access this as a solution for their debilitating PTSD," said Juliana Mercer, a Marine Corps veteran and director at veterans advocacy group Healing Breakthrough.
- The FDA rejection pushes mental health progress back years, added Gould, a former Army Ranger. It "indicates to veterans that they are not being listened to and they're not a priority."
Where it stands: Veterans are continuing to work toward broadening access to psychedelic therapies.
- State-level action is also picking up. Oregon and Colorado have legalized psychedelic mushrooms for therapeutic use. But Massachusetts voters last week rejected a ballot proposal to legalize psychedelics.
Read about what's next for psychedelic therapies, and a potential "silver lining"
2. Care Program lacks care
A federal program serving 2.8 million veterans isn't delivering on key promises.
The big picture: The Veterans Community Care Program was set up to help veterans secure appointments with providers near their homes when they can't receive care from a Department of Veterans Affairs facility.
- It has been touted as an important safety net as demand for mental health care grows.
But the cost of the referrals has been rising, reaching nearly $30 billion in fiscal 2023. And since its establishment in 2019, the program aimed at bypassing long wait times has instead exacerbated them, at a higher cost to taxpayers, per reports.
Veterans are waiting more than two weeks on average from the time a referral is made to even schedule an appointment through the community care program, according to audits by the Government Accountability Office. They're supposed to have mental health appointments within 30 days.
- An examination of fiscal 2022 data showed that VA appointments were scheduled on time more often than community care.
Driving the news: Federal audits over the past two years found veterans aren't getting timely mental health care, services like diagnostic testing, or consultations with cardiologists and other specialists.
- Lawmakers in Congress highlighted instances in which veterans were cut off from cancer treatments in their hometowns or lost access to non-narcotic painkillers, leaving them with few options besides opioids.
- Also, the VA slowed health care hiring this year, Government Executive reported.
Friction point: A report by independent experts last spring detailed a budget squeeze, in which rising costs connected with community care will decrease available funds for the VA's own in-house direct care system.
- Without more funding, the report raised the prospect of VA service cutbacks.
What's next: VA officials say they still want to expand staffing in areas like mental health, cardiology and gastroenterology, raising questions about whether there will be cuts elsewhere.
3. 1 chart to go: Where our veterans are
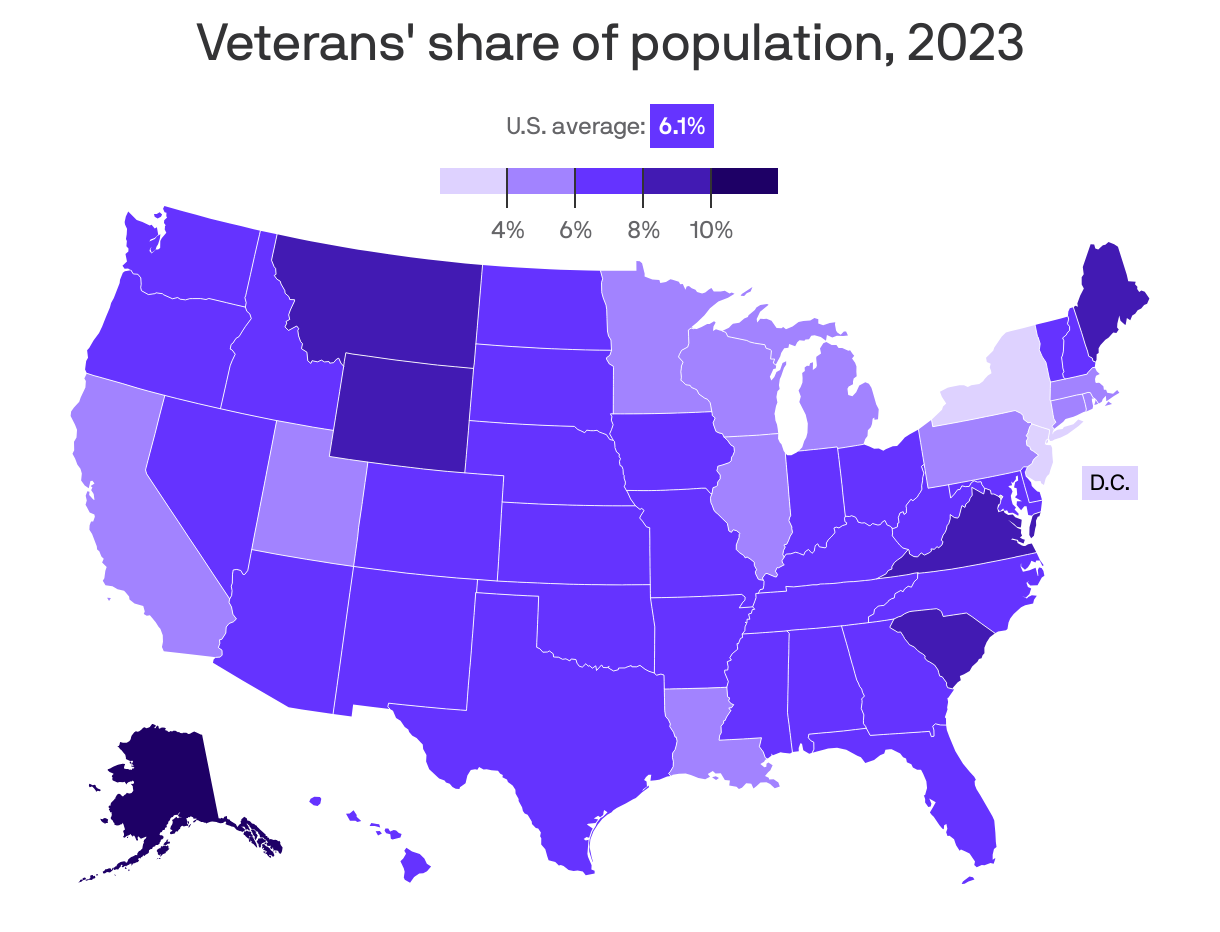
Veterans make up the greatest share of the population in Alaska (10.5%), Virginia (9.1%) and Montana (8.9%), per the latest census data.
- They make up the lowest shares in D.C. (3.2%); New York (3.6%) and New Jersey (3.6%).
How it works: That's among civilians over 18, and according to the 2023 American Community Survey.
The big picture: Veterans make up about 6.1% of the U.S. population overall.
Want more newsletters like this? Keep up with health care politics, policy and business by subscribing to Axios Vitals.
A special thank you to health care policy reporter Maya Goldman and senior health care editor Adriel Bettelheim for making this newsletter possible.
Sign up for Axios Cleveland





