Updated May 31, 2018 - Health
Aetna, doctors battle in court over sick infants' care
Add Axios as your preferred source to
see more of our stories on Google.
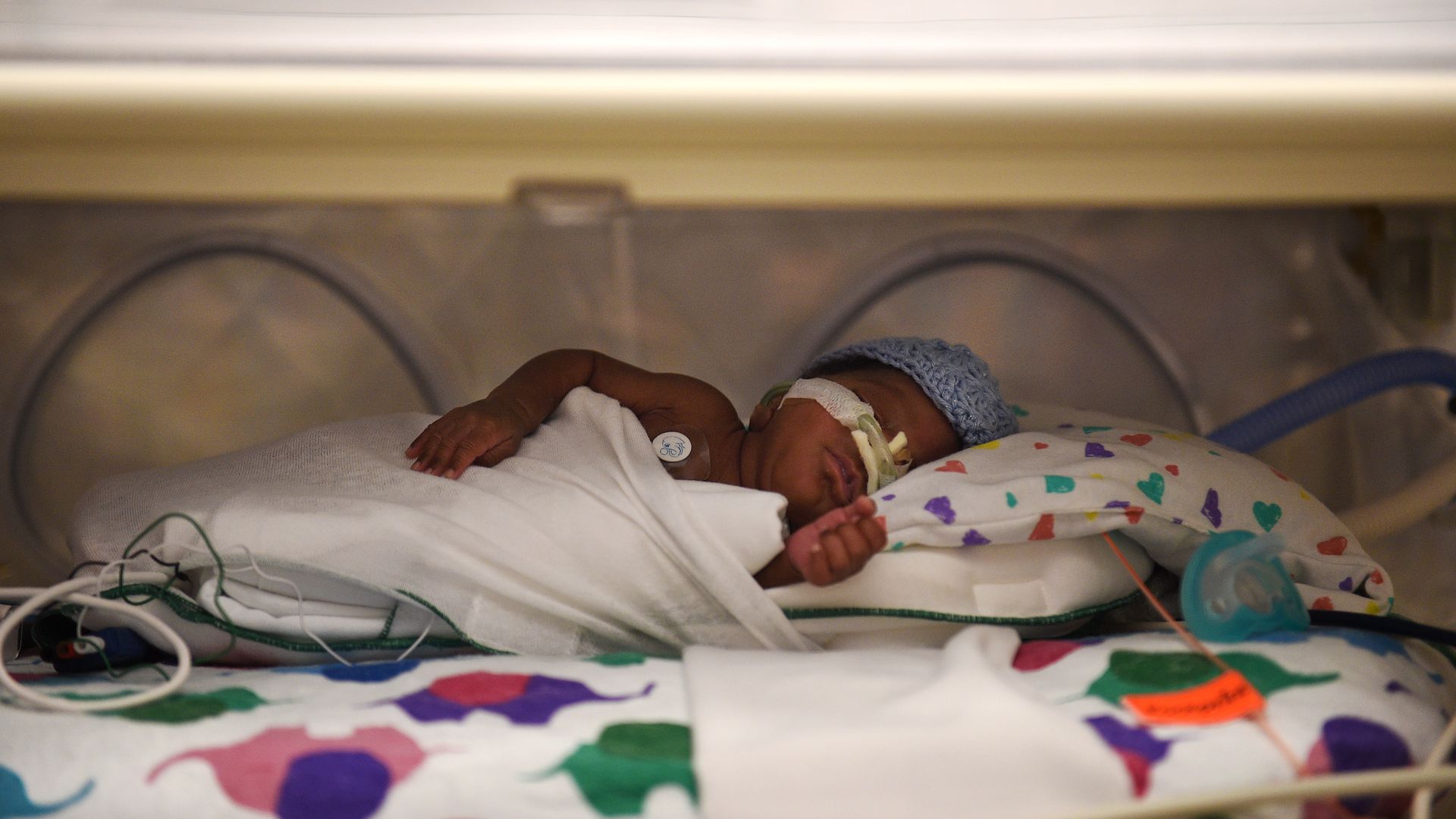
An infant is treated in a pediatric ICU. Photo: Astrid Riecken/The Washington Post via Getty Images
