Jul 29, 2019 - Health
Hospitals must post prices in new Trump administration proposal
Add Axios as your preferred source to
see more of our stories on Google.
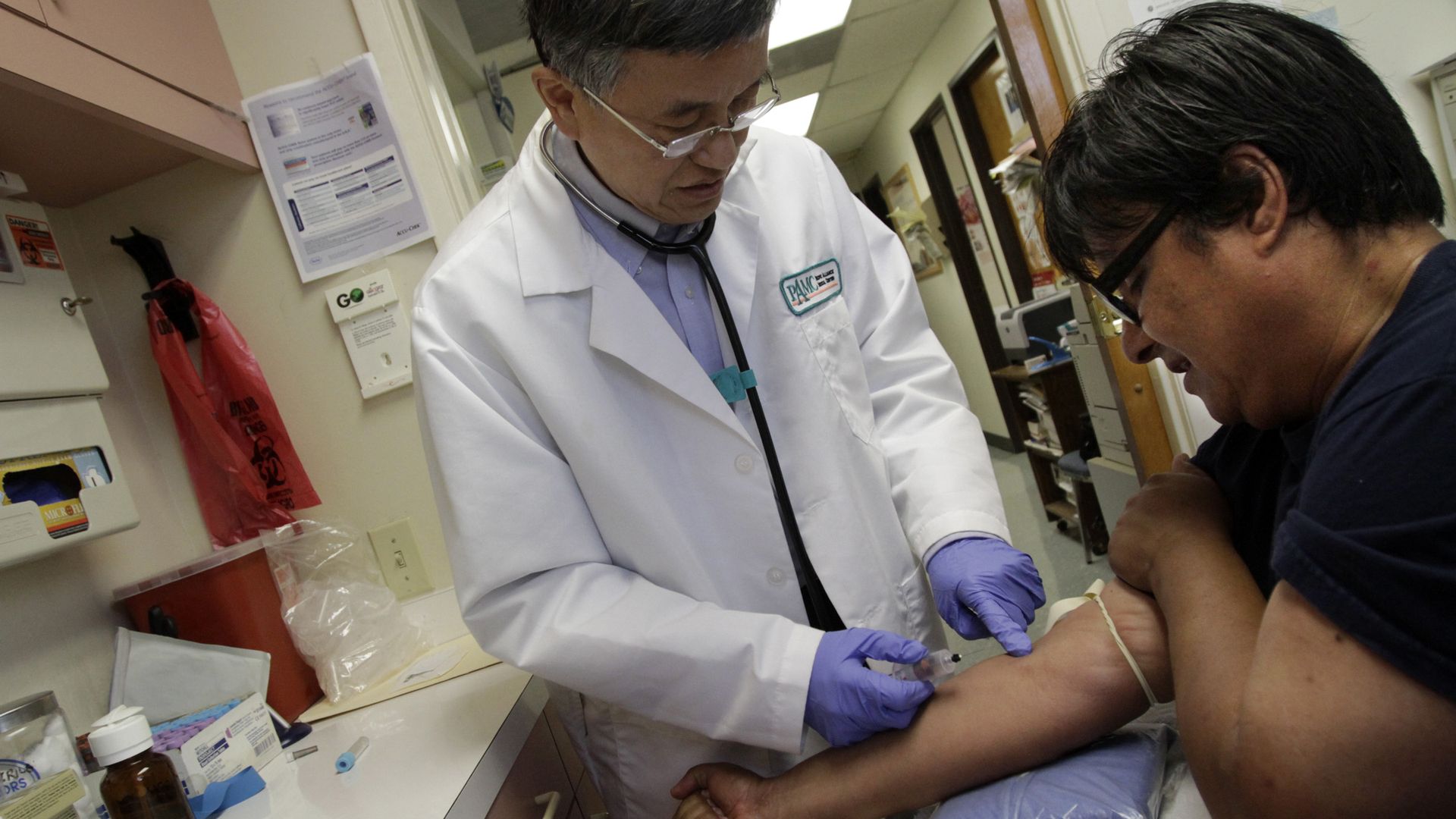
A patient likely has no idea how much this blood draw costs. Photo: Glenn Koenig/Los Angeles Times via Getty Images
