Women are more likely to die from cancer in the southern U.S.
Add Axios as your preferred source to
see more of our stories on Google.
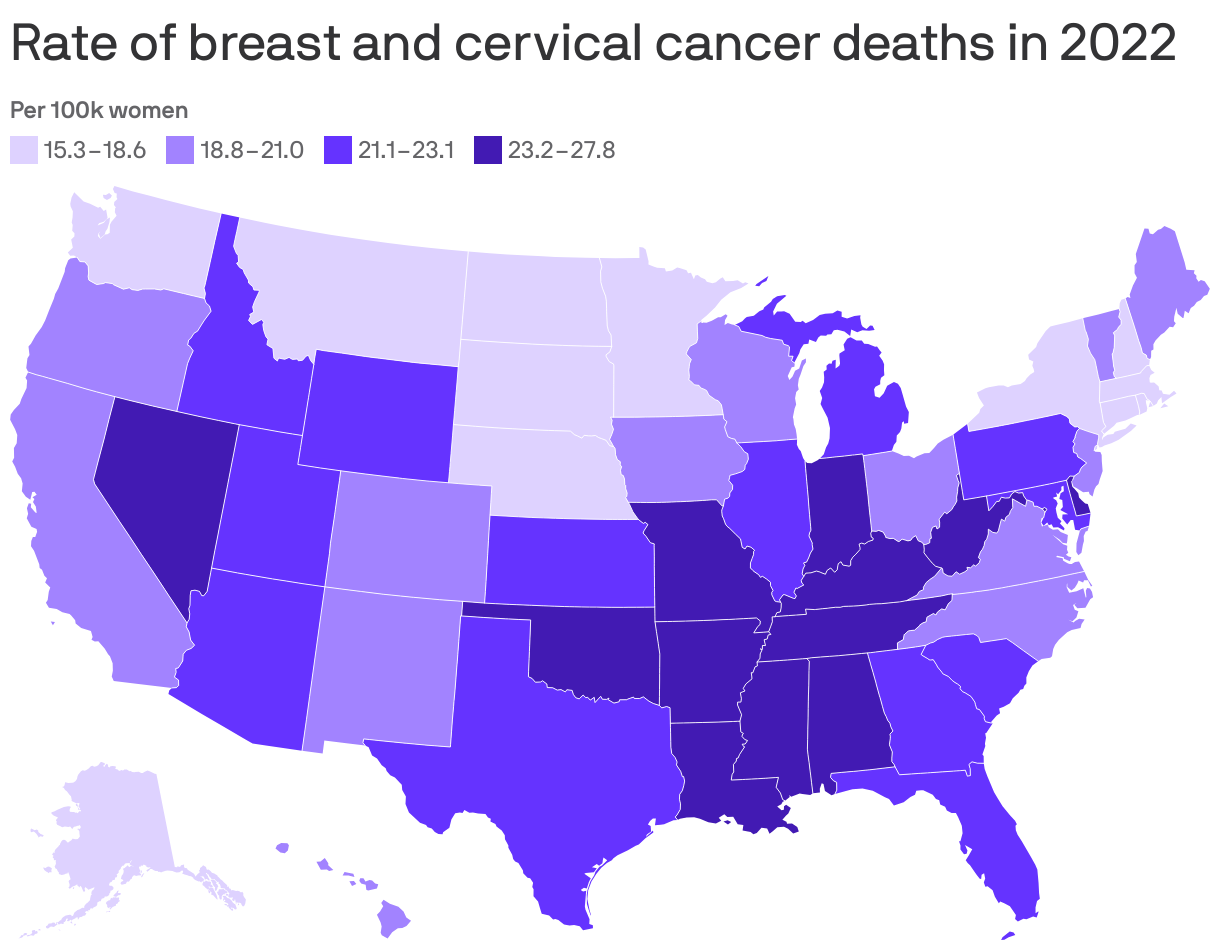
Women are likelier to die from breast and cervical cancer in a cluster of southern states where screenings and other preventive care lag behind the rest of the country.
Why it matters: The gap, shown in a new analysis of 2022 federal data by the Commonwealth Fund, illustrates how widening disparities in women's health aren't limited to reproductive care.
The big picture: Where a woman lives is becoming a key determinant in how dangerous it is to give birth or if she'll die from cancers considered treatable with proper screening and routine care.
- It's a trend that could intensify as OB-GYNs and applicants to medical residencies in other specialties increasingly move away from states with restrictions on abortion.
- "Rather than policies that might help narrow the divides [in women's health], we're seeing policies that can actually widen and deepen those divides," report author Sara Collins told Axios.
Breast and cervical cancer death is a proxy for assessing women's health services. Nationwide death rates are falling for both cancers, per the National Cancer Institute, as treatments advance and as free or low-cost screenings increase.
- But a cluster of states including Louisiana, Tennessee, Arkansas and Nevada saw between 23 to 28 deaths from cervical and breast cancer per 100,000 female residents in 2022, the Commonwealth Fund found.
- The national average was 20.9 deaths from breast and cervical cancer per 100,000 female residents in 2022.
- There also are well-documented racial disparities in who's dying from these cancers. Black women are 41% likelier than white women to die of breast cancer, for example.
Between the lines: States with higher breast and cervical cancer death rates tend to have lower cancer screening rates, the analysis noted.
- Many also have lagging vaccinations for the human papillomavirus, a major cause of cervical cancer, separate United Health Foundation data shows.
- The Affordable Care Act requires public and private insurance plans to cover preventive services like mammograms and cervical cancer screenings with no copays, but the requirement doesn't extend to follow-up screenings.
By the numbers: 11 of the 12 states with the highest breast and cervical cancer rates also ranked worse than average for women's health in general, according to the Commonwealth report.
- Mississippi, Texas, Nevada, Oklahoma and Arkansas ranked as the worst states for women's and reproductive health, according to the analysis.
- Massachusetts, Vermont, Rhode Island, Connecticut and New Hampshire were the top five.
Between the lines: The U.S. health system has placed more significance on tackling social factors that contribute to health outcomes in recent years. But determinants of health aren't the same in New Orleans as they are in Seattle, or even in a more rural part of Louisiana.
- "We have to start really looking at … specific communities when we're determining delivery of care," Irene Aninye, chief science officer at the Society for Women's Health Research, told Axios.
- "It's great we have guidelines" on screening and treatment, she said. "But then we actually need to get specific on how we're going to deliver it to these populations in these communities."
What's next: More resources need to be directed at research on improving screening and HPV vaccination rates where they're lacking, said William Dahut, chief scientific officer for the American Cancer Society.
- The Biden administration earlier this year pledged to invest hundreds of millions of dollars in women's health research and asked Congress to appropriate another $12 billion for the cause.
- Better data collection on race and ethnicity and more research including Black, Hispanic and Native American women could help close racial disparities in cancer deaths, too, the Commonwealth report said.
Editor's note: This story has been corrected to fix the spelling of Irene Aninye's name and to note that Aninye is chief science officer, not director of science programs.
