All signs point to a late summer COVID wave
Add Axios as your preferred source to
see more of our stories on Google.
If you've noticed a sudden rise in the number of people wearing masks while you're out and about lately, here's why: COVID-19 is on the upswing once again, according to closely watched metrics.
Driving the news: The late summer spread comes as a new variant, EG.5, is now the dominant form in the U.S., per CDC estimates — though it's unclear if that variant is directly responsible for the rising numbers.
Why it matters: Simply put, our guard is down.
- Many of us put COVID in our rearview mirrors, leaving us both mentally and practically ill-prepared for another wave.
- "Experts warn the U.S. is lacking critical tools to help manage future waves," as Axios' Sabrina Moreno recently reported.
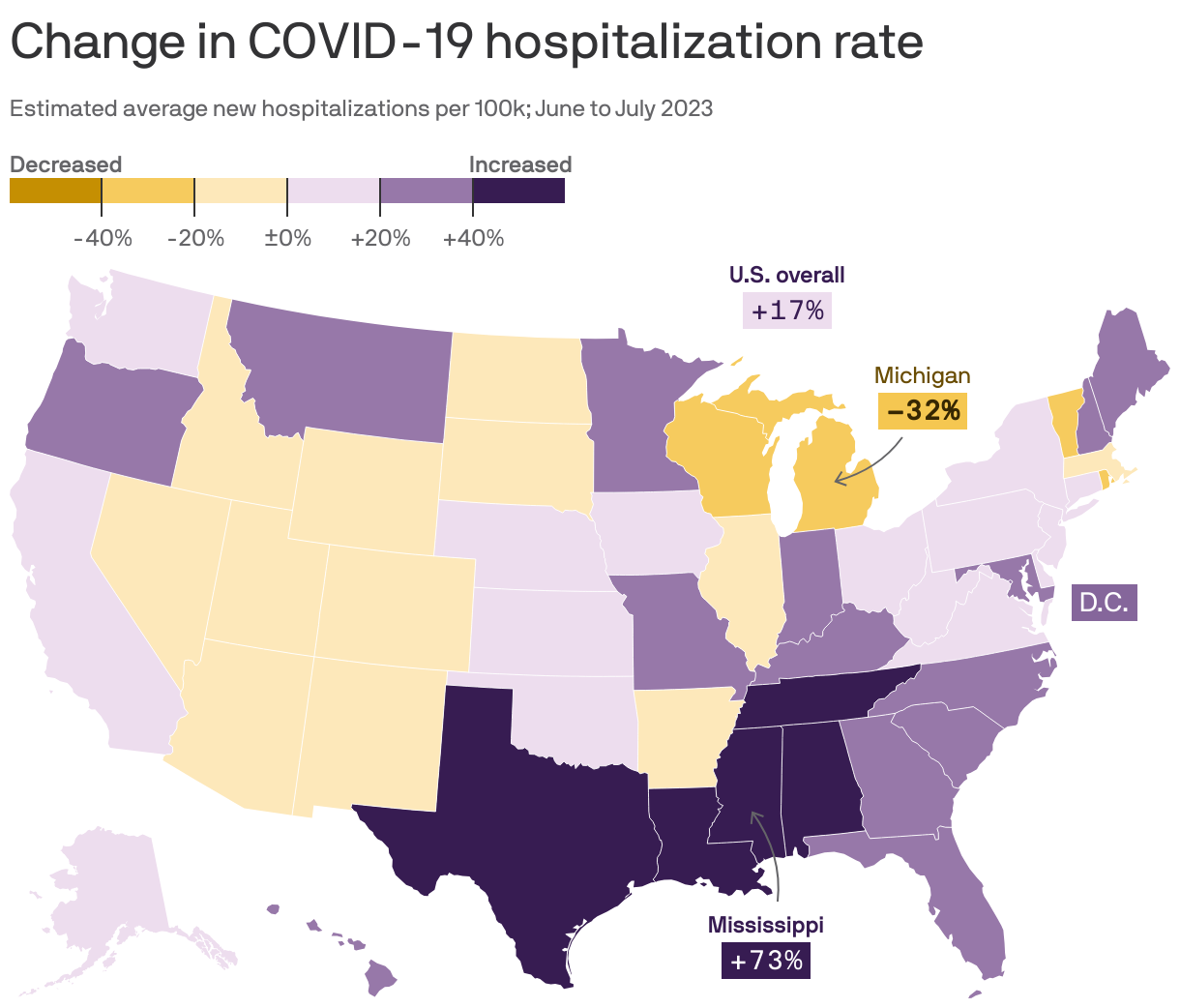
By the numbers: The average COVID-19 hospitalization rate nationwide rose about 17% between June and July, per the latest available CDC data.
- With so little testing happening these days compared to the height of the pandemic, hospitalization rates are now one of the best proxies for estimating broader viral spread.
Reality check: In both percentage change and raw terms, hospitalizations remain far below their pandemic-era peak.
- Nationally, hospitalizations are down 82% year over year.
- The CDC reports 10,320 overall hospital admissions in the week between July 30-Aug. 5, compared to more than 150,000 in one week in January 2022.
Zoom in: Hospitalization rates are rising the fastest in Mississippi (+73% month over month), Alabama (+66%) and Louisiana (+66%).
- Yet they're down in Michigan (-32%), Vermont (-31%) and Rhode Island (-31%).
- Remember from past waves that COVID moves about the country unequally, ebbing in some areas and flowing in others at any given point in time.
Yes, but: Hospitalizations aren't a perfect metric.
- Because older people are more vulnerable to severe COVID, for example, hospitalization rates are likely to be higher in states or communities with older populations. (To that end, nursing home cases are also rising, particularly in the Southeast.) Vaccination rates can be a factor too.
- Hospitalization rates are also a lagging indicator — it takes time for infected people to become sick, and more time still for them to become sick enough to require hospitalization. That delay means hospitalizations are a reflection of what's already happened, rather than a useful early-warning tool.
- The quality of hospitalization reporting can vary as well.
Other signs also point to increased spread.
- Wastewater analysis, for instance, is detecting rising levels of SARS-CoV-2 — the virus that causes COVID-19 — nationwide.
- Such analyses are especially useful in a world with less individual testing, as wastewater can reveal broad trends across wide areas, absent mass nose-swabbing campaigns.
Between the lines: This uptick comes at a less-than-ideal time with regard to booster availability.
- A newly updated booster is due out this fall. While it wasn't specifically designed with EG.5 in mind, it will likely offer at least some protection, experts told NBC News.
- Those behind on their shots need to decide whether it makes sense to wait for the updated booster, or to beef up their protection now in the face of this uptick.
The bottom line: There's no sign we're headed for anything like the waves of the peak pandemic era. But it's still an alarming trend, and a reminder that COVID will remain a public health concern for the foreseeable future.

