Why America was uniquely vulnerable to COVID
Add Axios as your preferred source to
see more of our stories on Google.
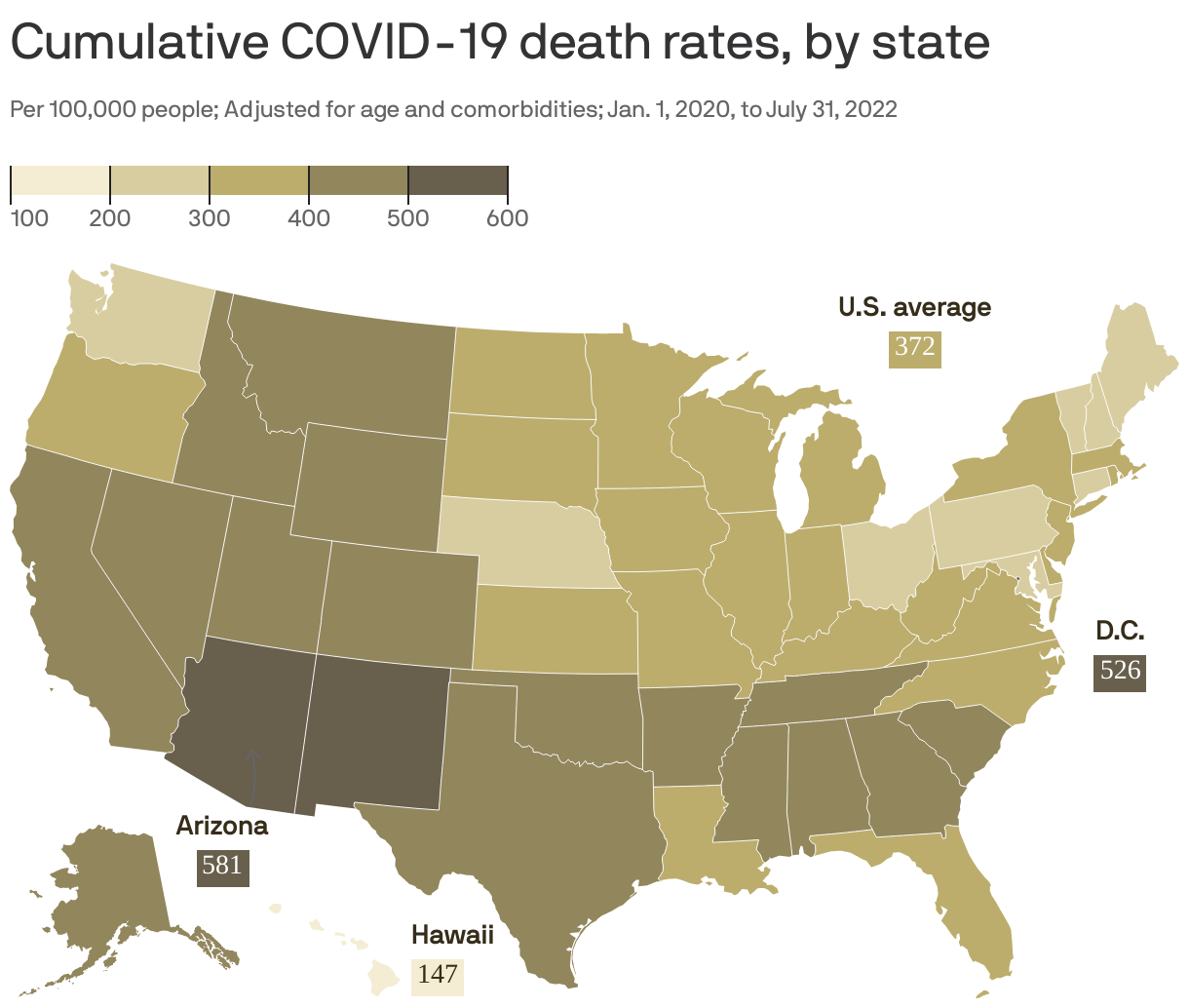
The pandemic experience varied sharply from state to state, with some of the highest adjusted death rates reported in Arizona, the District of Columbia and New Mexico, according to an analysis published in The Lancet.
Why it matters: It's among the first deep dives to explore the social and economic factors at play during the pandemic in the U.S., and it found a nearly fourfold variation in COVID infection and death rates between states.
What they're saying: "What is clear from our study is that COVID-19 exploited and compounded existing local racial inequities, health disparities, and partisan politics," co-lead author Thomas J. Bollyky, director of the Council on Foreign Relations' Global Health Program in the U.S., said in a statement. The combination of local factors increased the burden of disease and the likelihood of poor outcomes, he said.
By the numbers: States with higher poverty, lower rates of educational attainment, less access to quality health care and lower levels of interpersonal trust saw disproportionately higher rates of COVID infections and deaths.
- When adjusting the data to account for age and comorbidities, Arizona saw the highest COVID death rate (581 deaths per 100,000 people). Washington, D.C., (526 per 100,000) and New Mexico (521 per 100,000) were the second and third worst, respectively.
- On the flip side, Hawaii had the lowest adjusted COVID death rate with 147 COVID deaths per 100,000 people. It was followed by New Hampshire (215 per 100,000) and Maine (218 per 100,000).
The big picture: Previous studies have connected state politics with better or worse COVID outcomes or homed in on racial disparities linked to poorer outcomes.
- But this study offers a more nuanced view of how the combination of factors made certain states more vulnerable than others. For example, the analysis found no association between the political affiliation of the state governor and death rates. But one key predictor of infections and total COVID deaths was the share of people that voted for President Trump in the 2020 presidential election.
- Researchers also considered the benefits of protective measures like mandates against their harms, such as lost employment and drops in test scores.
- "Our study suggests that the policy mandates and protective behaviours adopted in this pandemic were effective in reducing SARS-CoV-2 infections but might have been associated with employment and educational trade-offs," the authors wrote, adding the trade-offs warrant study that could inform future protective measures.
- "The more robust a health system, the better a state performed in the pandemic, but only in states where the public was willing to make use of health care services for vaccination or to get early treatment for their conditions," senior author Joseph Dieleman, an associate professor at the Institute for Health Metrics and Evaluation, said in a statement.
Between the lines: The analysis found states with more mandates, such as those that encouraged mask use, mobility restrictions and vaccination — and kept them longer — experienced lower infection rates.
- But only vaccine coverage had a strong association with the state-by-state variation in COVID death rates, they said.
- "Ultimately our public health policies seem capable of preventing transmission, but other societal factors like poverty, education attainment, and access to high-quality healthcare might have muddled the response and led to death rates being highest in some states that didn't have tremendously high infection rates," Dieleman said in a statement.
