Rural hospitals again face financial jeopardy
Add Axios as your preferred source to
see more of our stories on Google.
After weathering the pandemic with federal COVID aid, rural hospitals are facing a convergence of challenges that could leave many facilities deep in the red and at risk of closing as soon as the end of this year.
Why it matters: Hospitals are among the biggest employers in rural communities and the only health providers in large swaths of the country. But they've been operating on the edge for years, tending to older, sicker patients who often can't afford care.
Driving the news: Hospitals couldn't persuade Congress to delay a scheduled 2% cut in Medicare payments, then were frustrated by a Medicare payment proposal for 2023 they say ignores the effects of inflation, labor and supply cost pressures.
- Many facilities have burned through federal COVID provider relief funds and Paycheck Protection Program loans that helped them cope with staffing and supply shortages and lower demand as patients deferred care.
- "The data would suggest we will see a lot more rural hospital closures at the end of this year and into 2023," Alan Morgan, chief executive of the National Rural Health Association, told Axios.
- Closures could dramatically reduce access to care, forcing patients to travel longer distances for inpatient services, substance use treatment and other needs, per the Bipartisan Policy Center, which recommends new payment models and incentives to retain health workers to ease the crunch.
- But sympathy may be limited for an industry that recently received large sums of federal dollars to get through the pandemic.
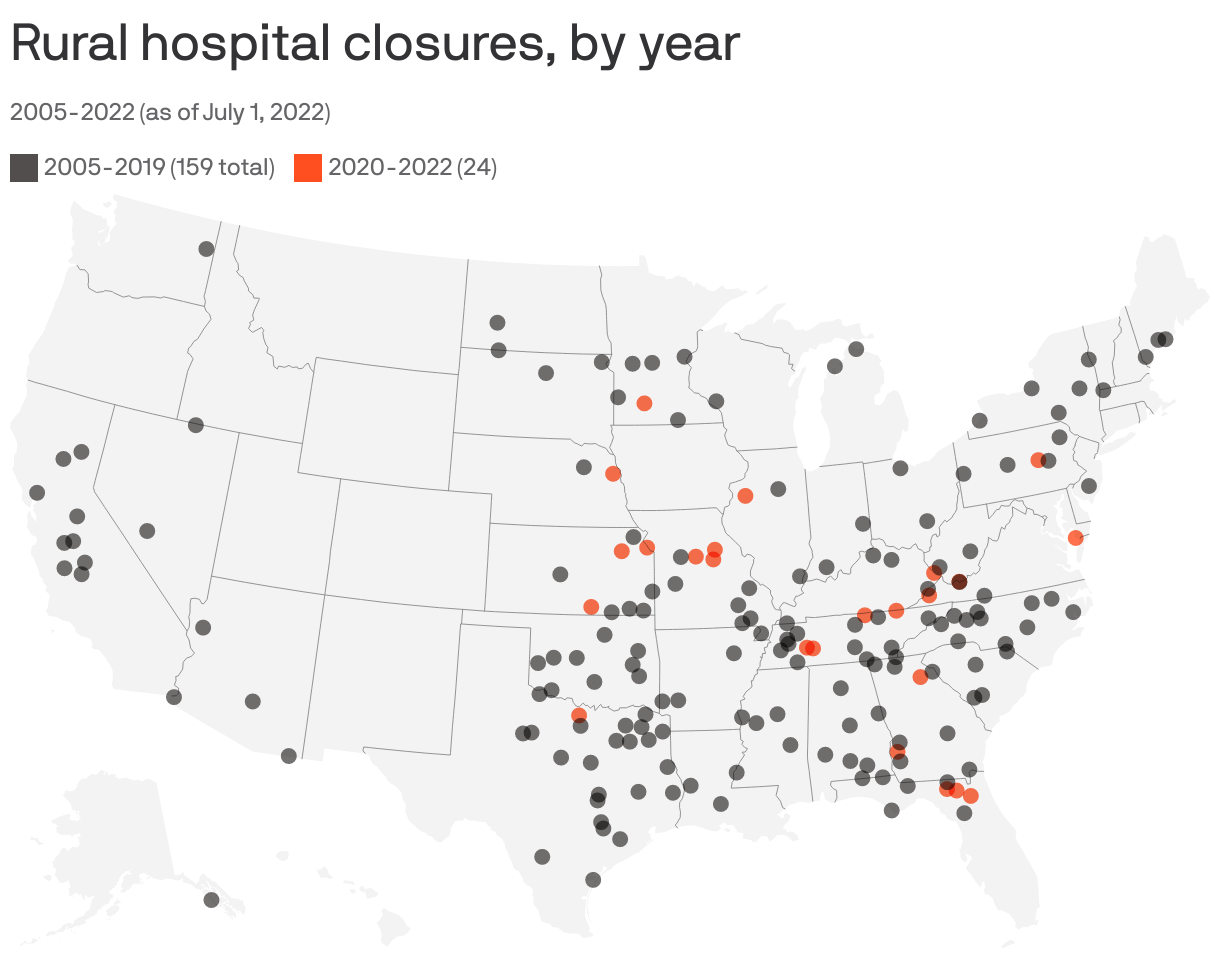
Flashback: Rural hospital closures are not a new story — since 2010, 140 rural hospitals have closed, according to the University of North Carolina's Rural Health Research Program's tracker.
- The majority of closures were in the Southeast, where "you've got a lower-income, sicker population that is underinsured or uninsured," Morgan said.
- The pandemic forced facilities to lay off staff and, in some cases, restrict services just to COVID patients. But Congress responded with a bailout, including $175 billion to hospitals and clinicians around the country that was particularly advantageous to rural facilities.
- While revenues might have dropped, margins at most facilities held firm, a May study in JAMA found.
- Since the beginning of 2021, just five rural hospitals have closed, compared to 19 that closed in 2020 and 18 in 2019.
Go deeper: Experts say many of the rural facilities are running on unsustainable business models.
- Some "only had one-third of their beds filled, with a low occupancy rate, and then you have to run a hospital with a lot of fixed costs and that's a fundamental reason that hospitals are facing financial challenges," Ge Bai, a Johns Hopkins University professor who studies rural hospital finance, said.
- The situation leaves facilities in peril without federal aid, especially since many rural residents bypass their local facilities for elective surgeries, Bai said.
What's next: With federal funds depleted, experts say many rural facilities are back on their shaky pre-pandemic footing.
- There's growing pressure from labor and supply costs, as staffing shortages and supply chain issues combine with inflation to send margins into negative territory.
- The situation is especially tough for independent or publicly run facilities that aren't part of integrated health care systems and face obstacles to striking better purchasing agreements.
- "For small rural hospitals, generally, they operate with small volumes regularly, and as such even slight increases in the supplies they have to utilize to take care of sicker patients can create dramatic upswings in costs," Erik Swanson, senior vice president at Kaufman Hall, told Axios.
What we're watching: Sicker patients, some of whom deferred care during the pandemic, will still flock to the facilities — but may be unable to pay.
- Some hospitals may find relief in a new CMS-led care delivery arrangement that kicks in next year and will allow small rural hospitals to provide continued access to emergency services, observation care and added services.
- But the Bipartisan Policy Center notes that while payments would cover services beyond typical Medicare reimbursements, the payments still may be set too low or be too restrictive to prove useful.
- "We can do more structural innovation to help rural hospitals and rural residents access to affordable care," Bai said.
