COVID missteps hang over monkeypox response
Add Axios as your preferred source to
see more of our stories on Google.
The United States is applying some of the hard lessons it learned during the COVID pandemic to the monkeypox outbreak. But it's still playing catch-up.
Why it matters: Monkeypox won't bring the death and suffering COVID did, but public health experts say it could take hold in the population without robust testing, vaccinations and communicating about the health risks.
- "We’re just seeing the tip of the iceberg here," said Megan Ranney, academic dean at the Brown University School of Public Health. "Many of us are concerned it could only be a matter of time before it spreads more generally,” she said.
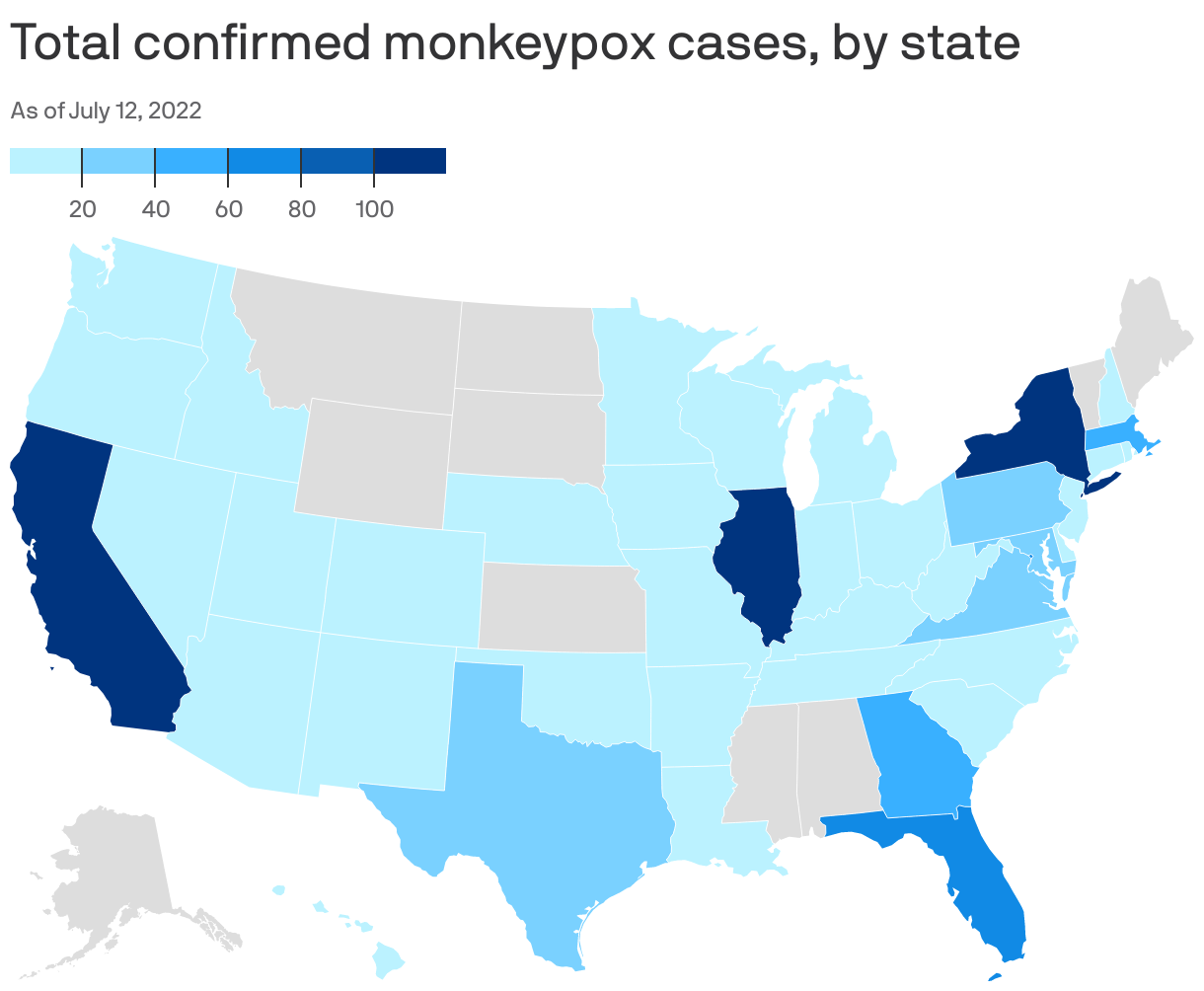
State of play: At least 767 cases have been identified in 37 states and the District of Columbia, though it's likely the actual count is higher.
- Testing was first confined to public health laboratories and hard to access, similar to the beginning of the COVID pandemic. The CDC last month began pushing out tests to five commercial labs to increase capacity, including Labcorp, which last week said it will start processing samples.
- The U.S. also is vaccinating people with confirmed cases and their immediate contacts. But shots were slow to arrive, and the FDA took nearly two months to approve the release of 1.1 million doses that were in storage in Denmark, according to New York magazine.
- HHS last week said it's making an additional 144,000 doses of Bavarian Nordic's JYNNEOS vaccine available to states and other jurisdictions, on top of the 20,000 doses that have already been sent to 15 states and cities.
- Even with vaccines and testing, public health departments are facing a familiar scenario and need to investigate cases, isolate people confirmed to be ill and deploy effective contact tracing to get control of a virus that's spreading widely.
Zoom in: Local health officials are still getting their hands around the scope of the outbreak, using tools like wastewater surveillance that proved effective detecting COVID-19 cases before symptoms arise.
- Testing picked up traces of monkeypox as far back as June 20 on the west side of San Francisco, and just a week later, monkeypox was detected in a different sewershed in the other side of town, per the Sewer Coronavirus Alert Network.
- "It can provide a community-level perspective ... and give us confidence that we are or are not following up on outbreaks with proper resources," Marlene Wolfe, a professor at Emory University and researcher for the network, said of the surveillance.
Between the lines: Because the variety of the virus circulating in the U.S. is spread mostly through intimate contact, much of the surveillance so far has fallen to primary care providers, including sexual health clinics.
- Health authorities are trying to focus on gay and bisexual men who've borne a disproportionate percentage of cases without stigmatizing them.
- "We'd like to make sure this doesn't disseminate widely into that community and it's of concern to the broader community because individuals who get infected do pose a risk to family members," Ali Khan, who leads the College of Public Health at the University of Nebraska, told Axios.
- But there aren't enough supplies and health workers: STD clinics report a shortage of test tubes, swabs and other equipment needed to collect specimens. Elizabeth Finley of the National Coalition of STD Directors said more money is needed to secure supplies and hire more staff.
The big picture: The lagging response has left knowledge gaps about precisely how monkeypox circulating in the U.S.
- "How many days does it take from illness to diagnosis?" Khan said. "Are we catching these [cases] fast enough?"
- Contact tracing and other surveillance could identify large clusters of cases traced to an event or setting, not unlike early in the COVID-19 response.
- One advantage is monkeypox changes much slower than the coronavirus, potentially giving officials more time to connect cases, find at-risk individuals and cut chains of transmission.
- But as with COVID, it's hard to say who will really be protected as the virus continues to circulate and evolve. For that reason, experts caution against an "all-or-nothing" public health message that leaves the impression that vaccinated people will never get sick.
- "The message should be if you do get vaccinated against monkeypox, you will have a much less likelihood of getting it and be less likely to spread it," Aaron Glatt, an epidemiologist at Mount Sinai, told Axios.
