American women more likely to die from preventable causes
Add Axios as your preferred source to
see more of our stories on Google.
American women of reproductive age score worse on just about every major health metric compared to their peers in other wealthy countries.
Why it matters: It's no secret that the maternal mortality rate in the U.S. is the highest among developed nations.
- But a new report from the Commonwealth Fund offers a higher resolution view of the role that cost plays as a barrier to care for women of reproductive age.
- "Maternal deaths and complications may be a bellwether for the U.S.’s wider failures with respect to women’s health and health care," the authors wrote.
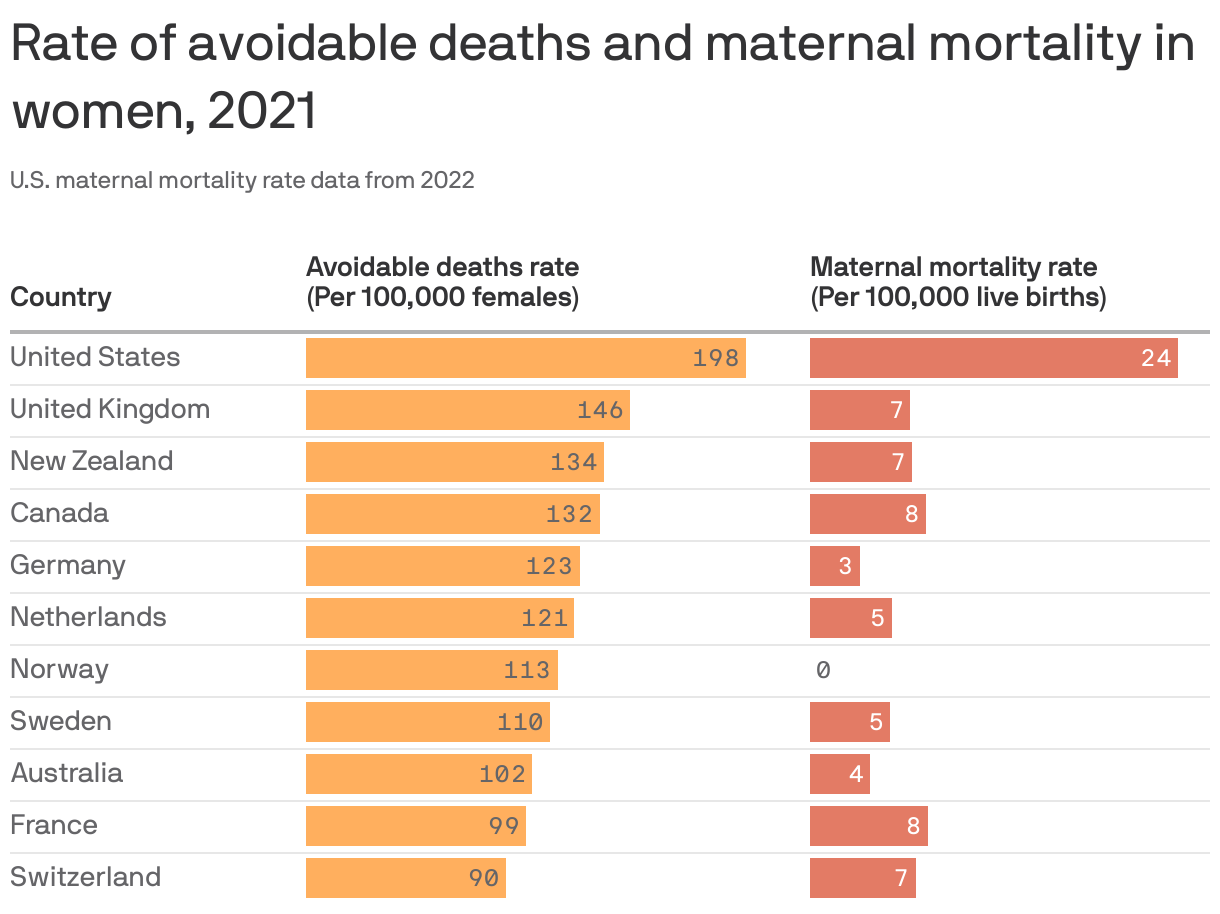
By the numbers: The researchers looked at women ages 18–49 in 11 developed nations and found the U.S. had the highest maternal mortality rate by far at 23.8 maternal deaths per 100,000 live births.
- When broken out by race, the rate was 55.3 deaths per 100,000 births for Black women, or about triple the 19.1 deaths per 100,000 for white women and 18.2 deaths per 100,000 for Hispanic women.
Zoom out: American women also were among the most likely to have two or more chronic conditions, skip necessary care due to cost and have the worst rate of avoidable deaths. For instance...
- Chronic conditions: The U.S. and Canada tied for having the highest percentage of women of reproductive age — 20% — who had two or more chronic conditions in 2020. Only about 7% of women in this age group in Switzerland had two or more chronic conditions.
- Delayed care: Nearly half (49%) of American women in this demographic said they'd skipped or delayed care in the last year. The country with the second highest percentage of women who'd skipped or delayed care in the last year was Australia (32%). Only 12% of women in the Netherlands had.
- Avoidable deaths: The U.S. was also the worst by this metric, with 198 avoidable deaths per 100,000 women annually. The next highest rate was in the U.K. where they had 146 deaths per 100,000 women. Switzerland had 90 avoidable deaths per 100,000 women annually, the lowest rate of the countries examined.
What they're saying: Across the U.S., access to women's health care is a big problem with only 50% of all counties having OB/GYNs and with rural providers closing, says Mary Jacobson, chief medical officer at Alpha Medical, a virtual primary care group which specializes in women's health.
- Preventative care for women is also often poorly covered, she tells Axios. But the problem goes far beyond those myriad access problems and far beyond their sexual health care.
- "In medical schools, there's not enough education about gender-based care or the sex differences in different medical conditions," she says. The benchmark for medical guidance is often based on the benchmark of a white man and assumed to be the same for women of all races, which is often not the best care.
- "There's also implicit bias for women. Let's say there's a woman who comes in, she's in her mid-40s and has chest pain, maybe the first diagnosis they think of is anxiety. It's not a heart attack, it's not angina, it's not cardiovascular disease. It's a missed opportunity," she adds.
Driving the news: Congress is weighing a number of bills aimed at tackling the maternal mortality crisis in the United States.
- Several provisions that were part of the Black Maternal Health Momnibus Act were included in recent reconciliation language passed by House committees, according to the Georgetown Health Policy Institute.
The big picture: America's health care hasn't compared favorably to other wealthy nations in recent years.
- In a study published in the BMJ, the U.S. was top among wealthy nations when it came to the highest absolute number of excess deaths during the COVID pandemic in 2020.
The bottom line: "The U.S. health care system too often fails women of reproductive age," the Commonwealth Fund wrote.
- "The COVID-19 pandemic has unveiled the true extent of health and racial inequities in U.S. health care and exacerbated its many weaknesses, including underinvestment in primary care and mental health."
