What it takes to persuade the unvaccinated
Add Axios as your preferred source to
see more of our stories on Google.
Vaccine uptake is fading, but doctors and health care workers are trying to reach the tens of millions of unvaccinated Americans — one conversation at a time.
The big picture: Persuading the remaining unvaccinated takes a lot more time and effort, and health care workers who have found success are not writing off holdouts as anti-vaxxers.
"You do need to meet people and individualize your approach," said Odilichi Ezenwanne, a primary care physician at the Aaron E. Henry Community Health Services Center in Tunica, Mississippi, where just 50% of the county is fully vaccinated as of Feb. 9.
- "You have to understand their own reasons for restraint or hesitancy ... that's when they really open up to you."
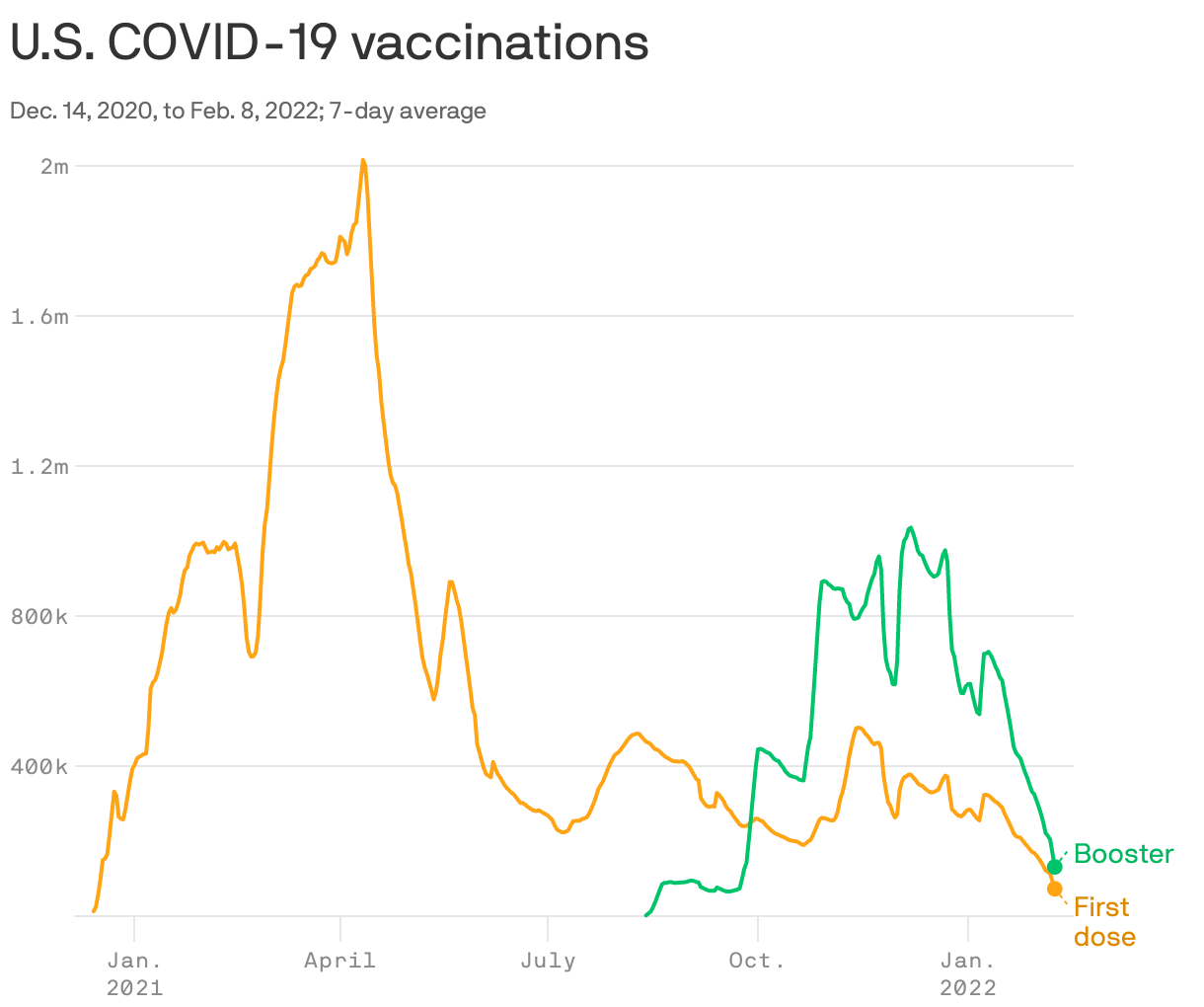
By the numbers: CDC data shows fewer than 100,000 people are getting their first COVID vaccine dose every day, the lowest daily average since the vaccines were available in late 2020.
- Fewer than 200,000 people are getting booster doses every day, by far the lowest rate since boosters were recommended last September.
Between the lines: Ezenwanne, who has traveled around his community to educate and vaccinate people over the past two years, said the "three Cs" often explain the lingering reluctance.
- Confidence: People may not trust the vaccines, especially with how quickly they were developed. There's also deep mistrust of the government.
- Convenience: The vaccine may not be easy to get. People may not live close to a pharmacy or health center, or people can't afford to take off work if they come down with side effects. Language and immigration status are also barriers.
- Complacency: People may not think COVID-19 is a big deal, or they wonder what the point of the vaccine is if you can still catch the virus. (The vaccine drastically reduces one's chances of getting hospitalized or dying.)
Yes, but: Taking the time to sit down with people is difficult, and explaining the benefits of the vaccines won't always lead to someone getting the shot, clinicians admit.
- But nurturing those relationships has proven to be the best way to change people's minds.
- "I hope it moves people to consider things," said Dimitri Drekonja, an infectious disease physician at the Veterans Affairs hospital in Minneapolis who recently helped a skeptical patient and parent get vaccinated. "Sometimes I find out months later, they did get vaccinated ... and frankly, it makes my day."
The bottom line: "If all health care providers start to listen more and talk less, we'll make a bigger impact," said Ana Maria Barbosa, a nurse and "vaccine ambassador" at the Brockton Neighborhood Health Center in Massachusetts.
