The big Medicare Advantage players keep getting bigger
Add Axios as your preferred source to
see more of our stories on Google.
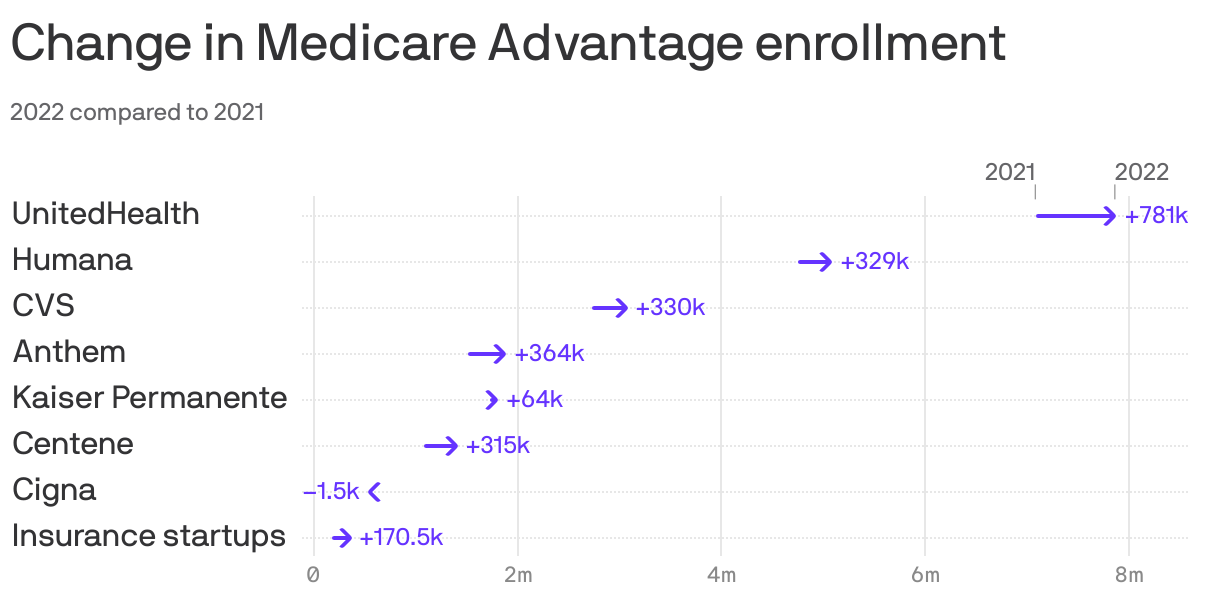
Six health insurers control roughly three-quarters of the fast-growing Medicare Advantage market, according to an Axios analysis of federal data.
Why it matters: Medicare Advantage enrollment hasn't slowed down in 2022, even though dismal projections from Humana and Cigna freaked out Wall Street earlier this month, and concentration at the top remains high.
The big stat: UnitedHealth Group had almost 7.9 million MA members as of Jan. 1, the most of any insurer and an 11% increase from the 7.1 million members it had at the same time in 2021, according to federal data.
- That means UnitedHealth captured roughly one out of every three people who joined Medicare Advantage this year.
By the numbers: Here's the MA enrollment totals for the other major insurers, compared with the same period in 2021.
- Humana: ⬆️ 7% to 5.1 million.
- CVS: ⬆️ 12% to 3.1 million.
- Anthem: ⬆️ 24% to 1.9 million.
- Kaiser Permanente: ⬆️ 4% to 1.8 million.
- Centene: ⬆️ 29% to 1.4 million.
- Cigna: ⬇️ 0.3% to less than 553,000.
Between the lines: If anything, UnitedHealth, CVS, Anthem and Centene ate some of Humana's and Cigna's lunches, but all of their lunches were still large.
The big picture: Even a small number of MA members translates into big bucks, which is why startup insurers have rushed to enter the $412 billion market.
- The federal government pays MA plans more than $1,000 every month, on average, for every person they cover.
- Startup insurer Devoted Health doubled its MA enrollment from 2021 to 2022, tallying 63,000 members as of Jan. 1. That translates to at least $750 million of annual revenue.
Yes, but: Four leading MA startups — Devoted, Alignment Healthcare, Clover Health and Bright Health — cover 350,000 MA members combined, which is a small fraction of national enrollment.
- UnitedHealth added double that amount of people to its rolls, just this year.
Zoom in: MA also is playing out very differently in local markets.
- For example, Highmark and UPMC are the health care oligopolies in Pittsburgh, operating the hospital systems and MA plans in the area.
- Highmark now has the upper hand in the city: It gained 77,000 MA members for 2022, now totaling 318,000, while UPMC lost members, falling below 200,000.
The bottom line: Health insurers are fighting to attract seniors who continue to flood into the MA market, but problems surrounding MA's coding and excessive payments to insurers remain unresolved.
