Jun 15, 2021 - Health
Study: Nearly a quarter of COVID-19 patients developed new or long-term conditions
Add Axios as your preferred source to
see more of our stories on Google.
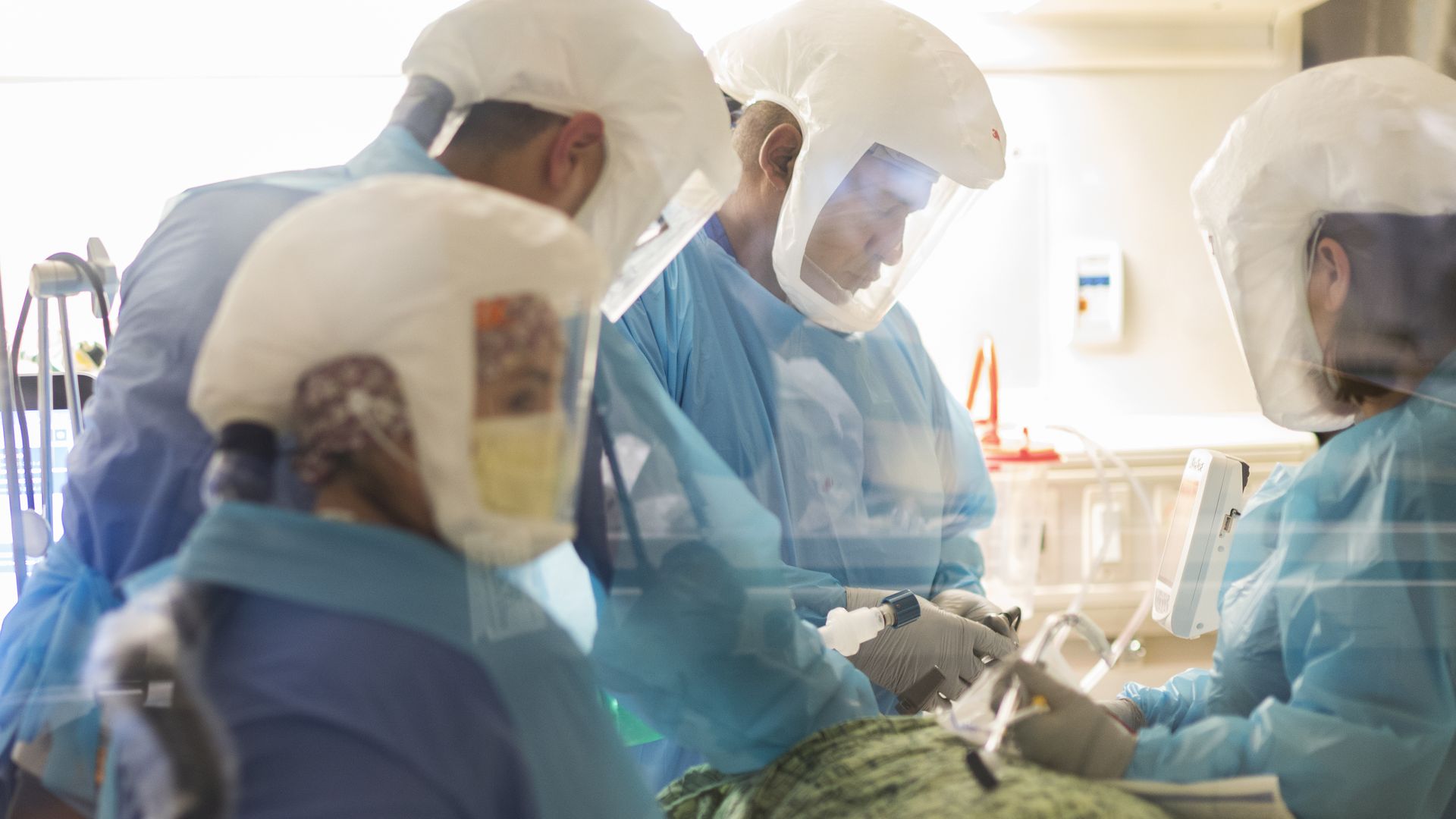
Healthcare workers incubate a patient at a Covid-19 Intensive Care Unit (ICU) of Salinas Valley Memorial Hospital in Salinas, California, U.S., on Jan. 26, 2021. Photo: Nic Coury/Bloomberg via Getty Images
