HPV vaccination rates show progress, but off track for 2020 goal
Add Axios as your preferred source to
see more of our stories on Google.
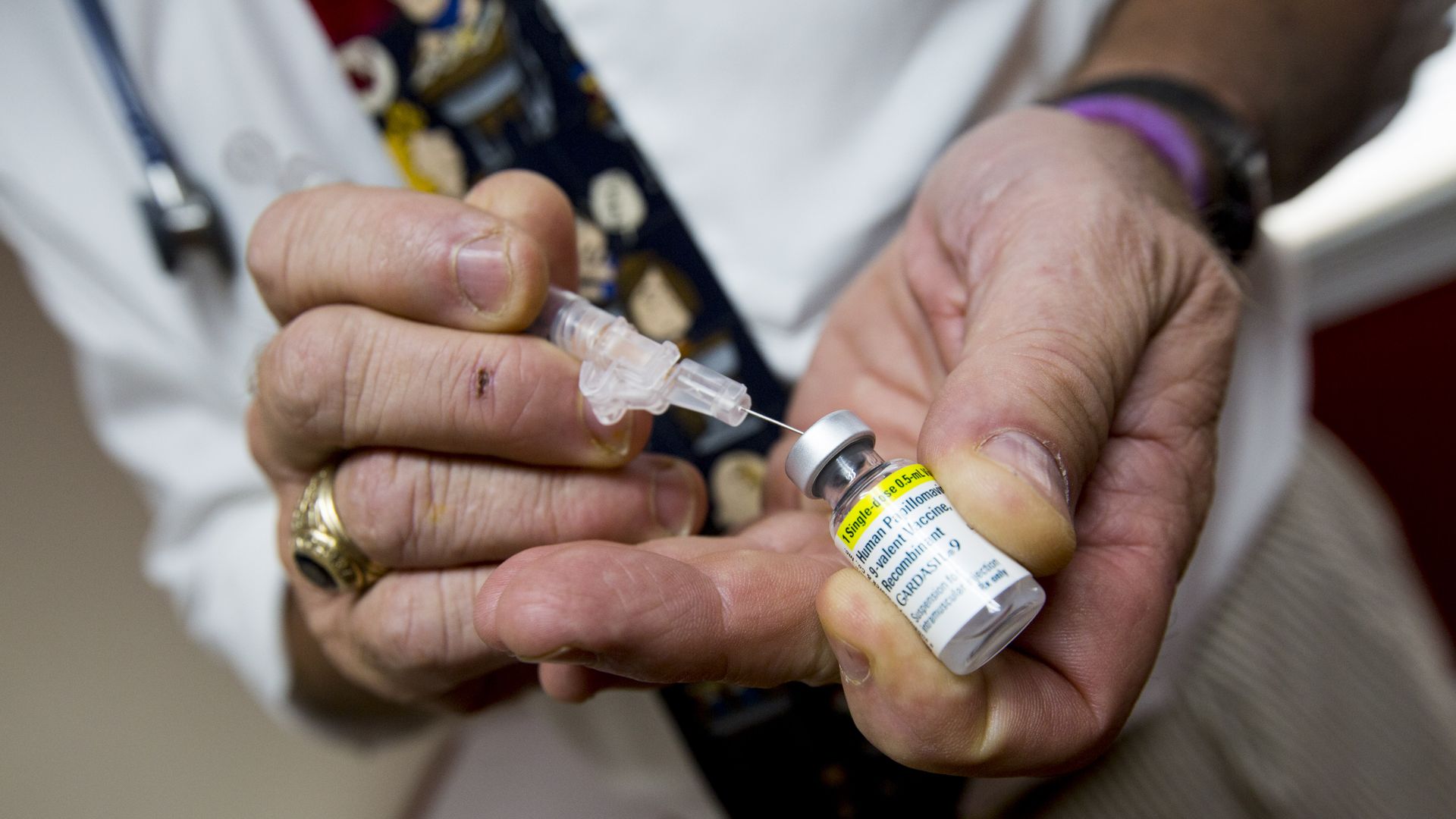
A pediatrician prepares a shot of the HPV vaccine Gardasil for a patient. Photo: Keith Bedford/The Boston Globe via Getty Images
In 2006, a safe and effective human papillomavirus (HPV) vaccine became available to protect against cancers caused by HPV infection. HPV vaccination rates in adolescent boys and girls are rising, though still not fast enough, with HPV-linked cancer cases soaring by nearly 45% between 1999 and 2015. Fewer than half of American adolescents have been fully vaccinated, far short of the 80% goal officials have set for 2020.
Why it matters: The lifetime risk of acquiring an HPV infection is approximately 80%. Each year, 14 million new cases are diagnosed in the U.S., and 79 million Americans are currently infected, putting them at increased risk of cervical cancer as well as throat, vaginal, penile and anal cancers. A more comprehensive campaign is needed to make the world free of HPV infections.
All 70 National Cancer Institute–designated cancer centers recommend that boys and girls ages 11 to 12 receive two doses of the HPV vaccine, 6 to 12 months apart. Women who have not received the vaccine should undergo HPV screenings. In some cases though, as for throat cancer, no screening test exists.
What to watch: A trial is underway to assess whether a single vaccination is sufficient to confer immunity. Also, there is a new screening recommendation as an option for women 30 and over, moving from a pap smear every 3 years to the more reliable HPV molecular test every 5 years.
A more comprehensive campaign might also include the following objectives:
- Remove Barriers: Free or low-cost and convenient access to HPV vaccination and screening is needed, everywhere from schools and retail settings to faith-based organizations.
- Enact Policy: Legislators should make vaccination mandatory with an opt-out provision and add vaccination rates as a quality measure for health-care providers.
- Launch knowledge campaign: Government, industry, healthcare institutions and media should launch a multi-pronged educational campaign using mass media, celebrity endorsements, and advertisements.
The bottom line: The 33,000 HPV cancers that will be diagnosed in the U.S. this year reflect the lack of vaccination in the past decade. Parents, legislators and doctors must continue improving vaccination rates to reduce the incidence of these preventable cancers.
Ronald DePinho is a professor and past president of the University of Texas MD Anderson Cancer Center.
