Study: Emphasizing a drug's side effects can trigger those effects
Add Axios as your preferred source to
see more of our stories on Google.
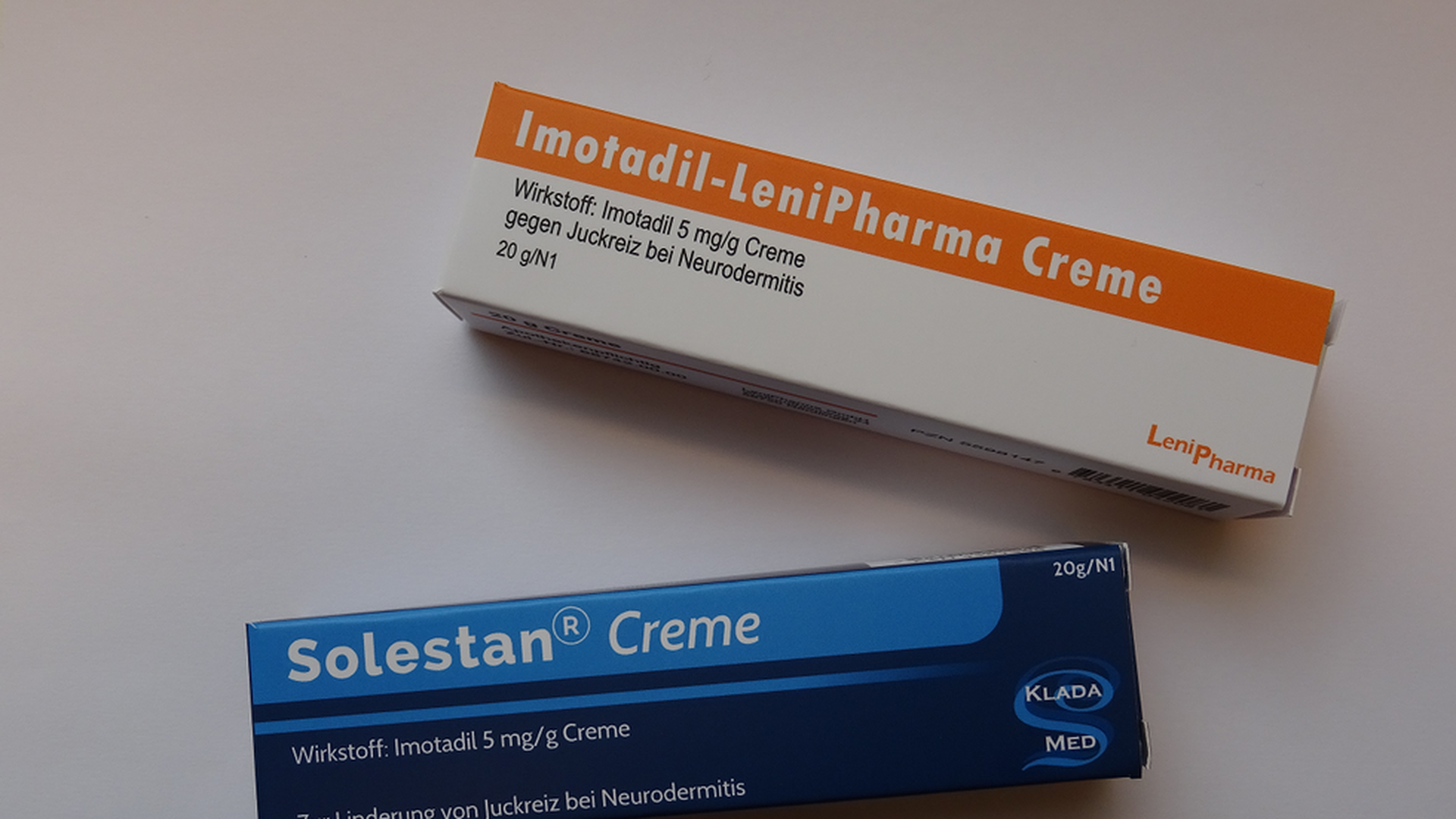
The "inexpensive" cream (on top) and "expensive" cream used in the study. Photo: Alexandra Tinnermann / Institute of Systems Neuroscience in Hamburg, Germany
Most people know about the placebo effect — when a person perceives, and then often receives, a beneficial health impact from a treatment that actually isn't directly addressing their condition. Studies have also shown people's perception of a higher-priced drug is that it will provide its remedy better.
Now, in a new study published Thursday, the flip side of that coin — called the nocebo effect — has been seen in people who reported worse side effects when given what they thought was a higher priced medicine.
Why this matters: "Understanding how nocebo effects work means that health care providers could actively use this knowledge in their way of talking to patients, how they explain things to patients and also which information to mention and to avoid in order to minimize the effect," one of the study authors, Alexandra Tinnermann, told Axios.
Study details: The team told 49 participants they were testing a prescription cream to relieve itch, and that one possible side effect was local skin sensitization, which could lead to increased pain perception. The group was divided into two groups — one to take an expensive-looking cream in a fancier box and the other to take a less expensive cream in a generic-looking box (both creams had no active ingredients).
The researchers then treated the participants with painful heat stimuli and recorded the neural activation in the brain and spinal cord.
Their findings: The participants who used the "expensive" cream reported a higher rate of pain that became more pronounced over time, compared to the participants using the "cheaper" cream. The researchers also determined the altered sensations due to perceived price were associated with differences in two particular brain regions (the periaqueductal gray and rostral anterior cingulate cortex).
Luana Colloca, a neuroscientist at the University of Maryland who was not part of this study, told Axios the study is interesting in how it shows the role the spinal cord and the two brain areas plays in switching pain on and off and the very real impact a person's perception can have on their pain levels.
"It's important [for clinicians and trial researchers] to know the words they use, the way they communicate, their behavior can raise perception of the side effects," says Colloca, who also wrote a perspective published with the study. She warned that in the past, misleading information about side effects led people to discontinue their treatment resulting in some of them dying from heart attacks or strokes.
Go deeper: Listen to a podcast of an interview with Tinnermann (at 10:01) and a YouTube video about the study.
