Groups representing PBMs, drugmakers and physicians all ramped up year-over-year spending on lobbying in advance of the December government funding deal, an Axios review of new federal lobbying disclosures found.
Why it matters: Powerful health care interests were laser-focused on the possible inclusion of health provisions that would have cracked down on PBMs, reformed drug patents and delayed scheduled Medicare physician payment cuts.
- Although the provisions were ultimately dropped from negotiations, some could resurface in reconciliation or another short-term spending deal.
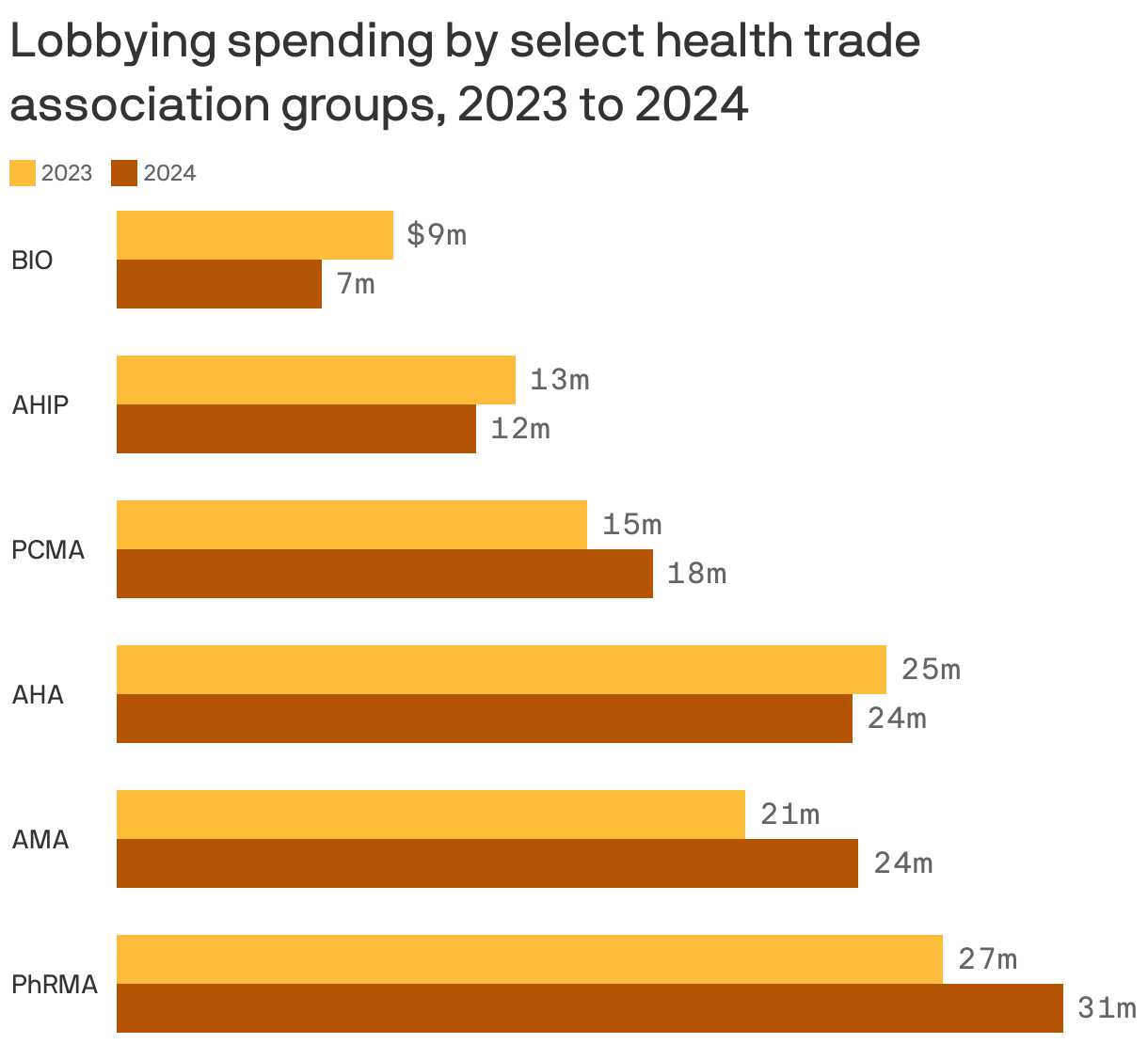
By the numbers: PhRMA spent $31 million in 2024, up from $27 million in 2023.
- The trade group boosted its activity as the funding deadline approached, spending $7.6 million in Q4, compared with $6.9 million in Q3.
- PCMA spent almost $18 million in 2024, compared with $15 million in 2023. And that's after only $9 million total in 2022.
- The group was fighting multiple bipartisan proposals that would have changed the way PBMs are paid or would have reformed their business practices.
- PCMA also upped spending by about $1 million from Q3 to Q4 2024.
The AMA also spent $24 million in 2024, up from $21 million in 2023.
- The physicians group also increased spending by about $1.3 million from Q3 to Q4 2024. It was active not only on Medicare pay but on including prior authorization reforms in a year-end package.
Context: Republicans and Democrats spent weeks negotiating a massive end-of-year health package deal that included major PBM reforms as well as a crackdown on drug "patent thickets" that backers say drugmakers use to forestall competition from generics.
- The pharmaceutical industry has long been pushing for reforms to PBMs' practices, blaming the companies for high drug costs. The group also didn't want changes to drug patents, arguing they would squelch innovation.
- PBMs, meanwhile, argue that they're controlling costs in a convoluted health system and have been lobbying against such reforms for several years.
- In the end, most of the health provisions were dropped after President Trump came out against a large year-end bill.
Doctors groups were also pushing for a Medicare physician payment fix to be included in that package, as they frequently do at the end of the year.
- The original package contained a 2.5% increase in the Medicare physician fee payment schedule for 2025, which would have averted most of a scheduled cut.
- Physicians groups are intent on reviving the provision when the March funding deadline comes back up.
Between the lines: Major hospital trade associations reduced or kept their year-to-year spending constant in 2024 despite the threat of site-neutral payment policies that would have changed Medicare reimbursements for outpatient care.
- The American Hospital Association spent $24 million in 2024, down from $25 million in 2023.
- The Federation of American Hospitals spent about the same in both years: $2.4 million.
- One notable exception was America's Essential Hospitals, which represents safety net facilities and more than doubled its spending year over year. The group spent almost $5 million in 2024, compared with $1.8 million in 2023.
- All three hospital groups did increase spending in Q4 compared with the previous quarters of the year.
- Their concerns also included a "dishonest billing" measure that was in the initial end-of-year package and would have required off-campus providers to be assigned a unique identifier number. It, too, was dropped when the bill slimmed down.
The intrigue: Pharmaceutical company Novo Nordisk, which faced scrutiny all last year from former Senate HELP Chair Bernie Sanders over the price of its GLP-1 drugs Ozempic and Wegovy, upped its year-over-year spending by about a million.
- The Danish pharma giant spent $5.3 million in 2024, up from $4.2 million in 2023.
