Axios Vitals

October 15, 2025
It's already Wednesday. Today's newsletter is 1,060 words, a 4-minute read.
- Got a news tip? Reach us on Signal at Petersu.98, TinaReed.202 or MayaGold.57.
1 big thing: Rate shopping intensifies ACA drama
Premium increases are starting to hit home for millions of Americans as state-run Affordable Care Act marketplaces begin posting rates for next year that are based on the assumption Congress won't renew expiring financial assistance.
Why it matters: Sticker shock could lead many Americans to conclude health coverage is out of reach while the government remains in a shutdown that centers on the fate of enhanced ACA subsidies that will sunset at year's end.
Driving the news: "Window shopping," when ACA enrollees can preview their premiums for next year, is already underway in a half dozen states and begins today in California, Kentucky, Maine, New Mexico, Oregon and Vermont.
- In Idaho, the actual enrollment for 2026 coverage also begins today. Signs-ups begin November 1 for the rest of the country.
- Democrats are already seizing on early examples of premium increases to prod Republicans to extend the subsidies. Sen. Raphael Warnock (D-Ga.) posted on X a potential premium increase, sent to him by a constituent, from $307 per month to $964 per month. The post has 6.5 million views.
- On average, premiums for roughly 22 million ACA enrollees will more than double without a subsidy extension, per KFF.
What they're saying: Brad Woodhouse, president of the Democratic-aligned group Protect Our Care, said the group has created a toolkit to allow lawmakers to post examples similar to Warnock's and drive home the point that the pain has arrived.
- "I think after tomorrow when this window shopping starts to open, and you start to see this data trickle out, I think it's going to put Republicans in a tremendous bind," Woodhouse said yesterday.
The other side: Republicans say they are open to talks about extending the enhanced ACA subsidies in a modified form, but not as a precondition for reopening the government, as Democrats insist it should be.
2. CDC cuts put injury tracking in limbo
The job of tracking the ravages of the opioid crisis may come down to a bare-bones team of about 150 CDC workers whose overdose division survived a mass firing that took out much of the National Center for Injury Prevention and Control last week.
Why it matters: The injury center is a microcosm of the fractured landscape at the agency, which has lost about a quarter of its employees this year through successive Trump administration force reductions.
- The cuts announced on Friday rippled through the entire federal health bureaucracy, including at the nation's mental health and substance use office and among key biodefense staff. But confusion reigned, as more than half of the targeted workers later had their terminations rescinded.
- "There is no transparency. We still have no idea why certain programs, including mine, were eliminated and others were saved," Aryn Melton Backus, formerly with the CDC's Office on Smoking and Health, told reporters yesterday.
- She said she received her third reduction in force notice this year on Friday.
State of play: The injury center has about 250 people left out of roughly 700 it had at the start of the year, according to a source who was granted anonymity to reveal internal agency details.
3. States expand fertility coverage for cancer survivors
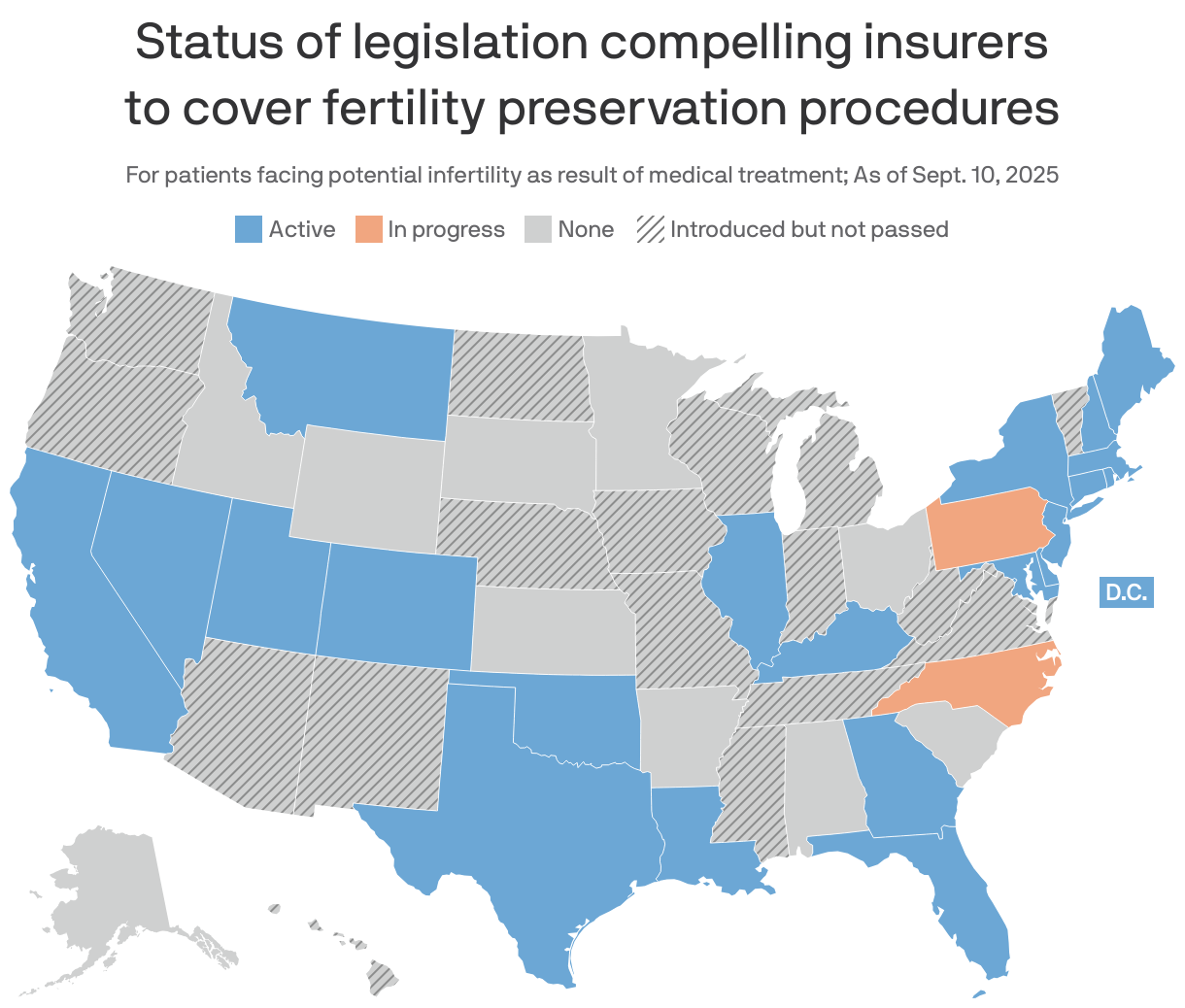
A wave of new state laws is making fertility preservation procedures — from egg freezing to the emerging ovarian tissue freezing technology — a covered benefit for cancer patients.
Why it matters: Chemotherapy and radiation can cause reproductive problems, but fertility preservation procedures are costly and can be left out of cancer treatment conversations.
State of play: As more Americans survive cancer at younger ages and delay parenthood, demand for oncofertility care — a field bridging oncology and reproductive medicine — is rising.
By the numbers: 21 states and Washington, D.C., now require insurers to cover fertility preservation for medical reasons, per the Alliance for Fertility Preservation.
- There was legislative action this year in Georgia, Virginia and New York, and executive director Joyce Reinecke tells Axios she's "hopeful" that laws are passed in Hawaii and Washington next.
Between the lines: Coverage rules vary by state, including which insurers must comply, which procedures are included, and which diagnoses qualify patients for coverage.
- "Experimental" procedures are rarely covered by insurance.
Established fertility preservation options include freezing eggs or embryos, the most common approach for women; and freezing sperm, standard for men.
What we're watching: The American Society of Clinical Oncology has expanded its fertility preservation guidelines, and the American Society for Reproductive Medicine is expected to update its guidelines soon, which could push more insurers to cover services.
4. Many GLP-1 prescriptions go unfilled: Study
About 40% of prescriptions for GLP-1 drugs went unfilled in a study of nearly 10,000 orders in the University of Colorado health system, with Black and Hispanic patients less likely to get the medicines.
Why it matters: The findings in JAMA Network suggest significant disparities and barriers to access exist despite a surge of GLP-1 prescribing.
What they found: Overall, 60.1% of GLP-1 prescriptions written in the health system between January 2018 and September 2022 were filled.
- The fill rate for white patients was 60.9%, compared with 55.3% for Black patients and 58.4% for Hispanic patients.
- Out-of-pocket costs for a 30-day supply varied, with Black and Hispanic patients paying less ($41.15 and $63.69, respectively) compared with white patients ($78.37).
- Costs for patients with obesity alone were nearly twice those for patients with diabetes, likely reflecting less comprehensive insurance coverage for the condition.
The big picture: The disparities are troubling, because patients in racial and ethnic minority groups have a higher prevalence of diabetes and obesity and can face institutional hurdles getting treatments, researchers wrote.
What we're watching: The Trump administration is reportedly considering a way to ease Medicare and Medicaid into covering GLP-1 drugs like Ozempic and Mounjaro for obesity starting as soon as next year.
5. Catch up quick
💊 Family members of President Trump and Commerce Secretary Howard Lutnick stand to benefit from the administration's efforts to overhaul prescription drug sales. (WSJ)
🤖 Mass General Brigham is addressing the shortage of primary care doctors with an AI app that questions patients, reviews medical records and produces potential diagnoses. (Boston Globe)
🥨 Big food companies are leaning into America's protein obsession and rebranding iconic snacks as functional fuel. (Axios)
Thanks for reading Axios Vitals, and to editors Adriel Bettelheim and David Nather and copy editor Matt Piper. Please ask your friends and colleagues to sign up.
Sign up for Axios Vitals







