Axios Vitals

October 13, 2022
Good morning, Vitals readers. Today's newsletter is 1,015 words or a 4-minute read.
1 big thing: Omicron boosters are now available for American kids. Many won't get them.
Illustration: Sarah Grillo/Axios
Pfizer's Omicron-specific COVID-19 vaccines are now available for kids as young as 5 years old.
- But while some parents will jump at the chance to get their children boosted, uptake of this version of the booster will likely remain low, unless there's a wintertime surge of new cases.
Why it matters: The updated shots, retooled to target the BA.5 strain that still accounts for most cases in the U.S., could provide some valuable protection for kids amid what's becoming a rough season for respiratory viruses.
- Already, RSV and enterovirus have surged among school-aged children, filling up U.S. emergency rooms and beds in children's hospitals, and officials have said they expect a severe flu season.
- As cold weather sends more people indoors, health officials also warn a new wave of COVID driven by stealthy new subvariants could also be on the way in the U.S., following trends in Europe.
- White House officials urged all eligible Americans to get a shot by Oct. 31 in order to be fully protected before the holidays, USA Today reported.
State of play: Nearly a year since the first COVID vaccines were approved for kids ages 5–11, parents continue to take a wait-and-see approach.
- About 9 million kids in that age group, or fewer than 1 in 3, have completed their primary series of COVID-19 vaccines, as of Oct. 5, according to the American Academy of Pediatrics.
- In comparison, 58% of kids 12-17 had completed their primary vaccine series.
- Even among adults, uptake of Omicron boosters has been soft. A recent Kaiser Family Foundation COVID-19 Vaccine Monitor found only 5% of adults had gotten the updated shot. Fewer than a third said they planned to get one as soon as possible.
Between the lines: Globally, uptake of COVID vaccines for kids has been spotty. Public health experts say delays resulted in them being launched at a time when the disease was no longer widely viewed as a crisis, Nature reported.
- "The case has not been adequately made about the significant number of deaths and hospitalizations among kids," said Peter Hotez, a pediatric vaccine scientist at Texas Children's Hospital in Houston, per Nature.
The bottom line: "Overall, the vaccination push will continue to be a long slog, perhaps only receiving a jolt if cases start to rise significantly and/or a new variant emerges that is more harmful," Jen Kates, Kaiser Family Foundation's director of global health and HIV policy, tweeted.
Related: Nearly half of COVID patients haven't fully recovered months later, study finds (New York Times)
2. Study: Paxlovid may interact with heart meds
Illustration: Sarah Grillo/Axios
Paxlovid can have severe interactions with some of the most common heart medications, complicating treatment options for cardiac patients at increased risk of developing severe COVID, according to a new study in the Journal of the American College of Cardiology, Axios' Arielle Dreher writes.
Why it matters: Hospitalized COVID patients are at increased risk of facing major cardiovascular problems and could benefit from the antiviral pill. But doctors have to be aware of the potential adverse effects before they prescribe it.
What they found: Common blood thinners and statins used to control blood pressure and cholesterol levels should not be taken with Paxlovid, researchers found. Their conclusions are based on data on drug-drug interactions and not on any adverse events reported.
- The study includes a detailed matrix of what types and which specific kinds of heart disease medications have known reactions.
- Paxlovid has been shown to prevent hospitalization and death among older, unvaccinated patients as well as vaccinated patients with heart conditions, according to study author Sarju Ganatra, who leads the cardio-oncology program at Lahey Hospital & Medical Center.
- Applying drug-drug interactions to electronic medical records could help avoid adverse events, Ganatra said in a statement.
3. Insurers predict 10% health cost hikes globally
Inflation should drive health benefit costs about 10% higher this year — the biggest hike in 15 years, according to a global survey of health plans released today by Willis Towers Watson.
Driving the news: The survey of 257 insurers in more than 55 countries found more than three-fourths of companies surveyed say it's going to be an especially costly next three years.
Between the lines: Leading cost-drivers included "overuse of care" (74%) followed by poor health habits (52%.) The insurers also cited underuse of preventative services, particularly during the pandemic.
- The payers also identified cancer, cardiovascular, and musculoskeletal as the top three conditions by cost.
- Insurers ranked contracted networks of providers (70%) as the most effective method for managing costs.
4. Data du jour: Kidney disease and diabetes
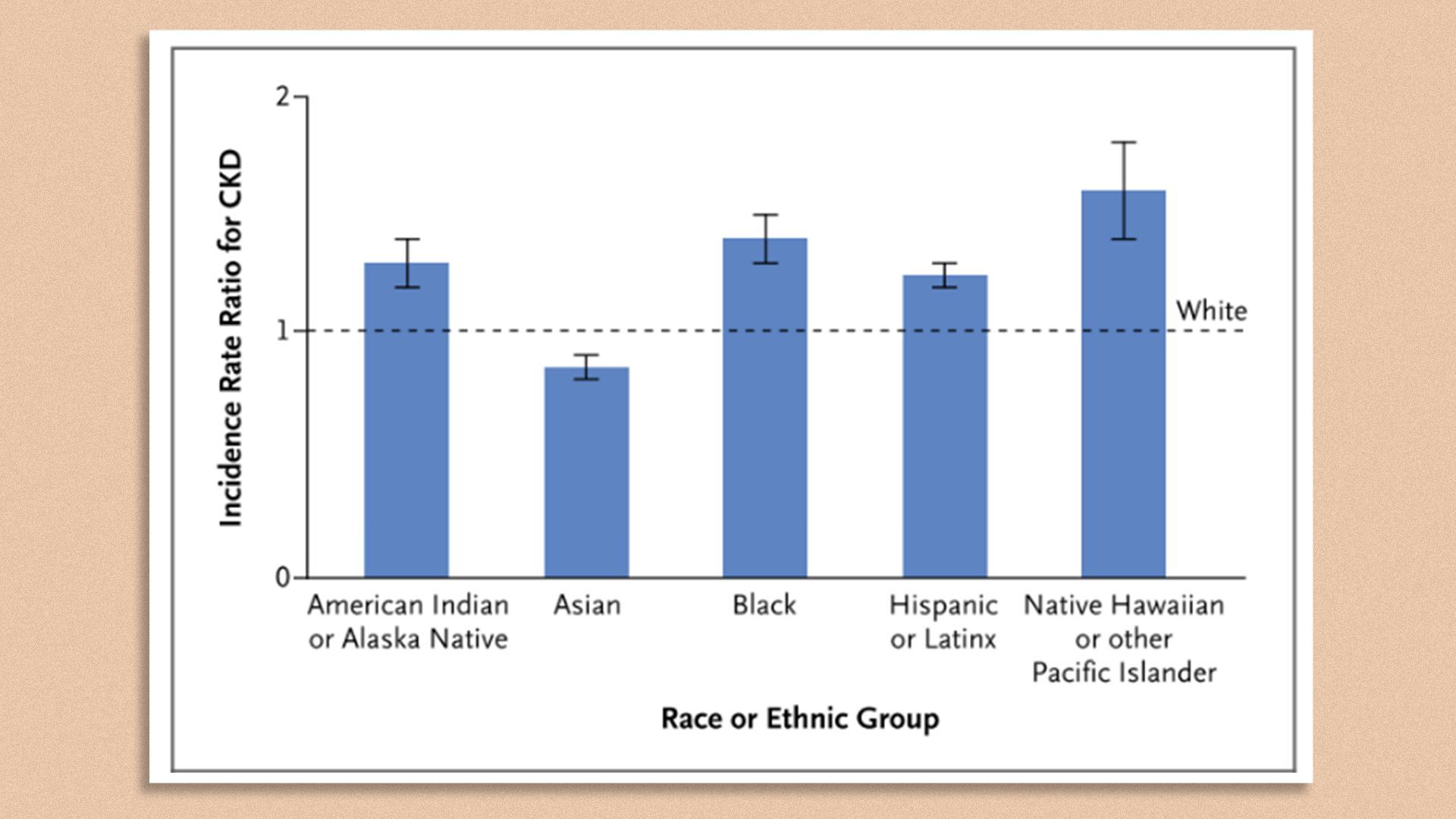
Incidence rate ratios for chronic kidney disease (CKD) among 654,459 patients in the Providence and UCLA health systems with diabetes between 2015 and 2020. Dashed line represents incidence rate ratio among white patients. Chart: Tuttle et al. "Incidence of Chronic Kidney Disease among Adults with Diabetes, 2015-2020" in the New England Journal of Medicine
Despite recent progress, there's still a high incidence of chronic kidney disease among adults with diabetes, particularly in minority communities, Arielle writes about a new analysis in the New England Journal of Medicine.
Driving the news: The review of more than 650,000 patient records found that Native Hawaiian, Pacific Islander, Black, Native American and Hispanic patients with diabetes had disproportionately higher rates of chronic kidney disease than white patients.
- Diabetes is the leading cause of kidney failure and resulting transplants or dialysis in the U.S., and the number of new diabetes patients is projected to increase in the coming decades.
Zoom in: Researchers examined electronic health records from Providence and UCLA patients from 2015 to 2020 to see how many with diabetes clinically progressed to chronic kidney disease.
- Rates were 60% higher in Pacific Islanders and Native Hawaiians than whites; 40% higher in Blacks; 33% higher in American Indians and 25% higher in Hispanic people.
- Less than 10% of patients who had early-stage kidney disease were aware of it, lead author Katherine Tuttle told Axios.
- "It's important, serious and treatable," she said.
5. Catch up quick
💊 Teva, the largest manufacturer of the ADHD drug Adderall in the U.S., told regulators a shortage of the drug may last through March. (Bloomberg)
💧Amid what is already a humanitarian crisis, Haiti is now suffering from an outbreak of cholera and could face threats from other diseases, Reuters reports.
🛩 A new nonprofit is connecting pilots of small airplanes with people seeking access to abortion and gender-affirming care. (Axios)
💰 Hospitals, boosted by private equity-backed staffing companies, have embraced a new idea: the obstetrics emergency department — and it comes with emergency department bills, too. (KHN)
Thanks for reading, and thanks to senior editor Adriel Bettelheim and senior copy editor Bryan McBournie for the edits. Please ask your friends and colleagues to sign up.
Sign up for Axios Vitals

Healthcare policy and business analysis from Tina Reed, Maya Goldman, and Caitlin Owens.