How dengue makes the immune system the enemy
Add Axios as your preferred source to
see more of our stories on Google.
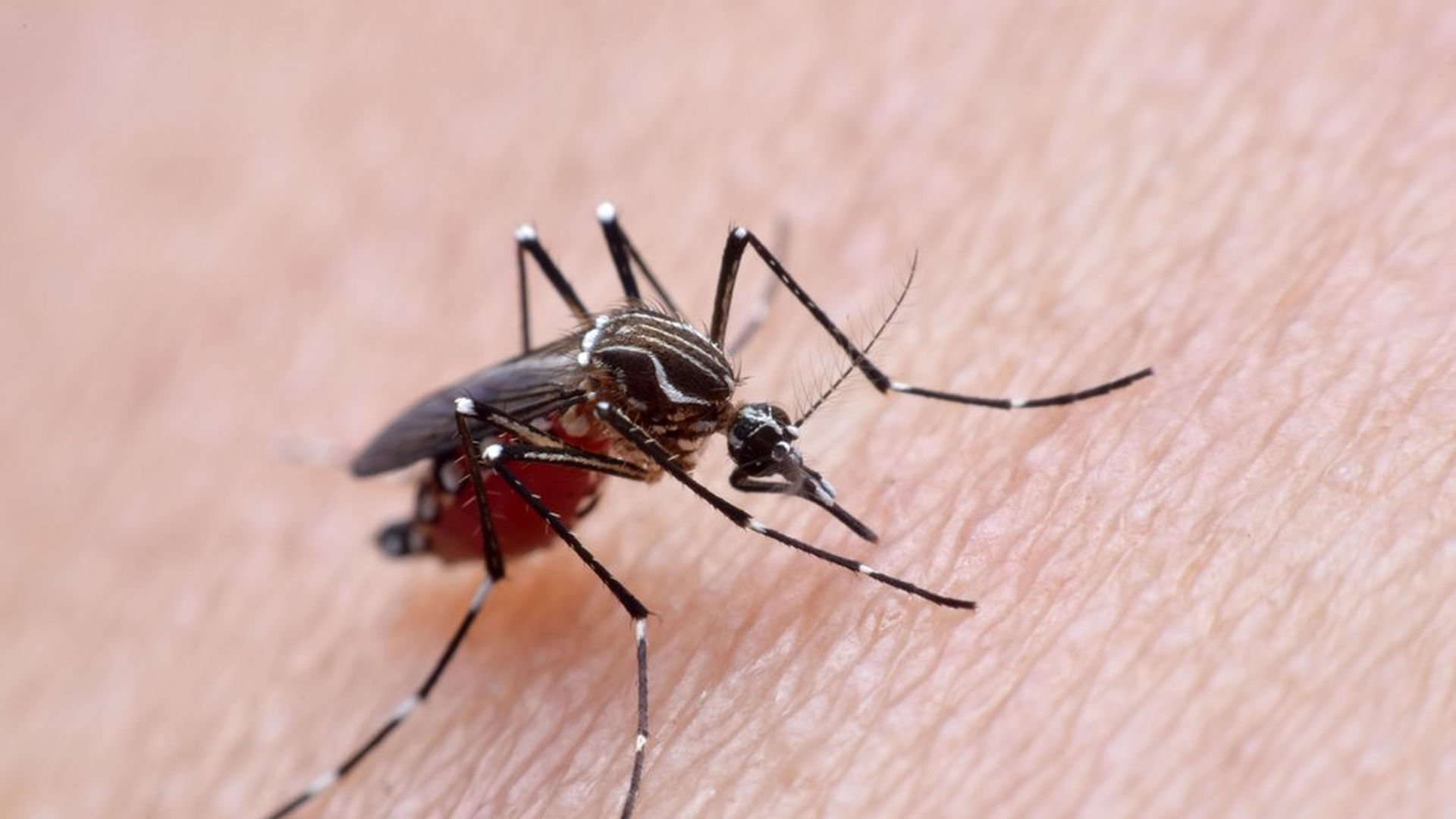
Aedes aegypti mosquito. Photo: iStock / Oistock89
When someone gets sick, their body learns what the virus looks like, and destroys it upon re-infection. But when someone is infected with dengue a second time, the immune system appears to help the virus cause a more severe and fatal illness. Previously only seen in the lab, a new study published Thursday in the journal Science shows a direct link between the dengue antibodies themselves and severe illness in humans, supporting a 40-year-old theory.
Why it matters: Dengue fever infects as many as 390 million people each year, up to 96 million of whom will experience symptoms. For most, access to medical treatment makes dengue survivable. But for a small fraction of victims, the virus can progress from a normal infection to a life-threatening hemorrhagic illness in less than a day. A better understanding of how and why this happens could save thousands of lives.
Some background: Dengue is closely related to — and carried by the same mosquitoes as — Zika, chikungunya, and yellow fever. There are four circulating flavors, or serotypes, of dengue. Infection with one type grants immunity to that strain. But a secondary infection with a different dengue virus can lead to dengue hemorrhagic fever or dengue shock syndrome, more severe forms of the disease. Since immune responses make it worse, scientists are concerned about how vaccines and infections from related viruses could influence a dengue infection.
Why it happens: Although scientists agree that a secondary dengue infection is more severe than the first, and that the immune system is involved, the mechanism is debated. The most widely accepted theory is antibody-dependent enhancement, first proposed 40 years ago, which works like this:
- An individual gets infected with one dengue virus type.
- They then get infected with a second, different serotype.
- The immune system recognizes the second dengue enough to respond, but doesn't send the right immune cells to take it down.
- These antibodies instead inadvertently help the dengue virus enter human immune cells and reproduce more easily.
- The body then mounts an over-the-top immune response, or cytokine storm. Normally cytokines cause disease-fighting inflammation, but with dengue the response can cause hemorrhage and shock.
Until now it was unknown what level of immune response and immune cells was necessary to trigger this reaction, although tests in the lab suggested there would be a 'sweet spot' for illness.
Past research has suggested that dengue vaccines in people who had never experienced dengue before can increase the risk of severe illness. The World Health Organization recommends the dengue vaccine only be given to children over 9 in areas where diseases levels are high. That means most vaccine recipients will already have some level of immunity.
What they did: The researchers used data from a longitudinal study of over 8,000 Nicaraguan children, 6,600 of whom had antibodies for dengue, and took yearly blood samples. They divided the children into four groups based on the levels of dengue-binding antibodies present in their blood measured via a simple assay. Then, they looked at the future risk of naturally occurring dengue infection developing into dengue hemorrhagic fever or dengue shock syndrome.
What they found: Children with high levels of the antibodies and children who had never had dengue had the same, low risk of developing severe dengue. But children with a specific range of antibodies were 7.64 times more likely to develop severe illness.
There are a few practical implications of this research.
- Study author Eva Harris imagines, potentially, a future where assays of dengue antibody levels are a normal part of yearly medical exams. If someone becomes re-infected with dengue, they can look at the pre-existing antibody levels and predict the risk of severe dengue developing, and preventatively hospitalize the patient.
- Past research has shown the dengue vaccine can increase the risk of severe dengue in those who have never been infected. It's possible antibody levels could be used to predict who would benefit most from the expensive vaccines, and who should wait to receive them.
Remaining questions: Research has shown dengue severity can be influenced by which serotypes are circulating, and the order of infection. This study didn't look at the response to specific serotypes only antibody levels. And, while this study has shown a strong predictive correlation between antibody levels and severe dengue, more research is needed before anything definitive can be said.
