Nov 8, 2018
Feds propose rolling back Medicaid's doctor network requirements
Add Axios as your preferred source to
see more of our stories on Google.
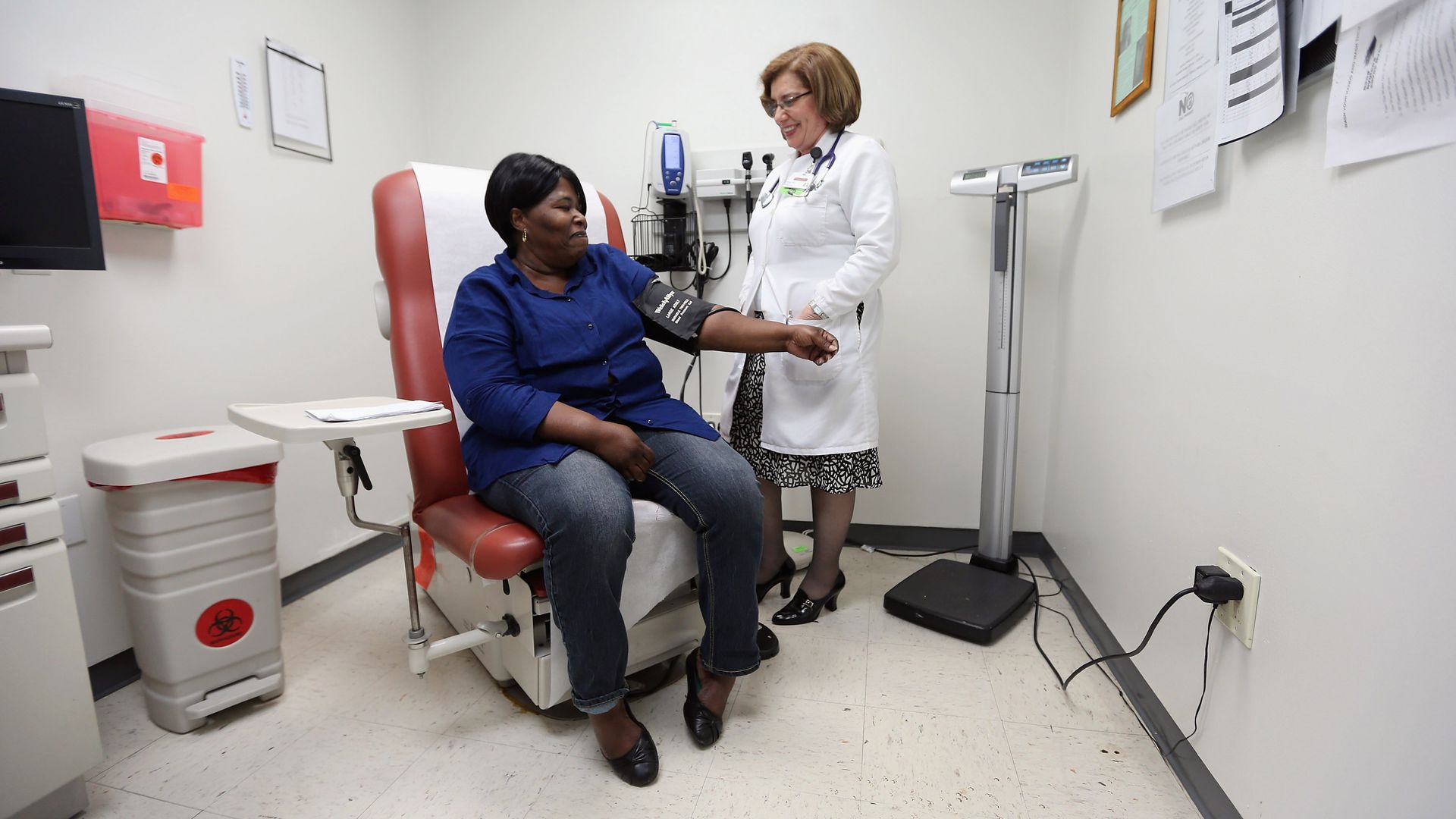
A new proposal would eliminate rules around Medicaid doctor networks. Photo: Joe Raedle/Getty Images
